Late Effects Basics - Time's Toll
- Appear > 6 months (or > 90 days) post-exposure.
- Classification:
- Deterministic (Tissue Reactions): Severity ↑ with dose; threshold dose exists. E.g., fibrosis, cataracts.
- Stochastic: Probability ↑ with dose; no threshold. E.g., cancer, heritable effects.
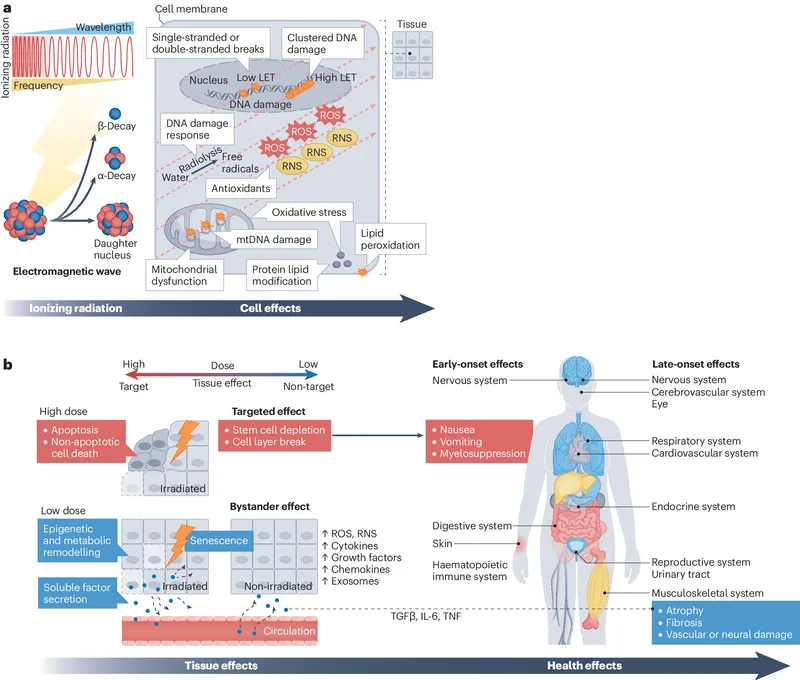
- Pathophysiology:
- Cell death (reproductive sterilization).
- Vascular damage (endothelial cell loss, stenosis).
- Chronic inflammation & fibrosis.
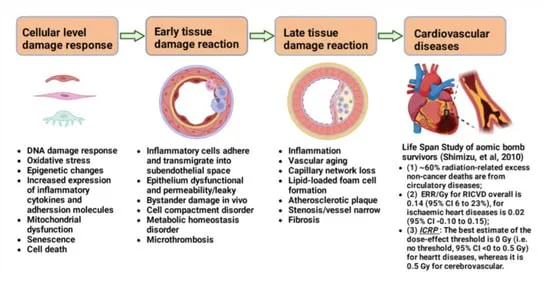
⭐ Most late deterministic effects are characterized by a threshold dose below which they are not observed, and severity increases with dose above the threshold.
Organ Systems Hit - The Aftermath
| Organ | Late Effect | Latency | Key Threshold Dose (TD5/5 or critical) |
|---|---|---|---|
| CNS | Necrosis, Myelopathy (Lhermitte's) | Months-Years | Spinal Cord: ~50 Gy |
| Lung | Pneumonitis → Fibrosis | Months-Years | Pneumonitis: ~17.5 Gy (whole) |
| Heart | Pericarditis, Cardiomyopathy, CAD | Years | Pericarditis: ~40 Gy (whole) |
| Kidney | Nephropathy | >6 Months | ~23 Gy (whole) |
| Lens | Cataract | Months-Years | ~2 Gy (single), ~5 Gy (fract.) |
| Gonads | Sterility, Premature Ovarian Failure | Variable | Ovaries: ~2-3 Gy; Testes: ~5-6 Gy |
| Skin | Fibrosis, Telangiectasia | Months-Years | Telangiectasia: >50 Gy |
| Bone | Necrosis, Impaired Growth (child) | Months-Years | Necrosis: >60 Gy |
Chance & Change - Cancer & Genes
-
Radiation Carcinogenesis
- Mechanism: DNA damage (direct/indirect) → mutations, genomic instability → cancer development.
- Dose-response: Linear No-Threshold (LNT) model used for radiation protection purposes (stochastic effects).
- Latency Period: Time from exposure to diagnosis; variable.
⭐ Radiation-induced leukemias (excluding CLL) typically have a shorter latent period (average 5-10 years) compared to solid tumors (typically 10-30 years or more).
-
Common Radiation-Induced Malignancies
- Leukemia: AML, CML; peak incidence 5-7 years. (📌 Leukemia Latency Low: 5-7 yrs)
- Thyroid Cancer: Papillary type common, esp. in children.
- Breast Cancer, Lung Cancer, Skin Cancer (BCC, SCC), Bone Sarcoma.
-
Heritable (Genetic) Effects
- Definition: Radiation-induced mutations in germ cells (sperm/ova) transmitted to offspring.
- Types: Gene mutations, structural/numerical chromosomal aberrations.
- Doubling Dose: Dose doubling spontaneous mutation rate; estimated ~1 Gy for humans.
- Human Evidence: No conclusive evidence of increased heritable effects in A-bomb survivors' offspring to date.
Factors & Modifiers - Influencing Variables
- 📌 5 R's of Radiobiology: Modulate tissue response.
- Repair: Crucial for late effects; late-responding tissues ↑ repair (low $\alpha/\beta$ ratio).
- Repopulation: Cellular proliferation.
- Redistribution: Progression of cells through the cell cycle.
- Reoxygenation: Improved oxygen status of hypoxic cells.
- Radiosensitivity: Inherent sensitivity of cells.
- Major Influencing Factors:
- Total Dose: Primary factor. ↑ dose → ↑ severity.
- Fractionation:
⭐ Fractionation generally spares late-responding tissues (greater repair capacity, low $\alpha/\beta$ ratio, typically 2-3 Gy) more than early-responding tissues.
- Dose Rate: ↓ rate usually ↓ late effects.
- Volume Irradiated: ↑ volume → ↑ risk/severity.
- Radiation Quality (LET/RBE): Higher LET can ↑ late effects.
- Age at exposure: Children often more sensitive to certain late effects.
- Individual Sensitivity: Genetic factors (e.g., Ataxia Telangiectasia).

High‑Yield Points - ⚡ Biggest Takeaways
- Late effects: deterministic (have a threshold dose, e.g., fibrosis, cataracts) and stochastic (no threshold, e.g., cancer).
- Severity of deterministic effects is dose-dependent; probability of stochastic effects is dose-dependent.
- Key late tissue reactions include fibrosis, atrophy, vascular damage, and necrosis.
- Secondary malignancies (e.g., leukemia, solid tumors) are a major concern, often with long latency periods.
- The lens of the eye (cataracts), thyroid gland, and bone marrow are particularly sensitive to late effects.
- Fractionation significantly spares late-responding normal tissues, thereby reducing late adverse effects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

