Cell Survival Curves - Curveballing Survival
-
Definition: Plots cell survival (reproductive integrity) vs. radiation dose.
-
Axes: Y-axis: log Surviving Fraction (SF); X-axis: Dose (Gy).
-
Purpose: Quantifies radiation-induced cell kill; compares radiosensitivity.
-
Key Parameters:
- SF (Surviving Fraction): $SF = N/N_0$; cells retaining reproductive ability.
- D₀ (Mean Lethal Dose): Dose reducing SF to 37% ($1/e$) on exponential part. ↓D₀ = ↑radiosensitivity.
- Dq (Quasi-threshold Dose): Width of shoulder. Dose where extrapolated linear portion intersects SF=1. Indicates Sublethal Damage (SLD) repair.
- n (Extrapolation Number): Y-intercept of curve's straight part (at dose=0). Reflects shoulder width, SLD repair.
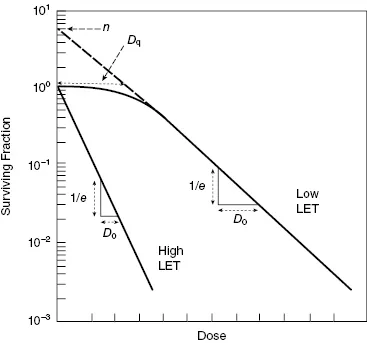
⭐ D₀ represents the dose required to reduce the surviving fraction to 37% on the exponential part of the curve.
Models of Cell Kill - Target Practice Time
- Linear-Quadratic (LQ) Model: Describes cell survival after radiation.
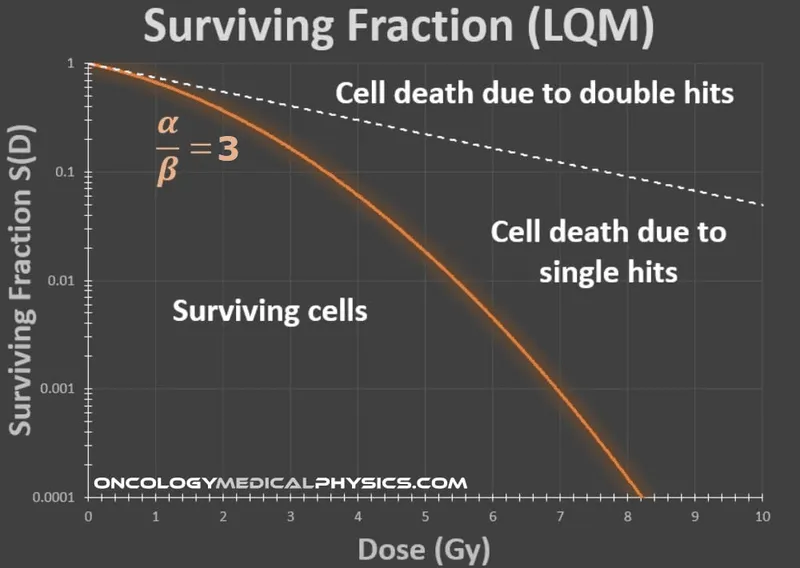
- Survival Fraction (SF): $SF = e^{-(\alpha D + \beta D^2)}$
- α component: Irreparable damage (single hit), linear, dominant at low doses.
- β component: Repairable damage (two hits/misrepair), quadratic, dominant at high doses.
- α/β ratio: Dose where linear & quadratic effects are equal.
⭐ The α/β ratio is high (≈10 Gy) for most tumors and acutely responding tissues, and low (≈3 Gy) for late-responding normal tissues.
- Target Theory: Older models.
- Single-target single-hit: One critical target; one hit inactivates. Exponential survival.
- Multi-target single-hit: Multiple targets; each needs one hit. Shoulder on survival curve.
 an
an
Influencing Factors - Survival Mod Squad
Key factors modifying cellular radiation response:
- The 4 R's of Radiobiology 📌:
- Repair (sublethal damage)
- Repopulation (cell division)
- Redistribution (cell cycle phases)
- Reoxygenation (of hypoxic cells)
- Physical Factors:
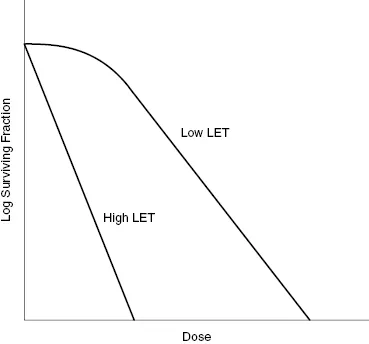
- LET (Linear Energy Transfer): ↑LET → ↑RBE, ↓OER, straighter survival curve (less shoulder).
- RBE (Relative Biological Effectiveness): Measures relative damage.
- Dose Rate: ↓Dose rate allows more repair → ↑survival.
- Chemical Factors:
- Oxygen Effect (OER): $OER = \text{Dose in hypoxia} / \text{Dose in aerated conditions for same biological effect}$.
- X-rays/γ-rays: OER 2.5-3.5.
- Neutrons: OER ~1.6. High LET (α-particles): OER ~1.0.
- Radiosensitizers (e.g., Misonidazole, Cisplatin): Enhance tumor cell kill.
- Radioprotectors (e.g., Amifostine): Protect normal tissues.
- Oxygen Effect (OER): $OER = \text{Dose in hypoxia} / \text{Dose in aerated conditions for same biological effect}$.
- Biological Factors:
- Cell Cycle Phase:
⭐ Cells in M and G2 phases are most radiosensitive, while late S phase cells are most radioresistant.
- Intrinsic Radiosensitivity: Cell-type specific.
- Repair Capacity: SLDR (Sublethal Damage Repair), PLDR (Potentially Lethal Damage Repair).
- Cell Cycle Phase:
Clinical Applications - Healing Rays Playbook
- Fractionated radiotherapy: Spares normal tissues by exploiting the 4 R's (Repair, Reassortment, Repopulation, Reoxygenation). 📌
- Therapeutic Ratio/Window: Maximize tumor control, minimize normal tissue complications.
- Biologically Effective Dose (BED): Quantifies biological effect of different fractionation schemes.
- Formula: $BED = D \times (1 + d/(\alpha/\beta))$, where D=total dose, d=dose per fraction.
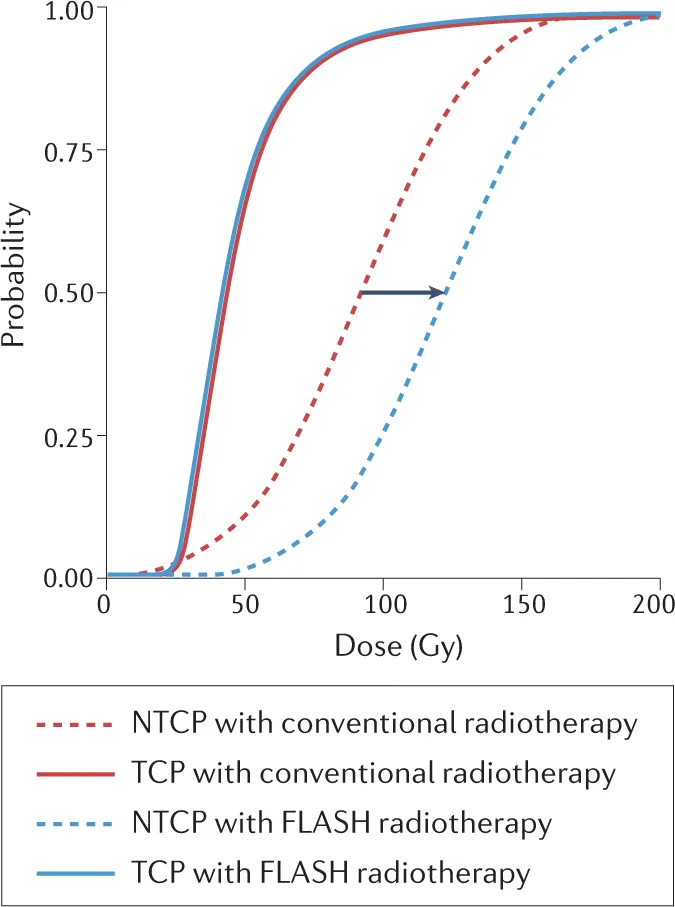
- Predicts Tumor Control Probability (TCP) and Normal Tissue Complication Probability (NTCP).
⭐ Fractionation exploits differences in repair capacity and α/β ratios between tumor cells and late-responding normal tissues.
High‑Yield Points - ⚡ Biggest Takeaways
- Cell survival curves plot surviving cell fraction against radiation dose.
- D0 dose: dose to reduce survival to 37% on the linear part; measures radiosensitivity.
- Shoulder (n, Dq): indicates sublethal damage repair (SLDR) capacity.
- Linear-Quadratic (LQ) model is key for modern radiotherapy and understanding dose response.
- α/β ratio: crucial for fractionation; high for tumors & acute effects, low for late-responding tissues.
- Oxygen effect: OER ~2.5-3.5 for low-LET; hypoxic cells are significantly more radioresistant.
- High LET radiation (e.g., alpha particles, neutrons): produces steeper survival curves with a reduced or absent shoulder and lower OER_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more