Biodosimetry Basics - Radiation's Fingerprints
-
Definition: Biological dosimetry (biodosimetry) estimates radiation dose by measuring quantifiable biological changes in irradiated individuals.
-
Purpose:
- Assess dose in accidental exposures.
- Guide medical management.
- Reconstruct dose retrospectively.
-
Principles: Relies on dose-dependent biological endpoints (e.g., chromosome aberrations, gene expression changes). The magnitude of the biological response correlates with the absorbed dose.
-
Comparison with Physical Dosimetry:
- Physical Dosimetry: Measures dose directly using dosimeters (e.g., TLDs). Provides immediate, precise readings if present.
- Biological Dosimetry: Measures dose effect on the body. Useful when physical dosimeters are absent/unreliable or for retrospective assessment.
⭐ Biological dosimetry complements physical dosimetry, especially when physical dosimeters are absent or unreliable, or for retrospective dose assessment.
Cytogenetic Assays - Chromosome Checkup
Cytogenetic assays quantify radiation dose by analyzing chromosomal damage in peripheral blood lymphocytes. These are key tools in biological dosimetry.
⭐ The Dicentric Chromosome Assay (DCA) performed on peripheral blood lymphocytes is considered the 'gold standard' for assessing recent acute whole-body radiation overexposure.
Key assays include:
| Feature | Dicentric Chromosome Assay (DCA) | Micronucleus Assay (MN) | FISH (Translocations) |
|---|---|---|---|
| Principle | Dicentric chromosomes | Micronuclei | Stable translocations |
| Sample | Lymphocytes | Lymphocytes (cytokinesis-blocked) | Lymphocytes |
| Time Window | Days-weeks (unstable) | Days-weeks (unstable) | Months-years (stable) |
| Dose Range | ~0.1-5 Gy | ~0.2-5 Gy (up to 10 Gy) | From ~0.1 Gy (retrospective) |
| Pros | Gold standard (recent) | Rapid, simpler | Retrospective, cumulative |
| Cons | Laborious, fades | Less specific | Complex, expensive |
Assay Utility Timeline Post-Exposure:
Advanced & Rapid Assays - Speedy Signals
- γ-H2AX Foci Assay:
- Rapid (minutes to hours), sensitive DNA double-strand break (DSB) marker.
- Application: Early triage, dose estimation.
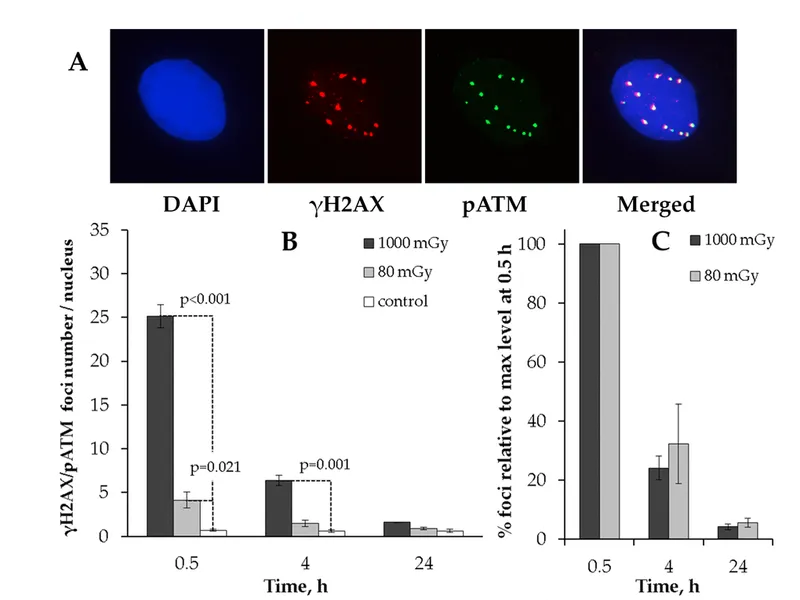
⭐ γ-H2AX foci formation is a rapid and sensitive early biomarker of DNA double-strand breaks, useful for triage in mass casualty radiological events.
- Gene Expression Profiling:
- Assesses changes in gene activity (e.g., GADD45, FDXR).
- Application: Triage, dose (esp. <2 Gy); results in hours.
- Proteomics:
- Analyzes protein alterations (e.g., C-reactive protein, Flt3 ligand).
- Use: Dose estimation, radiosensitivity prediction.
- Electron Paramagnetic Resonance (EPR):
- Detects free radicals in tooth enamel, nails.
- Application: Retrospective dosimetry.
- Optically Stimulated Luminescence (OSL):
- Measures dose from fortuitous materials (phone screens, salt, sugar).
- Application: Rapid population screening.
Application & Dose Interpretation - Reading Results
- Core Applications:
- Radiation accidents (individual, mass casualties).
- Occupational exposure monitoring.
- Radiotherapy dose verification & accidents.
- Triage in large-scale radiological events.
- Dose-Response Calibration Curves:
- Essential for dose estimation.
- Constructed using known doses & biological endpoints (e.g., dicentrics).
- Formula: $Y = C + \alpha D + \beta D^2$ (Y=yield, C=background, D=dose).
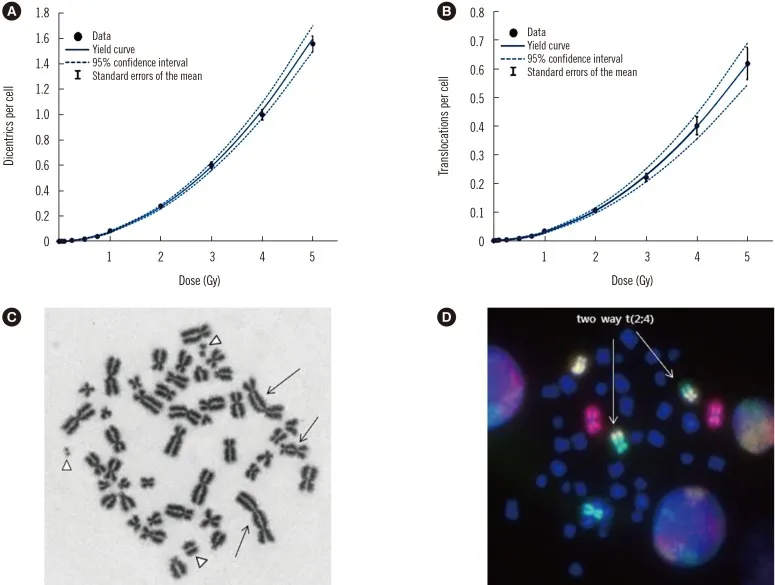
- Factors Influencing Dose Estimation:
- Exposure type: Partial vs. whole-body, uniform vs. non-uniform.
- Radiation quality (LET).
- Time since exposure (dicentrics stable for years, micronuclei less so).
- Inter-individual variability (age, genetics).
- Medical history (chemo/radiotherapy).
- Confounding factors: Smoking, viral infections, medications.
⭐ Accurate biodosimetry requires well-established calibration curves specific to the radiation type and exposure conditions, and careful consideration of confounding factors.
High‑Yield Points - ⚡ Biggest Takeaways
- Dicentric Chromosome Assay (DCA): Gold standard using lymphocytes; best for recent, acute exposures.
- Dicentrics: Unstable, radiation-specific. Translocations: Stable, for retrospective dosimetry (e.g., FISH).
- Micronucleus assay: Simpler, faster than DCA; less sensitive at low doses (<0.1 Gy).
- γ-H2AX foci: Early DNA damage marker (DSBs); useful for rapid triage.
- EPR (tooth enamel): For long-term retrospective dosimetry (accidents, chronic exposure).
- Effective dose range for cytogenetics: 0.1 Gy to 5 Gy.
- PCC assay: For very high doses (>5 Gy) or non-dividing cells.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

