ARS Basics - Radiation's Rude Jolt
- Definition: Acute illness from whole-body/significant partial-body exposure to high-dose penetrating radiation over a short period.
- Nature: Deterministic effect; severity ↑ with dose. A threshold dose must be exceeded.
- Radiation Types: Gamma rays, X-rays, neutrons.
- Symptom Onset:
⭐ Whole-body absorbed dose > 1 Gy (100 rads) is generally required to produce symptoms of ARS.
- Key Factors: Total dose, dose rate, body area exposed, radiation quality, individual sensitivity.
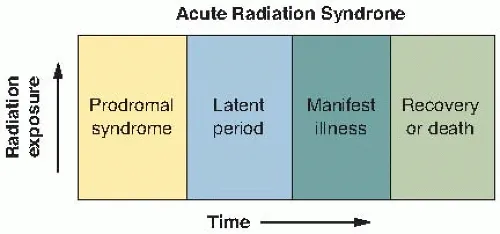
ARS Phases & Dose - Timeline of Trouble
- 1. Prodromal Phase:
- Onset: Mins-hrs post-exposure.
- Symptoms: NVD (Nausea, Vomiting, Diarrhea), fatigue.
- Dose: >1 Gy. Severity ↑ with dose.
- 2. Latent Phase:
- Apparent wellness. Duration: Hrs-wks.
- 3. Manifest Illness Phase: Specific syndromes.
- Hematopoietic (HP): 2-10 Gy. Infection, hemorrhage. Nadir ~3-4 wks.
- Gastrointestinal (GI): 6-10 Gy. Severe NVD, sepsis. Death ~2 wks.
- Neurovascular (NV)/CNS: >10-20 Gy. Rapid onset. Ataxia, seizures, coma. Fatal <48 hrs.
- 4. Recovery or Death:
- HP: Recovery possible. GI/NV: Often fatal.
⭐ The duration of the latent phase is inversely proportional to the radiation dose; higher doses lead to shorter or absent latent periods.
Core Syndromes - Systemic Shockwaves
-
Hematopoietic (Bone Marrow) Syndrome (HPS)
- Dose: ~0.7 - 10 Gy (mild from 0.3 Gy).
- Mechanism: Bone marrow stem cell destruction → pancytopenia.
- Nadir: Lymphocytes (1-2 days), Neutrophils (3-5 wks), Platelets (3-5 wks).
- Features: Infection (neutropenia), hemorrhage (thrombocytopenia), anemia.
- Outcome: Death at >2 Gy if untreated (infection/hemorrhage). Recovery possible.
- 📌 Mnemonic: Hematopoietic Problems Start (stem cells).
-
Gastrointestinal (GI) Syndrome (GIS)
- Dose: >6 - 10 Gy (overlaps severe HPS).
- Mechanism: Crypt cell death → mucosal denudation, villous atrophy → impaired absorption, barrier loss.
- Features: Severe N/V, bloody diarrhea, dehydration, electrolyte imbalance, sepsis.
- Outcome: Death in 2 wks (fluid/electrolyte loss, infection). Survival rare >10 Gy.
-
Neurovascular / Cardiovascular (NVS/CVS) Syndrome
- Dose: >20 - 30 Gy (effects >10 Gy; fulminant >50 Gy).
- Mechanism: Vasculitis, ↑capillary permeability, cerebral edema, direct neuronal/myocardial damage.
- Features: Rapid: severe N/V, disorientation, ataxia, seizures, coma, hypotension.
- Outcome: Uniformly fatal in hours to 3 days.
⭐ In the 2-10 Gy whole-body exposure range, the hematopoietic syndrome is dominant, and death, if it occurs, is typically due to infection and/or hemorrhage.

Diagnosis & Management - Battle Plan ARS
- Diagnosis:
- History of exposure.
- Clinical: Nausea, Vomiting, Diarrhea (NVD) onset time.
- Biodosimetry: Serial lymphocyte counts (key prognostic), cytogenetics (dicentrics).
- Management:
- Triage: Based on symptoms, dose estimation (lymphocyte kinetics).
- Decontamination: External/internal.
- Supportive Care: Fluids, antiemetics, antibiotics, transfusions.
- Cytokines: G-CSF/GM-CSF for doses > 2 Gy.
- Stem Cell Transplant (SCT): For doses > 6-8 Gy with severe marrow failure.
- Treat specific organ syndromes (GI, CVS, CNS).
⭐ A rapid fall in absolute lymphocyte count within the first 24-48 hours post-exposure is a key indicator of significant radiation dose and a poor prognostic sign.
High-Yield Points - ⚡ Biggest Takeaways
- Acute Radiation Syndrome (ARS) occurs after whole-body exposure >1 Gy.
- Key phases: Prodromal (NVD), Latent, Manifest Illness.
- Hematopoietic Syndrome (1-6 Gy): Lymphopenia is earliest; death via infection/hemorrhage.
- Gastrointestinal Syndrome (6-10 Gy): Crypt cell death leads to death by sepsis/fluid loss.
- Neurovascular Syndrome (>20-30 Gy): Rapid death from cerebral edema/vasculitis.
- Human LD50/60 is ~3-4 Gy without medical support.
- Early lymphocyte count drop is a crucial prognostic indicator and biodosimeter.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

