Shielding Fundamentals - Radiation's Kryptonite
- 📌 ALARA Principle: Minimize exposure (Time ↓, Distance ↑, Shielding ↑).
- Radiation Types & Shielding Needs:
- α (Alpha): Paper, skin.
- β (Beta): Plastic, Aluminium.
- X-rays & γ-rays: Lead (Pb), Concrete (high Z, high density).
- Neutrons: Water, Paraffin, Concrete (Hydrogen-rich).
- Attenuation: Intensity reduction ($I = I_0 e^{-\mu x}$); $\mu$ = linear attenuation coefficient.
- Half-Value Layer (HVL): Thickness reducing intensity by 50%. $HVL = 0.693/\mu$.
- Tenth-Value Layer (TVL): Thickness reducing intensity by 90%. $TVL = \ln(10)/\mu \approx 3.32 \times HVL$.
⭐ The TVL being approximately 3.32 times the HVL is a key calculation shortcut.
 oka
oka
Shielding Metrics - Numbers Game
- HVL (Half-Value Layer): Material thickness reducing radiation intensity by 50%. $HVL = 0.693 / \mu$.
- TVL (Tenth-Value Layer): Material thickness reducing radiation intensity by 90% (to 1/10th). $TVL = 2.303 / \mu$.
- $1 \text{ TVL} \approx 3.32 \text{ HVLs}$.
- Linear Attenuation Coefficient ($\mu$): Probability of photon interaction per unit length (cm⁻¹). Depends on energy, Z, density.
- Mass Attenuation Coefficient ($\mu/\rho$): $\mu$ normalized for density (cm²/g). More fundamental.
- Workload (W): Measure of radiation output (e.g., mA-min/week).
- Use Factor (U): Fraction of time beam is directed at a barrier.
- Occupancy Factor (T): Fraction of time an area is occupied.

⭐ For diagnostic X-rays, lead (Pb) HVL is typically < 0.5 mm at 80 kVp, while for Co-60 gamma rays (~1.25 MeV), lead HVL is ~1.25 cm.
Barrier Design - Building Fort Knox
- Goal: ALARA; keep exposures below weekly dose limits for staff & public.
- Barrier Types:
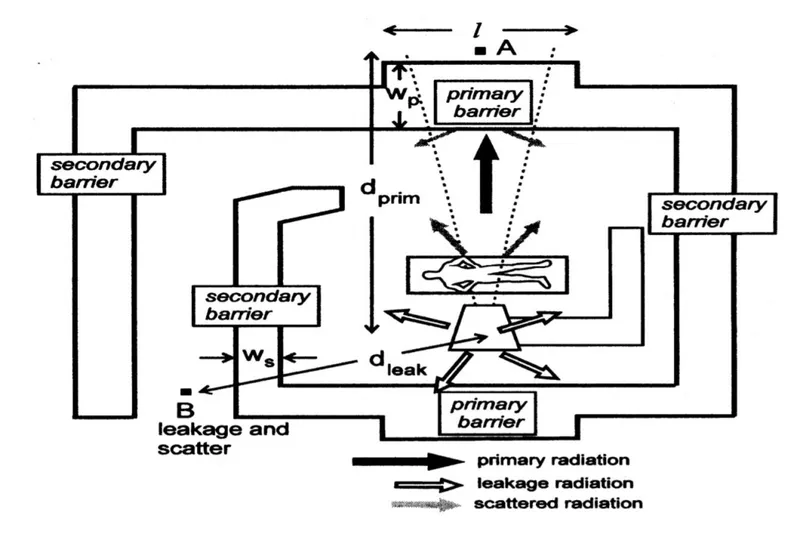
- Primary: Intercepts useful beam. Max shielding needed.
- Secondary: Shields scatter & leakage. Leakage: <1 mGy/hr @ 1m from housing.
- Shielding Factors ($B = P d^2 / (WUT)$):
- $P$: Permissible dose/wk (Controlled: 0.1 mSv; Uncontrolled: 0.02 mSv).
- $d$: Distance (source to occupied point).
- $W$: Workload (mA-min/wk), total tube output.
- $U$: Use factor (beam fraction at barrier).
- $T$: Occupancy factor (time area is occupied).
- Attenuation:
- HVL: Thickness reducing intensity by 50%.
- TVL: Thickness reducing intensity by 90% ($1 \text{ TVL} \approx 3.3 \text{ HVL}$).
⭐ Shielding calculations must account for workload (W), use (U), and occupancy (T) factors to avoid over/under-shielding.
Materials & Regs - Lead & Law
- Shielding Materials:
- High Z (e.g., Lead, Pb Z=82): Maximize photoelectric absorption.
- Cost-effective, widely used.
- Alternatives: Concrete, steel, barium plaster (Pb-equivalents).
- Half Value Layer (HVL): Thickness halving radiation intensity.
- Tenth Value Layer (TVL): Thickness reducing intensity by 90%.
- $TVL \approx 3.32 \times HVL$.
- High Z (e.g., Lead, Pb Z=82): Maximize photoelectric absorption.
- Regulations (AERB - India):
- Atomic Energy Regulatory Board (AERB): National regulatory body.
- Key Code: AERB/SC/MED-2 (Medical Diagnostic X-Ray Safety).
- Annual Dose Limits:
- Occupational: 20 mSv (avg/5 yrs), max 30 mSv/yr.
- Public: 1 mSv.
- Area Classification:
- Controlled Area: Potential > 6 mSv/yr.
- Supervised Area: Potential > 1 mSv/yr.
- 📌 ALARA: As Low As Reasonably Achievable.
⭐ AERB mandates type approval for X-ray equipment and regular Quality Assurance (QA).
High‑Yield Points - ⚡ Biggest Takeaways
- HVL and TVL are fundamental for shielding thickness; 1 TVL ≈ 3.3 HVL.
- Inverse Square Law (intensity ∝ 1/distance²) is critical for distance protection.
- Shielding design considers Workload (W), Use Factor (U), and Occupancy Factor (T).
- Primary barriers attenuate the direct beam; secondary barriers for scatter and leakage.
- Dose limits are stricter for uncontrolled areas (public) than controlled areas.
- Lead (Pb) and concrete are common materials, chosen based on radiation energy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

