Detector Fundamentals - Sparking the Science
- Radiation Detector: Converts radiation energy to a measurable signal for detection, measurement, identification.
- Key Performance Characteristics:
- Efficiency: Intrinsic (detector interaction %), Geometric (radiation reaching %).
- Dead Time: Unresponsive period. Paralyzable (any event extends it), Non-paralyzable (fixed duration after detected event).
- Energy Resolution: Distinguishes close energies (↓FWHM = better).
- Sensitivity: Minimum detectable radiation amount.
⭐ High dead time limits maximum count rate. Paralyzable detectors may show ↓ observed counts at high true rates, a critical limit_._
Gas-Filled Detectors - Counting the Charges
Principle: Radiation ionizes gas; an electric field collects charges. Voltage-Response Curve Regions (📌 R.I.P.L.G.C.):
- Recombination: Ions recombine.
- Ionization (Chamber): All charges collected.
- Proportional: Gas amplification; pulse size ~ energy.
- Limited Proportional: Non-linear amplification.
- Geiger-Müller (GM): Max amplification (avalanche).
- Continuous Discharge: Breakdown.
Types:
- Ionization Chambers: Current measurement (DC). Apps: dose calibrators, survey meters.
- Proportional Counters: Energy discrimination. Apps: α/β counting.
- GM Counters: High sensitivity, no energy info. 'Quenching' vital. Apps: contamination surveys.
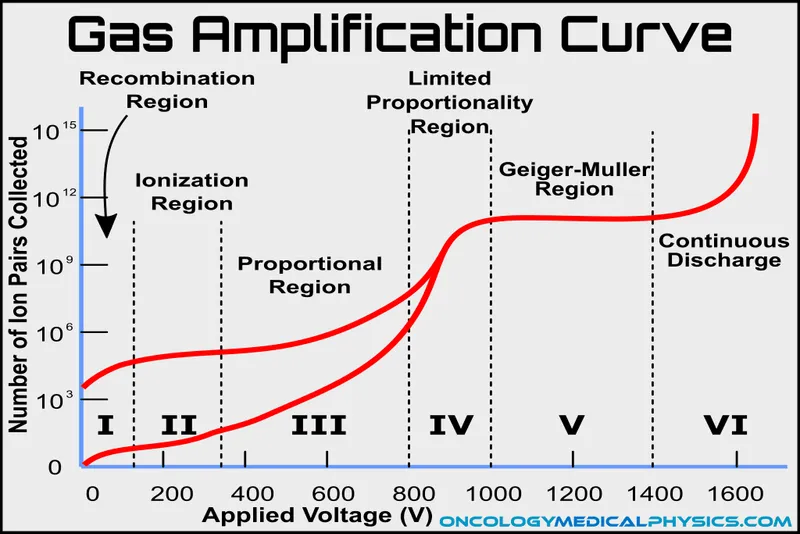
⭐ GM counters cannot distinguish radiation types or energies and have significant dead time.
Scintillators - Light Up the Count
- Principle: Radiation energy → light photons in scintillator → electrical signal via photodetector.
- Components:
- Scintillator Materials:
- Inorganic: NaI(Tl), CsI(Tl), BGO, LSO, LYSO. (📌 NaI Tali, CsI Tali, BiG Ones, Lutetium SOda)
- Organic: Plastic, liquid (for β-emitters).
- Photodetector: Photomultiplier Tube (PMT) (photocathode, dynodes, anode) or Photodiode.
- Scintillator Materials:
- Key Characteristics: Light output, decay time, density, effective atomic number (Z).
- Applications: Gamma camera (NaI(Tl)), PET (BGO, LSO, LYSO), well counters, liquid scintillation counters.
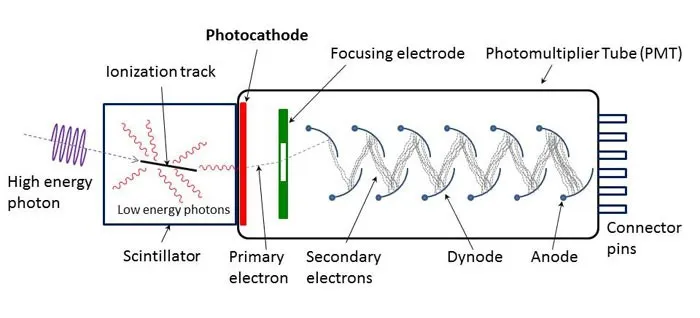
⭐ NaI(Tl) is the most common scintillator in gamma cameras due to its high light output and good efficiency for typical gamma ray energies.
Solid-State Detectors - Crystal Clear Counts
- Principle: Radiation creates electron-hole (e-h) pairs in semiconductor (Si, Ge). P-N junction's depletion region collects charge.
- Advantages: Superior energy resolution; low energy ($W$) needed per e-h pair.
- Types:
- Silicon (Si(Li)): For X-rays, charged particles.
- Germanium (HPGe): For gamma spectroscopy; requires cooling (e.g., liquid N₂).
- Disadvantages: High cost, radiation damage susceptibility, HPGe cooling needs.
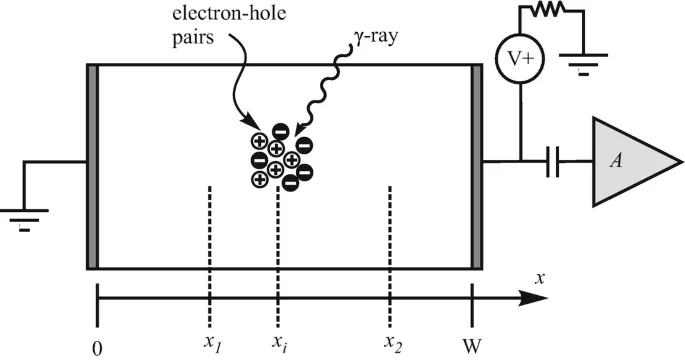
⭐ HPGe: Unmatched energy resolution for gamma spectroscopy, vital for radionuclide ID.
Dosimeters & Devices - Measuring the Dose
- Thermoluminescent Dosimeters (TLDs):
- Principle: Electrons trapped in material (e.g., LiF:Mg,Ti) emit light on heating (glow curve).
- Applications: Personnel & environmental monitoring.
- Optically Stimulated Luminescence Dosimeters (OSLDs):
- Principle: Light stimulation releases trapped charge, emitting light (e.g., Al₂O₃:C).
- Advantages: Re-readable, higher sensitivity.
- Film Badges:
- Principle: Ionizing radiation blackens silver halide emulsion.
- Disadvantages: Fading, sensitive to heat/humidity.
- Electronic Personal Dosimeters (EPDs):
- Semiconductor-based; provide real-time dose & dose rate readout, alarms.
⭐ TLDs (LiF) are nearly tissue-equivalent (effective Z similar to tissue), making them suitable for personnel dosimetry for whole-body dose.
High‑Yield Points - ⚡ Biggest Takeaways
- Gas-filled detectors (Ionization chamber, Proportional, GM counter) operate via gas ionization.
- Ionization chambers are used in dose calibrators and Automatic Exposure Control (AEC).
- Geiger-Muller (GM) counters: highly sensitive for contamination surveys, but offer no energy discrimination.
- Scintillation detectors (e.g., NaI(Tl)) convert radiation to light; core of gamma cameras.
- Thermoluminescent Dosimeters (TLDs) like LiF store energy, released as light on heating; for personnel dosimetry.
- Semiconductor detectors provide superior energy resolution for radionuclide identification.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

