Intro & Initial Response - Uh Oh, Glow!
Radiation Accident: Unplanned event; actual/potential radiation exposure or contamination. Goals: save lives, prevent harm escalation, mitigate consequences.
- Priorities:
- Treat life-threatening non-radiological injuries FIRST (ABCDE).
- Prevent further exposure & contamination spread.
- Rapidly assess radiological situation & hazards.
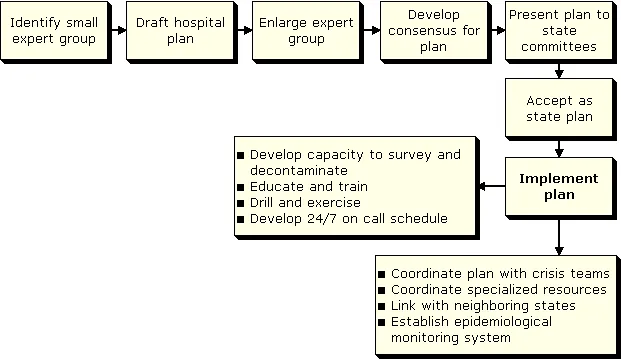
- Initial Actions (📌 SHINE):
- Secure area: Cordon off, control access.
- Help injured: Triage; trauma first. Stabilize.
- Identify contamination: Survey meters, define boundaries.
- Notify: RSO, local/national authorities (AERB/BARC).
- Evacuate: If needed, upwind from source. Shelter-in-place if appropriate.
⭐ Life-threatening non-radiological injuries (trauma, burns) ALWAYS take precedence over radiological concerns in initial management.
Victim Assessment & Triage - Zap Zone Checkup
- Initial "Zap Zone" Checkup:
- Rapid ABCDE survey for life threats.
- Identify highest risk: early severe symptoms (vomiting <1hr, CNS signs), known high exposure.
- Detect external contamination: Geiger-Müller counters.
- Triage Categories (Clinical & Dosimetric):
- Cat 1 (Expectant): Dose > 8-10 Gy. Severe early neurovascular symptoms. Palliative care.
- Cat 2 (Survival Probable): Dose 2-8 Gy. Prodromal (vomiting 1-2 hrs post-exposure). Hospitalize, supportive care, G-CSF.
- Cat 3 (Survival Likely): Dose < 2 Gy. Mild/delayed or no symptoms. Outpatient monitoring.
- Cat 4 (Minimal): No significant exposure/symptoms. Reassure.
- Biological Dosimetry:
- Blood: Lymphocyte count (kinetics), Dicentric Chromosome Assay (DCA).
- 📌 Nausea/vomiting onset time: rough dose estimate.
⭐ Lymphocyte count at 48 hours is key. Nadir < 0.5 x 10⁹/L (< 500/µL) suggests severe exposure (likely >4 Gy).

Decontamination & Decorporation - Scrubbing Rads Away
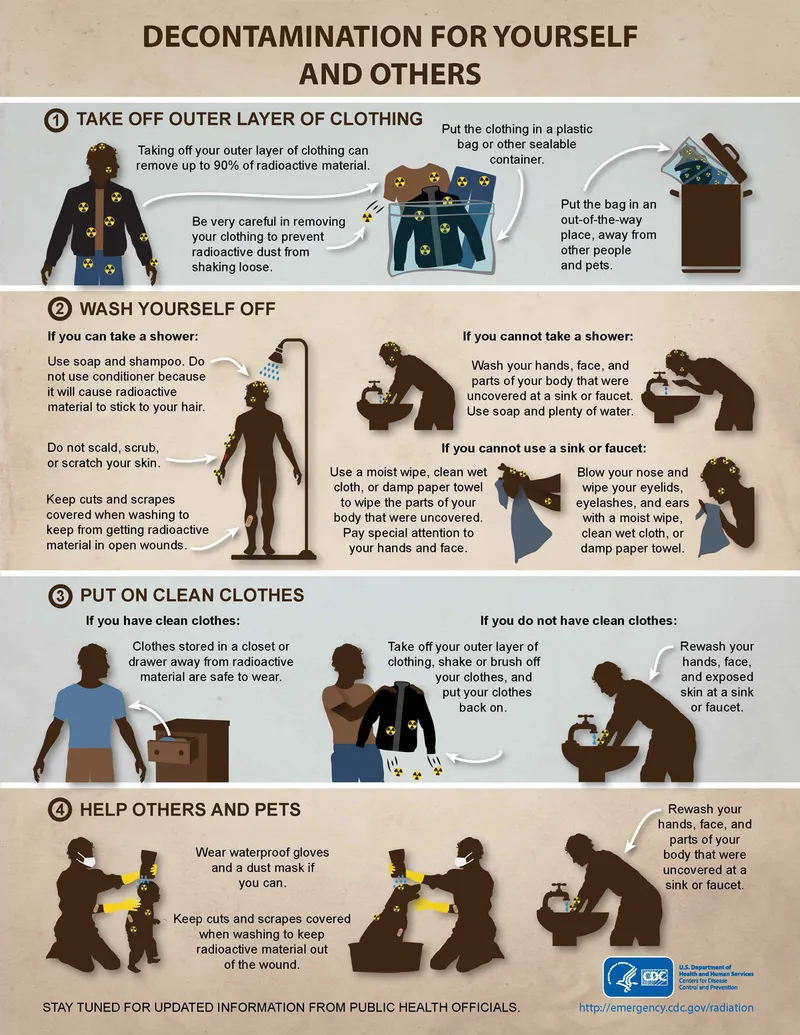
1. External Decontamination:
- Remove clothing (↓ ~90% contamination).
- Gentle wash: soap, lukewarm water. Avoid abrasion (↓ absorption).
- Clean cleaner to dirtier areas. Collect waste water.
- Care: hair, nails, folds.
2. Internal Decontamination (Decorporation):
- Goal: ↓ absorption, ↑ excretion.
- Agents:
- KI: For radioactive Iodine ($^{131}I$). Blocks thyroid.
- DTPA: For Plutonium ($Pu$), Americium ($Am$), Curium ($Cm$). Chelates.
- 📌 Prussian Blue: For Caesium ($^{137}Cs$), Thallium ($^{201}Tl$). Binds in gut.
- Water: For Tritium ($^3H$). Dilution.
- Diuretics/Laxatives: Enhance excretion.
⭐ Prussian Blue (Ferric Hexacyanoferrate) for Caesium-137 & Thallium-201 internal contamination significantly reduces biological half-life.
ARS & LRI Management - Healing Ray Harm
- Core Management:
- Aggressive supportive care: fluids, electrolytes, antiemetics, antibiotics, pain relief.
- Regular monitoring: CBC, electrolytes, organ function.
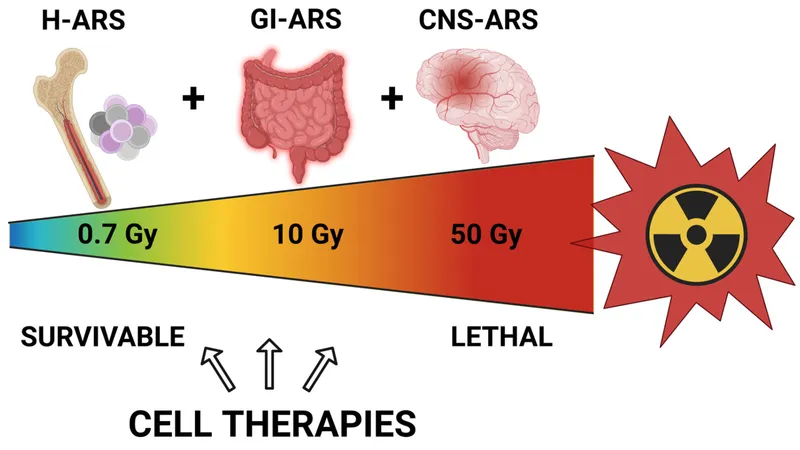
- Hematopoietic ARS (H-ARS):
- Cytokines (G-CSF/GM-CSF): If neutrophils < 0.5 x 10⁹/L or expected nadir < 0.5 x 10⁹/L.
- Transfusions: Platelets if < 10-20 x 10⁹/L; RBCs for anemia.
- Stem Cell Transplant (SCT): For whole-body dose > 7-10 Gy.
- Gastrointestinal ARS (GI-ARS):
- Aggressive fluid/electrolyte replacement.
- Parenteral nutrition.
- Local Radiation Injury (LRI):
- Pain management.
- Wound care: debridement, specialized dressings.
- Pentoxifylline & Tocopherol for fibrosis.
- Surgery for severe necrosis.
⭐ G-CSF (e.g., Filgrastim) is crucial for H-ARS if neutrophils fall below 0.5 x 10⁹/L, significantly improving survival.
High‑Yield Points - ⚡ Biggest Takeaways
- Prioritize external decontamination (remove clothes, wash) then internal decontamination (e.g., Prussian Blue for Cs-137, DTPA for transuranics).
- Triage victims based on clinical symptoms, exposure history, and lymphocyte depletion kinetics.
- Manage Acute Radiation Syndrome (ARS) syndromes: Hematopoietic (G-CSF, transfusions), Gastrointestinal (fluids, antiemetics), Neurovascular (supportive).
- Administer Potassium Iodide (KI) promptly to block thyroid uptake of radioactive iodine.
- Supportive care (fluids, infection control, pain management) is paramount for ARS victims anagement
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

