Introduction & Basics - Matter's Response
- Radiation: Energy transmitted as waves or particles.
- Matter: Anything with mass and volume, made of atoms.
- Types of Radiation:
- Electromagnetic (EM): X-rays, gamma rays (photons, no mass).
- Particulate: Electrons, protons, neutrons, alpha particles (have mass).
- Fundamental Processes:
- Excitation: Electron absorbs energy, moves to higher energy shell.
- Ionization: Radiation ejects electron from atom, creating an ion pair.
⭐ Differential attenuation of X-rays by various tissues is the fundamental principle behind radiographic image formation.
Low-Energy Photon Interactions - Photon Dance
Key low-energy X-ray interactions for imaging.
| Feature | Coherent (Rayleigh) Scattering | Photoelectric Effect (PE) |
|---|---|---|
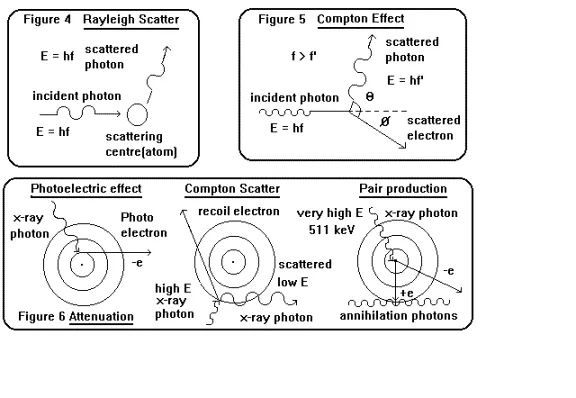
| Mechanism | Photon excites atom; re-emits same E photon, new direction. | Photon absorbed; ejects inner electron (photoelectron). Cascade emits characteristic X-ray/Auger e-. |
| Energy Range | <30 keV | 25-150 keV (diagnostic) |
| Z Dependence | $\propto Z^2$ | $\propto Z^3$ |
| E Dependence | $\propto 1/E^2$ | $\propto 1/E^3$ |
| Absorption | No (scattering) | Yes (absorption) |
| Products | Scattered photon (same E) | Photoelectron, Char. X-ray, Auger e- |
| Importance (Dx) | Minor; film fog (low kVp) | Primary for contrast |
- PE Formula: $PE \propto Z^3/E^3$

⭐ The Photoelectric Effect is the primary interaction responsible for subject contrast in diagnostic radiography, especially with contrast media and bone.
High-Energy Photon Interactions - Photon Clash
-
Compton Scattering: Photon interacts with an outer shell electron, ejecting a recoil electron and scattering the photon with reduced energy.
- 📌 "Compton Scatters, Independent of Zatter (matter's Z)" (largely independent of atomic number Z).
- Dominant in soft tissue at diagnostic energies (approx. 25 keV - 25 MeV).
- Products: Scattered photon, recoil electron.
-
Pair Production: High-energy photon (E > 1.022 MeV) interacts with the nucleus's field, converting into an electron-positron pair.
- Energy threshold: $E_{threshold} = 1.022 \text{ MeV}$.
- Positron annihilates with an electron, producing two $0.511 \text{ MeV}$ photons ($E_{annihilation} = 2 \times 0.511 \text{ MeV}$).
- Increases with photon energy and significantly with Z (approx. $Z^2$).
- Products: Electron-positron pair, then two annihilation photons.
-
Photodisintegration: Very high-energy photon (typically E > 7-10 MeV) is absorbed by the nucleus, ejecting a nuclear particle (e.g., neutron).
- Relevant at very high energies (radiotherapy).
Comparison: Compton vs. Pair Production
| Feature | Compton Scattering | Pair Production |
|---|---|---|
| Energy Threshold | Occurs at diagnostic energies | >1.022 MeV |
| Z Dependence | Largely Independent | Increases with $Z^2$ |
| Interaction | Scatter | Absorption (photon disappears) |
| Importance | Dominant in soft tissue (Dx imaging) | Important at therapeutic energies (Rx) |
Attenuation Principles - Beam Reduction
- Attenuation: ↓ radiation intensity in matter. $I = I_0 e^{-\mu x}$.
- Linear Att. Coeff. (µ): Intensity ↓ per unit thickness (cm⁻¹).
- Mass Att. Coeff. (µ/ρ): µ per density (cm²/g); density-independent.
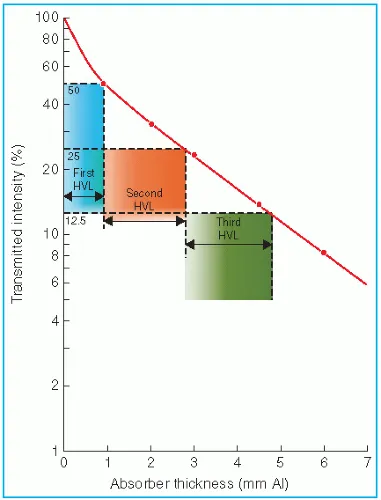
- Half Value Layer (HVL): Thickness for 50% intensity ↓. $HVL = \ln(2)/\mu \approx 0.693/\mu$.
⭐ The Half Value Layer (HVL) is a key indicator of X-ray beam quality or penetrability; a higher HVL means a more penetrating beam.
- Tenth Value Layer (TVL): Thickness for 90% intensity ↓. $TVL = \ln(10)/\mu \approx 2.303/\mu$.
- Factors for µ: ↑Energy → ↓µ (mostly); ↑Density (ρ) → ↑µ; ↑Atomic No. (Z) → ↑µ.
- Beam Hardening: Low-energy photon loss; ↑ avg. beam energy & penetrability.
 oka
oka
Particulate Interactions - Charged Paths
- Charged particles ($\alpha$, $\beta^-$, $\beta^+$) cause ionization & excitation.
- $\beta^-$ & $\beta^+$ also produce Bremsstrahlung (X-rays) in high-Z materials.
- Range: Particle's path length. LET: Energy deposited/unit distance.
- Alpha ($\alpha$): High mass, charge +2; Short range, $\uparrow$LET.
- Beta ($\beta^-$/$\beta^+$): Low mass, charge $\pm\mathbf{1}$; Longer range, $\downarrow$LET.
⭐ Bremsstrahlung production is significant for high-energy electrons interacting with high-Z materials, forming the basis of X-ray tube operation.
High-Yield Points - ⚡ Biggest Takeaways
- Photoelectric effect: Dominant at low energies & high-Z materials; key for image contrast.
- Compton scatter: Predominant at diagnostic energies in soft tissue; main source of scatter & staff dose.
- Pair production: Requires photon energy >1.02 MeV; basis for PET imaging.
- LET: High for alpha particles, low for X-rays/gamma rays; measures local energy deposition.
- Attenuation: Beam intensity reduction by absorption & scatter.
- HVL: Material thickness reducing intensity by 50%; measures beam penetrability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

