EM Spectrum - Wave Wonders
- EM radiation: Oscillating, perpendicular electric (E) & magnetic (B) fields. Travels at speed of light ($c$).
- $c \approx 3 \times 10^8 \text{ m/s}$ in vacuum.
- Wave-particle duality (photons).
- Energy: $E = h\nu = hc/\lambda$
- $h$: Planck's constant
- $\lambda$: Wavelength, $\nu$: Frequency
- Energy: $E = h\nu = hc/\lambda$
- Spectrum (↓$\lambda$, ↑E, ↑$\nu$):
📌 Roman Men Invented Very Unusual X-ray Guns
- Radio → Microwave → IR → Visible → UV → X-ray → Gamma ray
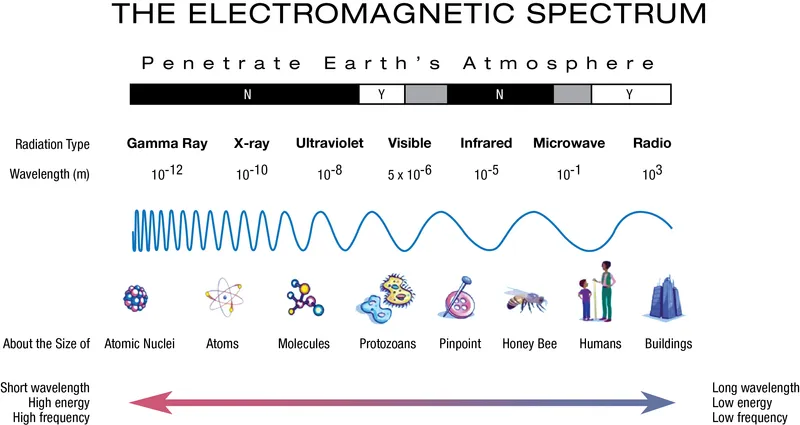
- Radio → Microwave → IR → Visible → UV → X-ray → Gamma ray
- Key Properties:
- Photons: no charge, no mass.
- Unaffected by E/B fields.
- Vary in $\lambda, \nu, E$.
⭐ X-rays originate from electron shell transitions, while Gamma rays originate from nuclear decay, regardless of their energy levels.
X-ray Production - Beam Basics
- Source: Thermionic emission from heated Tungsten filament (~2200°C) releases e⁻.
- Acceleration: High voltage (kVp) accelerates e⁻ to anode (Tungsten target).
- Tube Voltage (kVp): 25-150 kVp (diagnostic). Controls X-ray quality (penetrability) & max energy.
- Tube Current (mA): Controls X-ray quantity (photon number).
- Target Interactions:
- Bremsstrahlung: ~80-90%. e⁻ brakes near nucleus, emits X-ray. Continuous spectrum.
- Characteristic: Incident e⁻ ejects inner shell e⁻; outer e⁻ fills vacancy, emits specific energy X-ray. Discrete.
- Beam: Quantity (Intensity $I \propto mA \cdot (kVp)^2 / d^2$), Quality (↑kVp, ↑filtration).
⭐ High-Yield Fact: ~99% of incident electron kinetic energy converts to heat at the anode; only ~1% becomes X-rays.
EM Interactions - Photon Phate
| Interaction | Energy (Dominance) | Z Dependence | Key Outcome(s) | Relevance |
|---|---|---|---|---|
| Coherent (Rayleigh) | < 10 keV | $\propto Z^2$ | Photon scatter, no E loss | Minor haze, negligible dose |
| Photoelectric (PEA) | Low E (20-100 keV) | $\propto Z^3/E^3$ | Photon absorbed, e⁻ out, char. X-ray | High contrast (bone), ↑dose |
| Compton (CS) | Mid E (0.1-10 MeV) | $\propto \rho_e$, Z-indep. | Photon scatter (↓E), e⁻ out | Soft tissue contrast, scatter, staff hazard |
| Pair Production (PP) | > 1.022 MeV (Threshold) | $\propto Z^2$ | e⁻/e⁺ pair; Annihilation (2x 0.511 MeV) | PET, high-E RT |
⭐ Compton scattering is the most probable interaction between x-rays and soft tissue over a significant portion of the diagnostic energy range.
Radiation Quantities - Unit Roundup
| Quantity | Definition | SI Unit (Symbol) | Trad. Unit (Symbol) | Conversion |
|---|---|---|---|---|
| Exposure (X) | Ionization in air (X/γ rays) | C/kg | Roentgen (R) | 1 R = $2.58 \times 10^{-4}$ C/kg |
| Absorbed Dose (D) | Energy absorbed/mass | Gray (Gy) | rad | 1 Gy = 100 rad |
| Equivalent Dose (H) | Absorbed dose $\times$ radiation type ($w_R$) | Sievert (Sv) | rem | 1 Sv = 100 rem |
| Effective Dose (E) | Equivalent dose $\times$ tissue sens. ($w_T$) | Sievert (Sv) | rem | 1 Sv = 100 rem |
⭐ For X-rays, γ-rays, and beta particles, the radiation weighting factor is 1. Thus, for these radiations, Absorbed Dose in Gray is numerically equal to Equivalent Dose in Sievert.
High‑Yield Points - ⚡ Biggest Takeaways
- Electromagnetic radiation (EMR) travels at the speed of light (approx. 300 million m/s in vacuum).
- Photon energy is directly proportional to frequency, and inversely proportional to wavelength.
- X-rays (from electron shells) and gamma rays (from nucleus) are key ionizing EMRs in medicine.
- Inverse Square Law: EMR intensity decreases rapidly with increasing distance from the source.
- Shorter wavelength EMR possesses higher energy and greater penetration capabilities.
- EMR exhibits wave-particle duality, behaving as both waves and discrete particles (photons).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

