Initial Steps - Patient Prep & Imaging Powwow
- Patient Assessment & Consent:
- Comprehensive clinical evaluation: history, physical exam, performance status (e.g., ECOG, Karnofsky).
- Informed consent obtained: discussion of procedure, benefits, risks, alternatives.
- Immobilization & Positioning:
- Goal: Ensure reproducible patient setup for daily treatment accuracy.
- Devices: Thermoplastic masks, vacuum cushions (Vac-Lok™), alpha cradles, bite blocks.
- Fiducial markers or tattoos may be used for alignment.
- Simulation (Sim) Imaging:
- CT simulation is the primary imaging modality.
- Provides electron density data for dose calculation.
- Scan parameters: appropriate slice thickness (e.g., 2-3 mm), scan range covers target volume + margins.
- IV contrast may be used to delineate structures.
- 4DCT for targets with respiratory motion (e.g., lung, liver).
- Other imaging: MRI (superior soft tissue contrast), PET-CT (metabolic activity) often fused with CT sim data.
- CT simulation is the primary imaging modality.

⭐ CT simulation is the gold standard for initial treatment planning as it provides crucial electron density information required for accurate dose calculation by the treatment planning system (TPS).
Volume Delineation - Target Lock & Organ Guard
- GTV (Gross Tumor Volume): Macroscopic tumor; visible, palpable, or imageable.
- CTV (Clinical Target Volume): GTV + margin for subclinical microscopic disease.
- Anatomical-clinical concept.
- ITV (Internal Target Volume): CTV + internal margin (IM) for internal geometric variations (e.g., respiration).
- PTV (Planning Target Volume): CTV or ITV + setup margin (SM).
- Accounts for patient positioning/alignment uncertainties.
- Used for plan optimization & dose prescription.
- OAR (Organs at Risk): Normal tissues whose radiation sensitivity limits prescribed dose.
- PRV (Planning OAR Volume): OAR + margin for OAR position/delineation uncertainties.
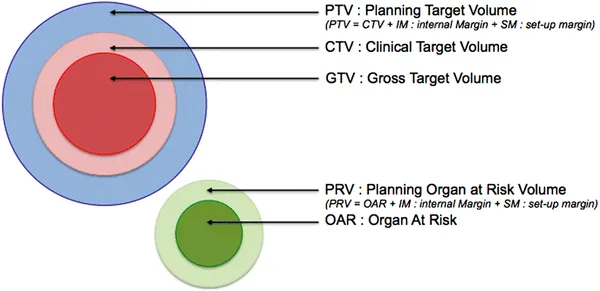
⭐ The PTV is the volume for which the radiation plan is designed to deliver the prescribed dose, encompassing all uncertainties.
Plan Design - Beam Tactics & Dose Artistry
- Beams & Modifiers:
- Energy/Type: kV (superficial), MV (deep photons), MeV (electrons, superficial), Protons (Bragg peak, distal spare).
- Modifiers: Wedges (tilt isodose), Bolus (↑surface dose, e.g., chest wall), Compensators (custom).
- Techniques & Arrangement:
- 3D-CRT: Conformal shaping.
- IMRT: Inverse planning, ↑conformity, OAR sparing.
- VMAT: Rotational IMRT.
- SBRT/SRS: Hypofractionated (e.g., 1-5 fx), ablative doses.
- Angles: Coplanar/Non-coplanar.
- Dose Calculation:
- Algorithms: Pencil Beam (fast, less accurate), Convolution/Superposition (balanced), Monte Carlo (gold standard).
- Plan Evaluation:
- DVH: PTV/OAR dose-volume.
- Indices: CI (Conformity Index), HI (Homogeneity Index; $HI = (D_{2%} - D_{98%}) / D_p$).
- OAR tolerance (QUANTEC).

⭐ IMRT enables "dose painting": delivering varying doses to different target subvolumes simultaneously.
Final Checks & Go-Live - QA & Treatment Launch
- Pre-Treatment Quality Assurance (QA): Critical for safety and accuracy.
- Independent Calculation/Plan Check: By a second qualified physicist. Verifies MUs, dose, constraints.
- Patient-Specific QA (PSQA): For complex plans (IMRT, VMAT, SRS/SBRT).
- Phantom measurements validate dose distribution.
- Common tolerance: ±3% dose difference, 3 mm Distance-to-Agreement (DTA).
- Machine QA: Ensures linac performance. Includes daily (output, lasers, door interlock, ODI), monthly, and annual checks.
- Treatment Launch (First Fraction):
- Dry Run: Optional; simulates setup and delivery without beam.
- Patient Identification & Setup: Verify patient ID, site, immobilization, alignment to lasers/tattoos.
- "Time Out": Final verification by entire treatment team before beam-on (Correct Patient, Site, Plan, Dose).
- Image-Guided Radiotherapy (IGRT): Pre-treatment imaging (e.g., CBCT, kV/MV EPID) for position verification and correction.
- Record & Verify (R&V) system confirmation.
⭐ For IMRT/VMAT, patient-specific QA passing criteria are often 95% of measured points within 3% dose difference and 3mm distance-to-agreement (gamma index).
High‑Yield Points - ⚡ Biggest Takeaways
- Immobilization is paramount for treatment reproducibility and setup accuracy.
- CT simulation defines target volumes (GTV, CTV, PTV) and Organs at Risk (OARs).
- Image registration/fusion (CT, MRI, PET) enhances precise target delineation.
- Beam arrangement, energy selection, and modifiers optimize dose distribution.
- Dose calculation algorithms (e.g., Pencil Beam, Monte Carlo) determine dose delivery.
- Plan evaluation via Dose Volume Histograms (DVHs) assesses target coverage and OAR sparing.
- Pre-treatment QA and IGRT (Image-Guided Radiotherapy) ensure accurate treatment delivery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

