Total Body Irradiation - Body Under Siege
- Definition: Radiation therapy delivered uniformly to the entire body.
- Primary Goals:
- Eradicate malignant cells (leukemia, lymphoma).
- Immunosuppression for HSCT (prevent graft rejection).
- Bone marrow ablation.
- Key Indications:
- HSCT conditioning (most common).
- Palliation (widespread low-grade lymphoma, rare).
- Dose: Typically 10-15 Gy fractionated (e.g., 1.5-2 Gy/fraction). Single dose ~7.5 Gy (higher toxicity).
- Lung shielding vital; mean lung dose often <8-10 Gy.
⭐ TBI is a cornerstone of myeloablative conditioning for allogeneic HSCT, especially in acute leukemias.
Total Body Irradiation - Zap Strategy
- Goal: Eradicate malignant cells (leukemia, lymphoma), immunosuppression for BMT/SCT.
- Techniques:
- AP/PA (Anterior-Posterior/Posterior-Anterior): Patient standing or lying, large SSD.
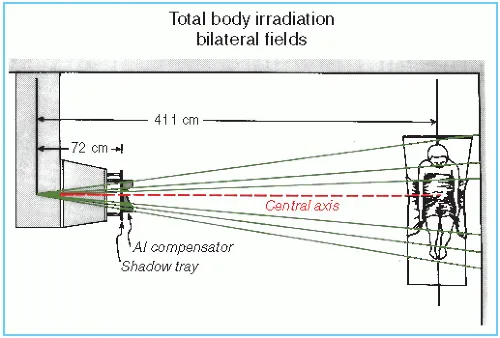
- Bilateral: Two opposing large fields, patient lying on side.
- Rotational or translational methods for dose uniformity.
- Beam: High energy photons (e.g., 6-10 MV LINACs) to ensure penetration.
- Dose Rate:
- Low Dose Rate (LDR): 5-15 cGy/min (classic).
- High Dose Rate (HDR): >15-20 cGy/min (more common now with fractionation).
- Fractionation:
- Single dose: e.g., 10 Gy (historically, higher toxicity).
- Fractionated: e.g., 12-15 Gy in 6-8 fractions over 3-4 days (improves tolerance, reduces late effects).
- Organ Shielding: Lungs (critical), kidneys, lenses (sometimes).
⭐ Lung dose is a major limiting factor; typically kept < 8-10 Gy with shielding to reduce risk of pneumonitis.
- Immobilization: Essential for reproducibility.
- In vivo dosimetry: TLDs or diodes on skin to verify dose delivery. 📌 Total Body Irradiation = Treat Big Intervals (fractionation).
Total Body Irradiation - Target Lock
- Aim: Uniform dose (typically ±5% to ±10%) across entire body for marrow ablation/immunosuppression pre-HSCT.
- Techniques: AP/PA or bilateral fields, extended SSD; compensators/bolus for homogeneity.
- Dose: 10-14 Gy total; single or fractionated (e.g., 1.5-2 Gy/fx, BID).
- Lung Shielding: Critical to prevent pneumonitis.
- Custom blocks (Cerrobend) or MLCs.
- Mean Lung Dose (MLD) target: < 8-10 Gy.
- Other OARs: Kidneys (limit < 12-14 Gy), Lens (limit < 5 Gy if possible).
- Verification: In vivo dosimetry (TLDs/diodes) at key anatomical points.

⭐ Lungs are the primary dose-limiting organs in TBI; mean lung dose is crucial, often kept < 8 Gy to minimize radiation pneumonitis risk.
Total Body Irradiation - Radiation's Toll
- Acute Toxicities (Days to Weeks):
- Gastrointestinal Syndrome: Nausea, vomiting, diarrhea, mucositis, parotitis.
- Hematopoietic Syndrome: Myelosuppression leading to pancytopenia; nadir at ~2-3 weeks. Risk of infection, bleeding.
- Pulmonary: Acute radiation pneumonitis (RP); typically 1-3 months post-TBI. Can be dose-limiting.
- Skin: Erythema, desquamation.
- Constitutional: Fever, fatigue.
- Late Toxicities (Months to Years):
- Ocular: Cataracts (most common non-fatal late effect, dose-dependent).
- Endocrine: Hypothyroidism, hypogonadism (infertility).
- Pulmonary: Chronic fibrosis, restrictive disease.
- Renal: Radiation nephropathy (proteinuria, hypertension, renal failure).
- Skeletal: Growth retardation (children), osteonecrosis.
- Carcinogenesis: Increased risk of secondary malignancies (e.g., AML, MDS, solid tumors).
- Hepatic: Veno-occlusive disease (VOD), especially with prior chemotherapy.
- Neurologic: Cognitive dysfunction (rare).
⭐ Interstitial pneumonitis is a major dose-limiting acute toxicity, often occurring 1-3 months post-TBI, and can be fatal if severe.
High‑Yield Points - ⚡ Biggest Takeaways
- TBI is crucial for pre-HSCT conditioning, mainly in leukemias and lymphomas.
- Aims: Malignant cell kill, immunosuppression for graft acceptance, and marrow space creation.
- Dose: 10-15 Gy in fractions; low dose rate (e.g., 5-15 cGy/min) is vital to reduce toxicity.
- Interstitial pneumonitis is the primary dose-limiting toxicity; lung shielding is often employed.
- Other major risks: Veno-occlusive disease (VOD), cataracts, endocrine dysfunction, and secondary malignancies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

