Stereotactic Radiosurgery - Precision Zap Basics
- Definition: Non-invasive radiation therapy delivering a single high dose (or 2-5 high-dose fractions) of precisely targeted ionizing radiation to well-defined intracranial or extracranial lesions.
- Core Principles:
- Stereotaxy: Sub-millimeter accurate lesion localization using 3D coordinate systems (frame-based or frameless image guidance).
- Conformality: Radiation dose is meticulously shaped to closely match the 3D contour of the target volume.
- Steep Dose Gradient: Achieves a rapid decrease in radiation dose at the periphery of the target, minimizing exposure to adjacent healthy tissue.
- Goal: Achieve complete biological ablation of the target tissue while preserving the integrity and function of surrounding normal structures.
- Key Feature: Delivers a high Biological Effective Dose (BED) due to the large dose per fraction.
⭐ SRS is characterized by its extreme precision, allowing for the treatment of lesions, especially those that are small and well-circumscribed, even when located near critical or eloquent structures where surgery might be high risk.
Stereotactic Radiosurgery - Zap Tech Parade
- Definition: High-dose, precisely focused radiation (1-5 fractions). Ablative doses, steep dose fall-off.
- Key Technologies:
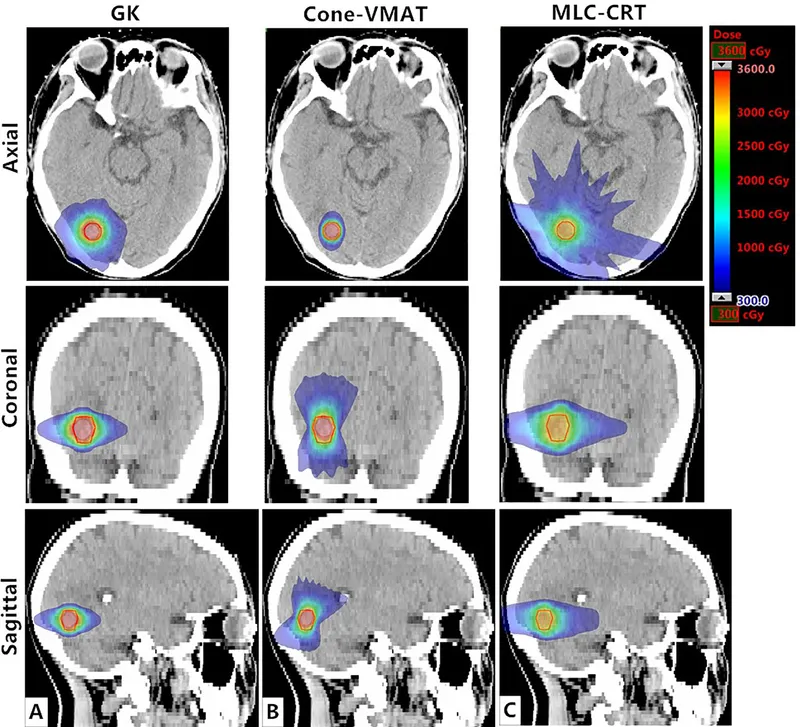
- Gamma Knife (GK): Multiple Cobalt-60 sources (e.g., 192, 201). Intracranial. Highly conformal.
⭐ Gamma Knife typically uses 192 or 201 Cobalt-60 sources, converging on the target to deliver a high dose with rapid fall-off.
- LINAC-based SRS: Linear accelerators.
- Techniques: Conformal arcs, Dynamic Conformal Arcs (DCA), IMRS.
- Versatile: Intracranial & extracranial (SBRT).
- CyberKnife: Robotic arm-mounted LINAC.
- Real-time image guidance (X-ray/fiducials). Tracks tumor motion.
- Gamma Knife (GK): Multiple Cobalt-60 sources (e.g., 192, 201). Intracranial. Highly conformal.
- Immobilization: Critical for sub-mm accuracy.
- Invasive: Stereotactic frames.
- Non-invasive: Masks, vacuum bags.
- Targeting: CT/MRI/PET fusion for delineation.
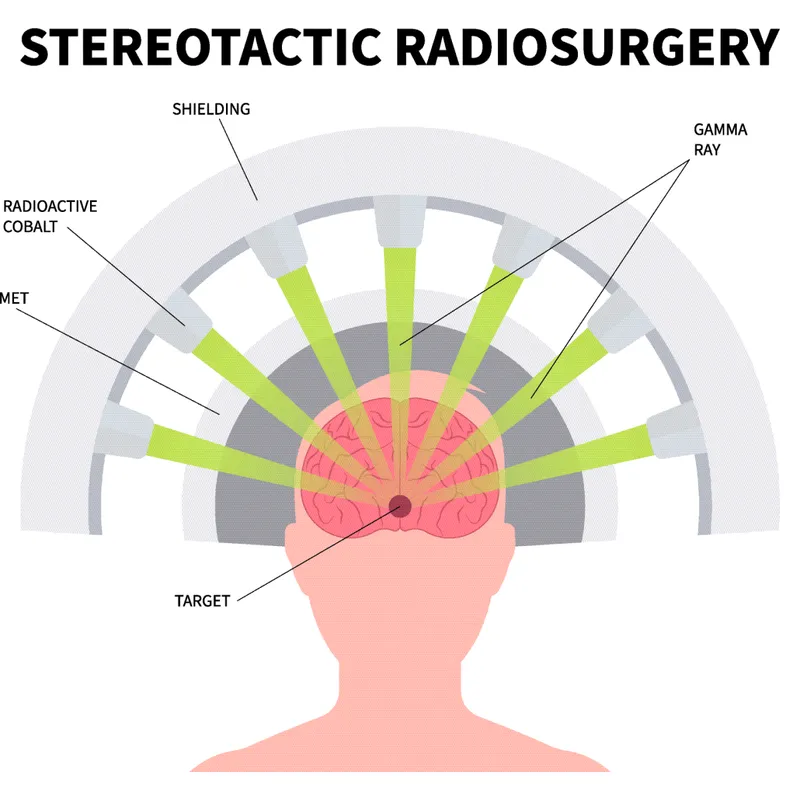
Stereotactic Radiosurgery - Target Practice Time
- Key Targets & Doses (Single Fraction):
- Brain Metastases: Most common (≤ 4-5 lesions).
- Dose: 15-24 Gy (size-dependent: <2cm: 20-24 Gy; 2-3cm: 18 Gy; >3cm: 15-16 Gy).
- Arteriovenous Malformations (AVMs):
- Goal: Obliteration. Dose: 16-25 Gy to nidus.
- 📌 AVM: "Rule of 2s" - 2 yrs, ~80% obliteration, ~20 Gy.
- Benign Tumors:
- Acoustic Neuroma: 12-13 Gy (hearing preservation).
- Meningioma: 12-16 Gy. Pituitary Adenoma: 12-25 Gy.
- Functional Disorders:
- Trigeminal Neuralgia: 70-90 Gy to nerve root.
- Movement disorders (e.g., Essential Tremor).
- Brain Metastases: Most common (≤ 4-5 lesions).
⭐ SRS is typically for lesions < 3-4 cm; larger lesions may require fractionated SRT or surgery due to normal tissue toxicity risk.
Stereotactic Radiosurgery - Zap Zone Dangers
- Contraindications:
- Large tumors (> 3-4 cm / > 20-30 cc)
- Multiple lesions (> 5-10)
- Poorly defined targets on imaging
- Prior overlapping high-dose RT
- Complications:
- Acute: Edema (common; steroids), headache, nausea.
- Late: Radiation Necrosis (RN) (months-years, mimics recurrence), cranial neuropathies.
- RN risk ↑ with dose & volume.
- SRS vs. Alternatives:
- SRT: 2-5 fractions; for larger/eloquent area tumors, ↓ toxicity.
- Conventional RT: Lower dose/fraction, longer course, less precise.
- Surgery: Invasive, immediate debulking, histology; SRS for inaccessible/high-risk cases.
⭐ Radiation necrosis is a key delayed complication of SRS, often presenting months to years post-treatment and can be challenging to differentiate from tumor recurrence.
High‑Yield Points - ⚡ Biggest Takeaways
- SRS delivers a single, high ablative dose of radiation with sub-millimeter accuracy.
- Employs rigid immobilization (frame-based/frameless) for precise targeting of intracranial lesions.
- Key indications: small brain metastases, acoustic neuromas, arteriovenous malformations (AVMs), and trigeminal neuralgia.
- Technologies include Gamma Knife (cobalt-60), CyberKnife (robotic LINAC), and specialized LINACs.
- Characterized by a sharp dose gradient, maximally sparing adjacent normal tissues.
- Distinguished from SRT (Stereotactic Radiotherapy) which uses 2-5 fractions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

