Intensity-Modulated Radiation Therapy - Beam Sculpting 101
- Advanced high-precision radiotherapy technique.
- Delivers radiation by modulating (varying) intensity of multiple small radiation beams.
- Each beam is divided into many "beamlets".
- Intensity of individual beamlets is independently controlled.
- Key Technology:
- Dynamic Multi-Leaf Collimators (dMLCs) or segmental MLCs (sMLCs).
- "Inverse planning": Desired dose distribution is specified first, then computer calculates beam parameters.
- Primary Aim: Achieve highly conformal dose distributions to target volumes while sparing surrounding healthy tissues.
⭐ IMRT enables creation of concave dose distributions, crucial for complex tumor shapes near critical organs, unlike conventional 3D-CRT (3D Conformal Radiation Therapy).
Intensity-Modulated Radiation Therapy - The Good & The Gotchas
The Good (Advantages):
- Superior conformality: Dose precisely "paints" complex target volumes.
- Steep dose fall-off: Minimizes dose to adjacent Organs at Risk (OARs).
- Enables dose escalation: Higher tumor dose, potentially ↑ local control.
- Reduced toxicity: E.g., parotid sparing in Head & Neck cancers, reducing xerostomia.
- Creates concave dose shapes: Unachievable with 3D-CRT.
The Gotchas (Disadvantages/Challenges):
- Complexity: ↑ planning time, stringent Quality Assurance (QA) essential.
- Integral Dose: Larger volume of normal tissue receives low radiation dose ("low-dose bath").
⭐ Despite superior OAR sparing, IMRT results in a larger low-dose bath to normal tissues, posing a theoretical ↑ risk of secondary cancers in long-term survivors.
- Motion Sensitivity: Highly sensitive to target/organ motion & setup inaccuracies.
- Monitor Units (MUs): ↑ MUs, potentially longer treatment delivery times.
- Cost: More expensive than 3D-CRT.
Intensity-Modulated Radiation Therapy - From Plan to Patient
- Immobilization: Crucial for reproducibility (e.g., masks, vac-bags).
- Target Delineation:
- GTV (Gross Tumor Volume): Visible tumor.
- CTV (Clinical Target Volume): GTV + microscopic spread.
- PTV (Planning Target Volume): CTV + setup margins.
- Inverse Planning: Computer optimizes beamlet intensities to achieve desired dose distribution.
- Quality Assurance (QA): Essential before treatment; verifies planned vs. delivered dose.
⭐ IMRT uses Multi-Leaf Collimators (MLCs) that move dynamically during treatment to shape the radiation beam and modulate its intensity, allowing for highly conformal dose distributions to complex tumor shapes while sparing surrounding normal tissues. This process is often referred to as "painting" the dose onto the tumor volume slice by slice or arc by arc (for VMAT).
Intensity-Modulated Radiation Therapy - Prime Clinical Uses
- Head & Neck Cancers:
- Nasopharynx, oropharynx, larynx, hypopharynx.
- Spares salivary glands (↓xerostomia), spinal cord, optic structures.
- Prostate Cancer:
- Allows dose escalation to prostate.
- Spares rectum, bladder.
- Brain Tumors:
- Complex-shaped tumors near critical structures (e.g., brainstem, optic chiasm).
- Gynecological Cancers:
- Cervix, endometrium.
- Spares bladder, rectum, small bowel.
- Lung Cancer (NSCLC):
- For tumors near critical mediastinal structures.
- Pediatric Tumors:
- Reduces integral dose, potentially ↓late toxicities & ↓risk of secondary malignancies.
- Re-irradiation:
- For cases where normal tissue tolerance is limited by prior radiotherapy.
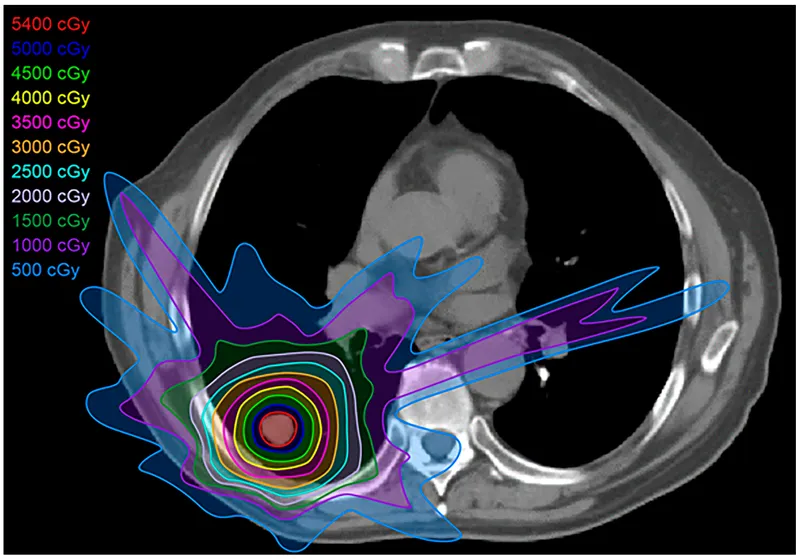
⭐ IMRT facilitates "dose painting": delivering heterogeneous doses within the target volume, escalating dose to high-risk subvolumes while concurrently sparing adjacent critical structures more effectively than 3D-CRT. This is particularly useful for boosting resistant tumor areas.
High‑Yield Points - ⚡ Biggest Takeaways
- IMRT uses multiple small beams with varying intensities for precise tumor targeting.
- Creates highly conformal dose distributions, closely matching complex tumor shapes.
- Maximizes tumor dose while significantly sparing surrounding normal tissues and critical organs.
- Relies on dynamic Multileaf Collimators (MLCs) and inverse planning software.
- Key advantage: Reduced toxicity to organs at risk (OARs).
- Common indications: Head & Neck cancers, prostate cancer, CNS tumors.
- Concern: Increased integral dose and potential for secondary malignancy due to larger low-dose volume.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

