IGRT: Core Concepts - Pinpoint Precision
- Definition: Imaging before (offline) or during (online) radiotherapy (RT) to improve precision & accuracy of dose delivery.
- Primary Goal: Minimize geometric uncertainties; accurate dose to target (PTV/CTV), spare Organs at Risk (OARs).
- Addresses:
- Inter-fraction motion (e.g., bladder filling, rectal gas).
- Intra-fraction motion (e.g., breathing, peristalsis).
- Patient setup variations.
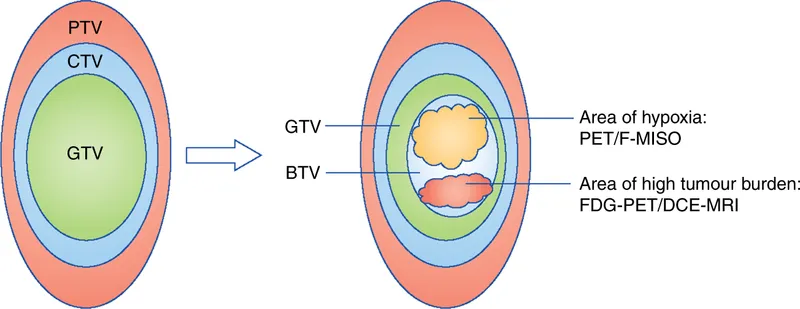
- Impact:
- Enables target dose escalation.
- Allows tighter PTV margins (e.g., from 10-15 mm to 3-5 mm).
- ↓ Radiation toxicity.
- Facilitates Adaptive Radiotherapy (ART).
⭐ Cone Beam CT (CBCT) is the most widely used IGRT technique for volumetric verification before daily treatment delivery to correct setup errors and monitor anatomical changes during the course of radiotherapy treatment for various cancer sites such as prostate, lung, and head and neck cancers, allowing for precise targeting and sparing of normal tissues, which is crucial for improving treatment outcomes and reducing side effects in patients undergoing radiation therapy for cancer management and cure.
IGRT: Imaging Modalities - The Tech Arsenal
Image-Guided Radiation Therapy (IGRT) utilizes various imaging techniques to enhance treatment accuracy. Key modalities offer distinct advantages and limitations for daily patient setup verification and target tracking:
| Modality | Image Quality (IQ) | Soft Tissue Contrast (STC) | Imaging Dose | Acquisition Speed | Key Advantages | Key Disadvantages |
|---|---|---|---|---|---|---|
| kV CBCT | Good | Moderate | Low-Mod | Fast (seconds) | Volumetric 3D, good bony detail, widely used | Scatter/artifacts, cumulative daily dose |
| MVCT | Fair | Poor | High | Moderate (mins) | Co-axial with Tx beam, ↓metal artifacts | Poor STC, higher imaging dose |
| MRI-Linac | Excellent | Excellent | Zero (MR) | Slower (mins) | Superior STC, no ionizing dose (MR), adaptive RT | High cost, B-field effects, geometric issues |
| Ultrasound | Fair-Good | Good (e.g., prostate) | Zero | Real-time | Non-ionizing, real-time (prostate, breast), portable | Operator-dependent, limited penetration |
⭐ MRI-Linac provides unparalleled soft tissue delineation without extra ionizing radiation, pivotal for precise targeting near organs at risk.
IGRT: Workflow & Process - Lights, Camera, Action!
IGRT verifies and corrects patient/tumor position immediately before or during radiation delivery, minimizing geometric uncertainties, enhancing precision.
- Core Workflow:
- IGRT Strategies & Purpose:
- Offline (e.g., EPID): Post-imaging review over fractions. Corrects systematic setup errors. Protocol-based.
- Online (e.g., CBCT, kV planar): Pre-treatment imaging; immediate couch shifts. Corrects random & systematic errors daily.
- Intrafraction (e.g., Calypso, AlignRT): Real-time tumor/surrogate monitoring & adjustment during beam delivery (gating, tracking). Manages motion.
- Key Decision Factors: Tumor site & mobility (lung, prostate), PTV margins, available imaging tech, workflow.
⭐ CBCT is the most widely used online IGRT, offering volumetric soft-tissue/bony anatomy verification at treatment time.
IGRT: Clinical Significance - Gains & Pains
Gains (Benefits):
- 🎯 Enhanced Precision: Improved target localization, reduced geometric uncertainties.
- 🛡️ Normal Tissue Sparing:
- Smaller Planning Target Volume (PTV) margins.
- Reduced dose to surrounding Organs at Risk (OARs), ↓ toxicity.
- 🔥 Dose Escalation: Allows higher, more effective doses to the tumor, potentially ↑ Tumor Control Probability (TCP).
- 🔄 Adaptive Radiotherapy (ART): Facilitates plan adjustments during treatment course based on anatomical/physiological changes.
- 💨 Hypofractionation Feasibility: Supports Stereotactic Body Radiation Therapy (SBRT)/Stereotactic Radiosurgery (SRS) by ensuring accurate high-dose delivery.
Pains (Limitations/Challenges):
- ☢️ Additional Imaging Dose: Cumulative radiation exposure from repeated imaging procedures.
- ⏰ Increased Treatment Time: Longer per-fraction duration due to on-couch imaging and verification.
- 💰 Resource Intensive: Requires expensive technology, specialized personnel, and robust Quality Assurance (QA).
- ⚙️ Workflow Complexity: Adds steps to treatment delivery, potential for errors if not managed.
- ⚠️ Image Artifacts/Interpretation: Challenges with image quality (e.g., metal artifacts) and accurate interpretation.
⭐ IGRT is crucial for highly conformal treatments like IMRT and VMAT, enabling tighter margins (e.g., 2-5 mm for prostate instead of 7-10 mm without IGRT), significantly reducing OAR toxicity.
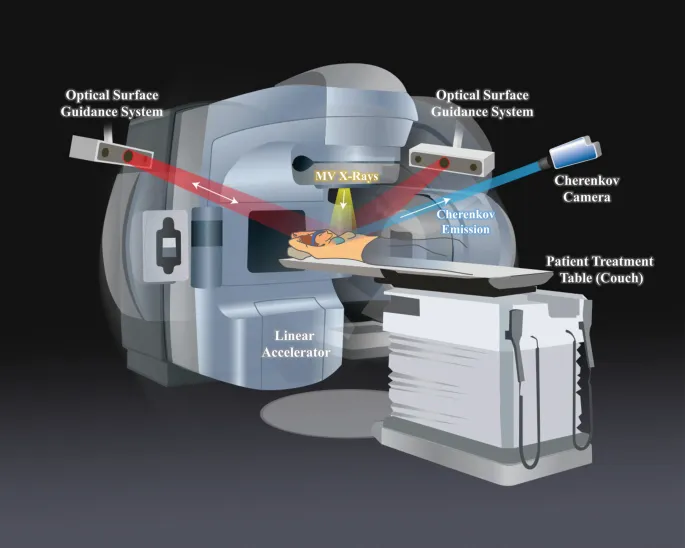
High‑Yield Points - ⚡ Biggest Takeaways
- IGRT uses imaging during radiotherapy to enhance precision and accuracy.
- Visualizes tumor and normal tissues immediately before or during radiation.
- Common modalities: kV Cone Beam CT (CBCT), MVCT, ultrasound, fiducial markers.
- Reduces treatment margins, spares healthy tissue, allows potential dose escalation.
- Corrects for inter-fractional (day-to-day) and intra-fractional motion.
- Essential for advanced techniques like SBRT/SRS and IMRT/VMAT.
- Improves tumor control and significantly reduces treatment-related toxicity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

