EBRT Intro - Healing Rays
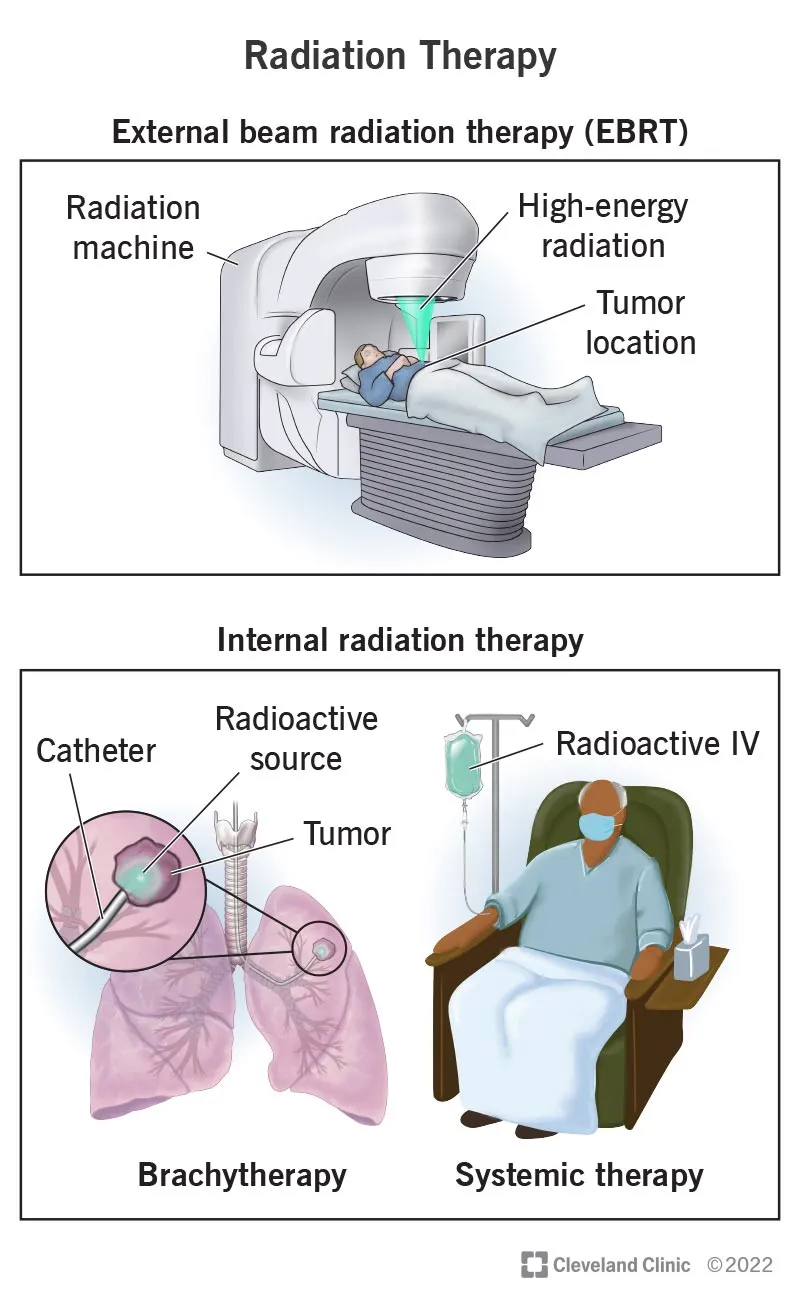
- EBRT: Uses external radiation (X-rays, gamma rays, electrons) from machines like Linacs or Cobalt-60 units to treat tumors.
- Mechanism: Delivers precise radiation doses to the tumor while sparing surrounding healthy tissues.
- Fractionation: Total radiation dose is divided into multiple smaller daily treatments (fractions).
- Allows normal cells to repair.
- Exploits differences in radiobiology between tumor and normal cells.
- Therapeutic Ratio (TR): $TR = \frac{TCP}{NTCP}$ (Tumor Control Probability / Normal Tissue Complication Probability).
⭐ Higher Therapeutic Ratio (TR) = better treatment outcome.
Linac & Co. - The Beam Machines
- Linear Accelerator (Linac): Most common EBRT machine.
- Produces X-rays (photons) for deep tumors & electrons for superficial targets (e.g., skin, nodes <5 cm).
- Key parts: Electron gun, waveguide, bending magnet, target, filter, collimators (MLCs).
- Cobalt-60 Units:
- Radioactive $^{60}Co$ source emitting gamma rays (avg. 1.25 MeV).
- Simpler design, larger penumbra due to source size. Source needs periodic replacement.
⭐ Modern Linacs can deliver highly conformal treatments like IMRT and VMAT due to precise Multi-Leaf Collimators (MLCs).
Plan & Target - Precision Plotting
- Simulation (Sim): Patient positioning, immobilization.
- CT sim: Standard; electron density for dose calc.
- Optional: MRI (soft tissue), PET-CT (metabolic).
- Target Volume Definition (ICRU 50, 62): 📌 Go Catch The Internal Plan (GTV→CTV→ITV→PTV)
- GTV (Gross Tumor Volume): Macroscopic disease.
- CTV (Clinical Target Volume): GTV + microscopic spread.
- ITV (Internal Target Volume): CTV + internal margin (IM) for motion.
- PTV (Planning Target Volume): CTV/ITV + setup margin (SM).
- $PTV = ITV + SM$; $ITV = CTV + IM$.
- OAR (Organs at Risk): Normal tissues. PRV.
- Treatment Planning:
- Dose, energy, angles, modifiers (MLCs, wedges).
- Dose calc: Algorithms (Pencil Beam, Monte Carlo).
- Plan Eval: Dose Volume Histograms (DVH).
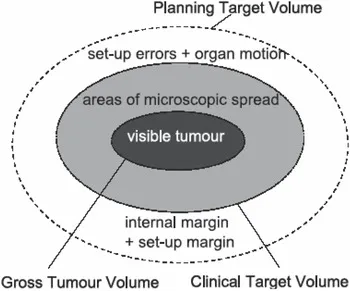
⭐ PTV accounts for organ motion (IM) & setup variations (SM), ensuring CTV dose coverage despite uncertainties.
Delivery Tech - Smart Strikes
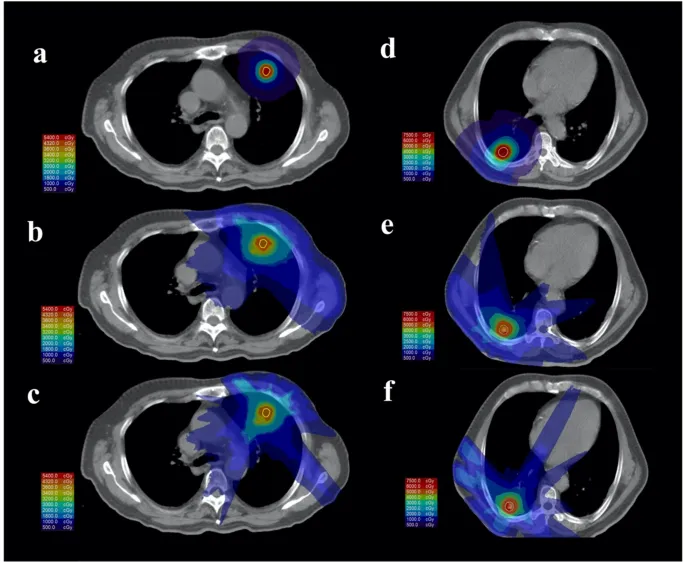
- 3D-CRT: Beams match tumor shape via Multi-Leaf Collimators (MLCs).
- IMRT: Modulates beam intensity; ↑ conformity, ↓ Organ at Risk (OAR) dose. Uses inverse planning.
- VMAT/RapidArc: Arc-based IMRT; faster delivery.
- IGRT: Daily imaging (e.g., Cone Beam CT - CBCT) ensures treatment accuracy. Essential for precision.
- SBRT/SABR: High dose/fraction (e.g., 1-5 fx); for small extracranial tumors.
⭐ SBRT: ablative doses, high precision; boosts local control (e.g., early lung cancer, oligometastases).
- SRS: Single high-dose fraction for intracranial lesions.
- Proton Therapy: Bragg peak spares distal tissues; minimal exit dose.
Radiobiology & Reactions - Cell Battle & Aftermath
- Radiation damages DNA: Indirect action (water radiolysis, $OH^{\cdot}$ free radicals) is dominant over direct action. Double-Strand Breaks (DSBs) are most lethal.
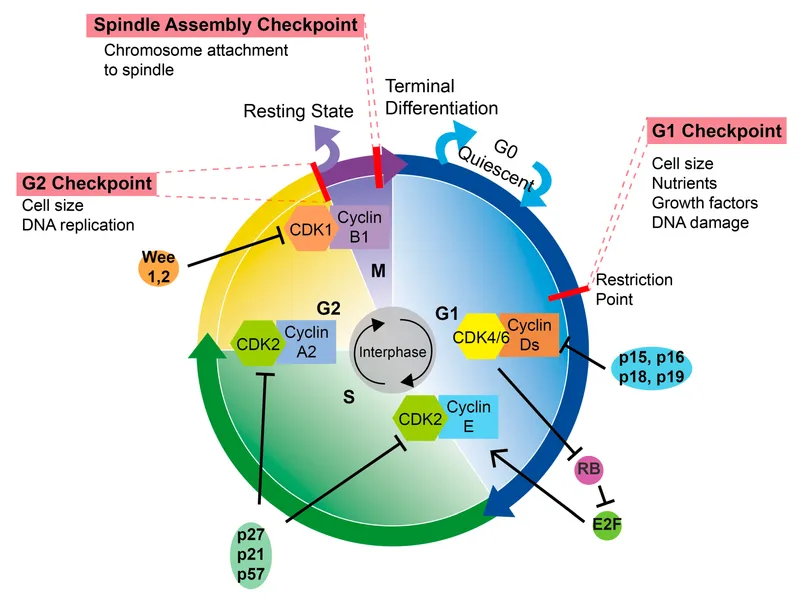
- Cell cycle sensitivity: M & G2 phases are most sensitive; late S phase is most resistant.
- The 4 R's of Radiobiology: Repair (of sublethal damage), Repopulation (of cells), Redistribution (of cells in cycle), Reoxygenation (of hypoxic tumor cells).
- Acute reactions: Occur during or shortly after RT (e.g., mucositis, dermatitis). Typically reversible.
- Late reactions: Occur months to years post-RT (e.g., fibrosis, necrosis). Often permanent & dose-limiting.
⭐ Tissues with high radiosensitivity include lymphoid, hematopoietic, and gonadal tissues. Muscle and CNS are relatively radioresistant.
High‑Yield Points - ⚡ Biggest Takeaways
- LINACs (Linear Accelerators) are the primary EBRT machines, delivering photon (most common) or electron beams (for superficial tumors).
- Teletherapy is treatment from a distance, contrasting with brachytherapy.
- Fractionation (dividing the total dose into multiple smaller daily doses) is key to spare normal tissue and improve tumor kill over weeks.
- Modern techniques like IMRT (Intensity-Modulated Radiation Therapy) and VMAT (Volumetric Modulated Arc Therapy) allow high dose conformity to the tumor, sparing OARs (Organs at Risk).
- IGRT (Image-Guided Radiation Therapy) ensures daily treatment accuracy by verifying patient and tumor position.
- Acute side effects (e.g., dermatitis, mucositis, fatigue) are common, site-dependent, and generally manageable.
- Late effects can include fibrosis, organ dysfunction, and a small risk of radiation-induced secondary cancers years later.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more