Introduction & Principles - Close Quarters Combat
Brachytherapy ("short-distance" therapy): Radioactive sources are placed directly into or very near the tumor. Rationale: To deliver a high, concentrated radiation dose to the tumor while minimizing exposure to surrounding healthy tissues, leveraging rapid dose fall-off.
- Advantages:
- High dose conformity to target.
- ↓ radiation toxicity to normal tissues.
- Potentially shorter overall treatment time (in select cases).
- Disadvantages:
- Invasive procedure.
- Risk of radiation exposure to medical staff.
- Limited to localized and accessible tumors.
Underlying Physics: The Inverse Square Law is fundamental. Radiation intensity ($I$) from a point source decreases with the square of the distance ($d$) from the source: $I \propto 1/d^2$. This explains the steep dose gradient.
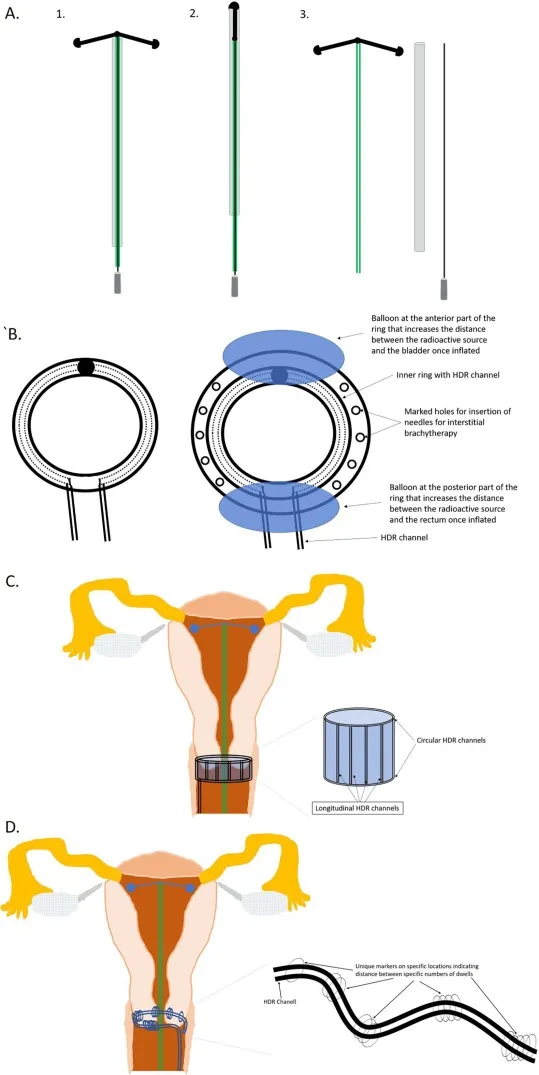
⭐ Brachytherapy allows for significant dose escalation to the tumor volume, which can lead to improved local control rates, particularly in cancers like cervical, prostate, and some head & neck sites when compared to External Beam Radiation Therapy (EBRT) alone.
📌 Remember: Close contact, High dose to tumor, Sharp fall-off protects normal tissue (CHS).
Sources & Classification - Radioactive Seeds & Systems
Radioactive Sources: Key isotopes:
| Isotope | Sym | Half-life | Energy (MeV) | Type | Uses |
|---|---|---|---|---|---|
| Iridium-192 | Ir-192 | 73.8 d | 0.38 (avg $\gamma$) | LDR/HDR | Interstitial, Intracavitary |
| Iodine-125 | I-125 | 59.4 d | 0.028 (avg $\gamma$) | LDR | Prostate, Eye |
| Palladium-103 | Pd-103 | 17 d | 0.021 (avg $\gamma$) | LDR | Prostate |
| Cesium-137 | Cs-137 | 30.2 y | 0.662 ($\gamma$) | LDR | GYN (hist.), Intracavitary |
| Strontium-90 | Sr-90 | 29 y | Y-90 (2.28 $\beta$) | LDR | Surface (Pterygium) |
Dose Rate Classification: 📌 LDR (Low & Long), HDR (High & Hurry)
| Rate | Dose Rate ($Gy/hr$) | Duration | Examples |
|---|---|---|---|
| LDR | 0.4-2 | Days | Prostate seeds, GYN (old) |
| MDR | 2-12 | Hours | Some GYN, H&N |
| HDR | >12 | Mins/frac | GYN, Bronchus, Esoph, Breast |
| PDR | Pulsed (~1 $Gy/pulse$) | Hrs (pulses) | Mimics LDR radiobiologically |
- Interstitial: In tissue (prostate, breast).
- Intracavitary: In cavity (GYN, esophagus).
- Intraluminal: In lumen (bronchus, bile duct).
- Surface: On skin/eye (skin Ca, pterygium).
- IORT: Surgery, tumor bed.
Loading Techniques:
- Manual: Historical, ↑staff exposure.
- Remote Afterloading: Standard, remote load, ↓staff exposure.
⭐ Ir-192: versatile for LDR/HDR; optimal half-life & gamma energy.
LDR vs. HDR Choice:
Applications & Techniques - Precision Strikes
Brachytherapy delivers highly conformal radiation directly to/near the tumor, sparing normal tissues.
- Temporary Implants: Sources removed after treatment (e.g., HDR for cervix, breast).
- Permanent Implants (Seeds): Sources remain indefinitely (e.g., LDR for prostate - I-125, Pd-103).
Common Brachytherapy Applications:
| Site | Isotopes | Technique/Applicator | Key Point / Dose Example |
|---|---|---|---|
| Cervix | Ir-192, Cs-137 | Tandem & Ovoids (Fletcher-Suit, Manchester), Interstitial | Point A: 80-85 Gy (EQD2) |
| Prostate | I-125, Pd-103 (LDR); Ir-192 (HDR) | LDR seeds; HDR catheters | LDR: 145 Gy (I-125) |
| Breast | Ir-192 | APBI (Interstitial, MammoSite) | APBI: 34 Gy/10 fr |
| H&N (e.g. Lip, Tongue) | Ir-192 | Interstitial, Moulds | Boost/Monotherapy |
| Skin | Ir-192, Sr-90 | Moulds, Applicators | Superficial lesions |
| Lung (Endobronchial) | Ir-192 (HDR) | HDR catheter | Palliation, Boost |
| Esophagus | Ir-192 (HDR) | Intraluminal HDR | Palliation |
⭐ Point A (cervical Ca): 2 cm superior to cervical os & 2 cm lateral to tandem. Crucial for dose prescription.
Dosimetry & Safety - Dose, Dangers, Defense
- Dosimetry & Planning Goals:
- ICRU reference points guide dose reporting.
- DVH analysis: D90 (e.g., >95% PTV coverage), V100 (target volume receiving 100% dose), OAR dose constraints (e.g., V20 for rectum).
- Brachytherapy Workflow:
- Radiation Safety (📌 ALARA):
- Time: Minimize exposure duration.
- Distance: Maximize distance from sources (inverse square law).
- Shielding: Use barriers (lead, concrete) for staff/public.
- Complications:
- Acute: Mucositis, dermatitis, pain, swelling. Resolve with supportive care.
- Late: Fibrosis, necrosis, strictures, fistulae. Site-specific, potentially permanent.
⭐ High Dose Rate (HDR) brachytherapy allows for outpatient treatment and optimized dose distributions due to source stepping ability during treatment delivery for complex target volumes near critical structures.
High‑Yield Points - ⚡ Biggest Takeaways
- Brachytherapy delivers radiation internally, with sources placed close to or inside the tumor.
- Key types include Low Dose Rate (LDR) for continuous exposure and High Dose Rate (HDR) for short, intense treatments.
- Common isotopes: Iridium-192 (most common for HDR), Iodine-125, Palladium-103 (LDR permanent implants like prostate seeds).
- Offers high localized dose to the target volume, significantly sparing surrounding healthy tissues due to rapid dose fall-off.
- Widely used for cervical, prostate, breast, esophageal, and skin cancers.
- The inverse square law (I ∝ 1/d²) is a fundamental principle governing its dose distribution.
- Manchester system and Paterson-Parker rules are historical systems for dose calculation, especially in gynecological applications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

