Pre-sedation Assessment - Prepping for Peace
- Goal: Ensure patient safety & successful sedation for imaging.
- Key Steps:
- History: Medical, surgical, anaesthetic history; allergies; medications; NPO status (last oral intake).
- Examination: Airway (e.g., Mallampati, neck mobility), CVS, RS, CNS. Assign ASA physical status.
- NPO Guidelines: Adherence critical. 📌 "2-4-6-8 Rule" as quick recall.
⭐ Current NPO: Clear liquids ≥2h, breast milk ≥4h, infant formula/non-human milk/light meal ≥6h, solids/fried/fatty meal ≥8h before elective procedures.
- Consent: Informed, written consent obtained.
- Investigations: Usually not indicated for healthy children (ASA I or II).
Pharmacological Agents - Potions & Protocols
Selection guided by procedure, patient status, and available expertise. Always ensure availability of resuscitation equipment and reversal agents.
- Titrate to effect for desired sedation level.
- Continuous monitoring of vitals (HR, RR, SpO2, BP) is mandatory.
- Strict adherence to NPO guidelines is crucial.
| Agent | Dose | Onset | Duration | Pros | Cons | Reversal (IV Dose) |
|---|---|---|---|---|---|---|
| Midazolam | PO: 0.25-1 mg/kg; IV: 0.05-0.1 mg/kg; IN: 0.2-0.5 mg/kg | IV: 1-3m | 30-60m | Anxiolysis, amnesia | Resp. depression, paradox. agitation | Flumazenil (0.01 mg/kg) |
| Fentanyl | IV: 1-2 mcg/kg | 1-2m | 30-60m | Potent analgesia | Resp. depression, chest rigidity | Naloxone (0.01-0.1 mg/kg) |
| Ketamine | IV: 0.5-2 mg/kg; IM: 2-5 mg/kg | IV: <1m | 10-40m | Dissociative, analgesia, bronchodilation, sympathomimetic | Emergence reactions, ↑secretions | Supportive (BZD for emergence) |
| Propofol | IV Bolus: 1-3 mg/kg; Infusion: 50-200 mcg/kg/min | <1m | 5-10m | Rapid onset/recovery, antiemetic | Hypotension, resp. depression, PRIS ⚠️ | Supportive |
| Chloral Hydrate | PO/PR: 25-100 mg/kg (max 2g) | 30-60m | 60-120m | Oral/rectal route | Paradoxical excitement, no analgesia, prolonged sedation, arrhythmogenic | Supportive |
Intra-sedation Monitoring - Guardian Duty
- Core Monitoring (Continuous):
- Pulse oximetry (SpO2 > 94%, alarm < 90%).
- Heart rate, rhythm.
- Respiratory rate, pattern, effort.
- Capnography (ETCO2): detects hypoventilation.
- Blood pressure (NIBP q5min).
- Level of consciousness.
- Essential Equipment:
- Oxygen source, delivery systems.
- Bag-Valve-Mask (BVM), suction.
- Airway adjuncts (OPA, NPA).
- Reversal agents, resuscitation drugs.
- Personnel: Dedicated trained individual (PALS certified) for monitoring.
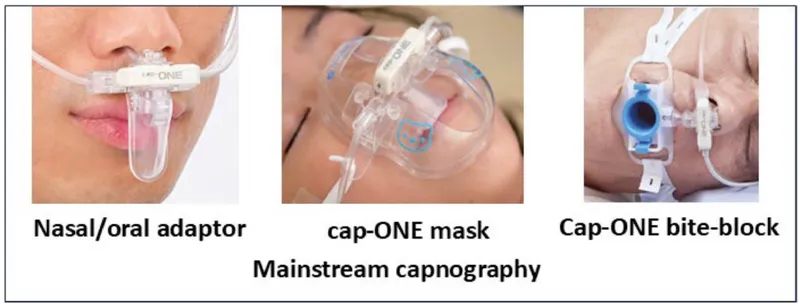
⭐ Capnography is the most sensitive indicator of early respiratory depression, apnea, and airway obstruction.
Complications & Discharge - Crisis Control
- Complications:
- Respiratory: Hypoventilation, apnea, laryngospasm, desaturation (O₂↓).
- Cardiovascular: Hypotension, bradycardia, arrhythmias.
- GI: Vomiting (aspiration risk).
- CNS: Paradoxical agitation, prolonged sedation.
- Crisis Control (ABCs):
- Airway: Maneuvers, O₂, suction.
- Breathing: BMV, supplemental O₂, consider reversal.
- Circulation: IV fluids, vasopressors.
- Discharge (Aldrete Score ≥9):
- Vitals stable & age-appropriate (HR, RR, BP, SpO₂).
- Awake, alert, baseline neuro status.
- Tolerates oral intake.
- Responsible escort present.
⭐ Reversal Doses:
- Flumazenil (Benzos): 0.01 mg/kg IV (max 0.2 mg/dose; total 1 mg).
- Naloxone (Opioids): 0.01 mg/kg IV (<5y/<20kg); 0.1 mg/kg IV (>5y/>20kg). Max 2mg/dose.
High‑Yield Points - ⚡ Biggest Takeaways
- Strict NPO guidelines (e.g., 2 hrs clear liquids, 6 hrs solids) are vital to prevent aspiration.
- Dexmedetomidine is preferred for procedural sedation due to its favorable safety profile and arousable sedation.
- Midazolam (intranasal/oral) is effective for anxiolysis pre-procedure.
- Comprehensive monitoring (pulse oximetry, capnography, vitals) is mandatory throughout.
- Always ensure availability of reversal agents (flumazenil, naloxone) and emergency equipment.
- Pre-sedation risk assessment using ASA status is crucial for patient safety.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

