Neonatal Brain & HIE - Tiny Brains, Big Worries
- Neonatal Brain:
- Germinal matrix: Vulnerable to Germinal Matrix Hemorrhage-Intraventricular Hemorrhage (GMH-IVH) in preterms.
- Myelination: Proceeds caudocranial, central-peripheral (T1↑, T2↓).
- Term: Posterior Limb Internal Capsule (PLIC), corona radiata normally myelinated.
- Hypoxic-Ischemic Encephalopathy (HIE):
- Etiology: Perinatal asphyxia.
- Term infant patterns:
- Partial prolonged (mild-moderate): Watershed zones (cortical/subcortical white matter).
- Acute profound (severe): Deep grey matter (basal ganglia, thalami), brainstem, perirolandic cortex.
- Preterm infant pattern: Predominantly Periventricular Leukomalacia (PVL).
- MRI findings:
- DWI: Restricted diffusion (earliest sign, within hours).
- MRS: ↑Lactate, ↓N-acetylaspartate (NAA).
- T1: Absent normal PLIC T1 hyperintensity (poor prognosis).
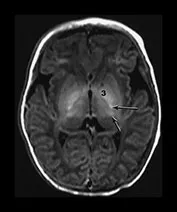
-
⭐ Deep grey matter (basal ganglia, thalami) injury on MRI in term neonates with HIE signifies severe insult and predicts adverse neurodevelopmental outcomes, especially if associated with lactate peak on MRS and restricted diffusion on DWI.
Congenital Anomalies - Brain's Blueprint Gone Wrong
- Neural Tube Defects (NTDs)
- Anencephaly: Absent cerebrum & calvarium; "frog-eye" sign on USG.
- Encephalocele: Herniation of brain/meninges; occipital commonest.
- Chiari Malformations:
- Type I: Tonsillar ectopia >5mm below foramen magnum (adults), >6mm (children).
- Type II: Assoc. w/ myelomeningocele. Cerebellar vermis/medulla herniation, tectal beaking, hydrocephalus.
⭐ Chiari II malformation is almost invariably associated with lumbosacral myelomeningocele.
- Forebrain Induction Disorders
- Holoprosencephaly (HPE): Incomplete cleavage of prosencephalon. Alobar (monoventricle, fused thalami), Semilobar, Lobar. Midline facial anomalies common.
- Neuronal Migration Disorders
- Lissencephaly: "Smooth brain"; agyria/pachygyria. "Hourglass" or "figure-8" appearance on axial MRI.
- Heterotopia: Neurons in abnormal locations (e.g., subependymal, band).
- Schizencephaly: CSF-filled clefts lined by gray matter, extending from pial surface to ventricle.
- Other Key Anomalies
- Dandy-Walker Malformation: Cystic dilation of 4th ventricle, cerebellar vermian hypoplasia/agenesis, elevated torcula.
- Joubert Syndrome: "Molar tooth sign" on axial MRI (deep interpeduncular fossa, thick superior cerebellar peduncles).

- Destructive Lesions
- Hydranencephaly: Near-total absence of cerebral hemispheres, replaced by CSF; falx present, thalami/brainstem spared. Caused by bilateral ICA occlusion in utero.
Pediatric CNS Infections & Tumors - Invaders & Overgrowths
- CNS Infections:
- Neonatal: GBS, E.coli. Complications: ventriculitis, hydrocephalus.
- TORCH: CMV (periventricular calcifications, white matter changes, migrational anomalies), Toxoplasmosis (hydrocephalus, diffuse intracranial & basal ganglia calcifications).
- Bacterial Meningitis: Leptomeningeal enhancement, subdural empyema.
- Brain Abscess: Ring enhancement, central restricted diffusion (DWI).
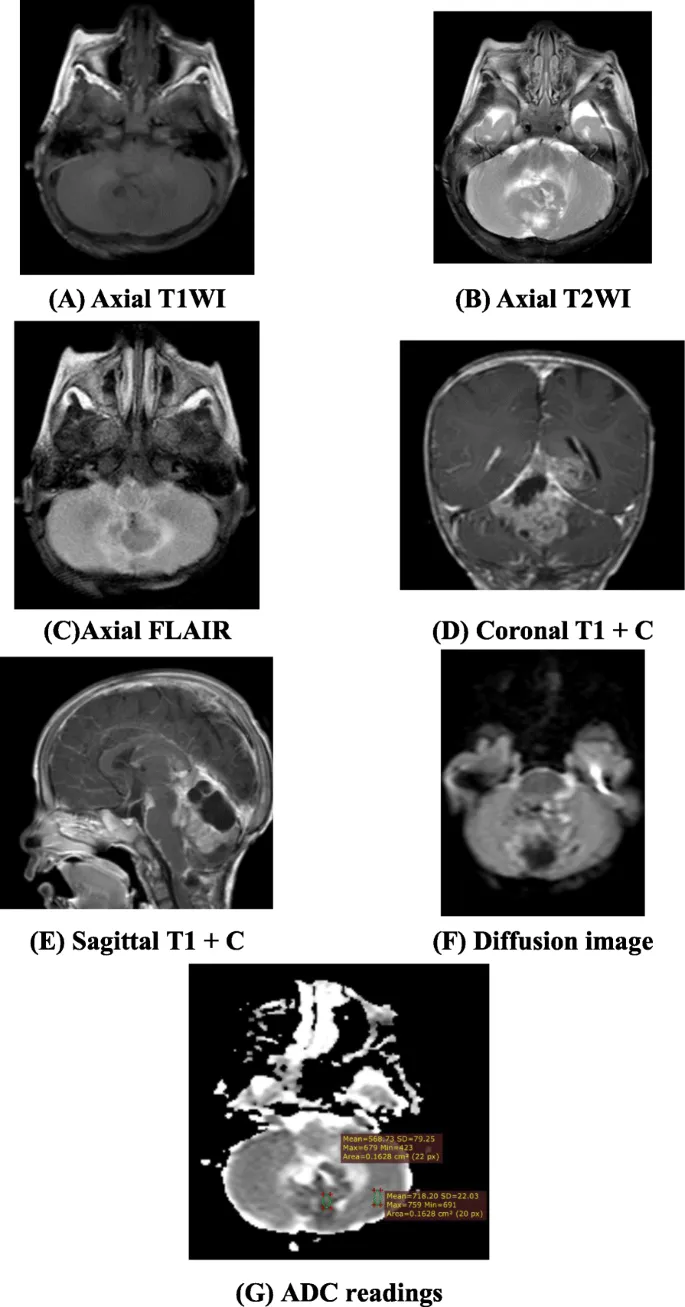
- CNS Tumors (Posterior Fossa commonest): 📌 My Apple Eats Bugs (Medulloblastoma, Astrocytoma, Ependymoma, Brainstem glioma).
- Medulloblastoma: Midline (vermis), hyperdense (CT), ↓ADC, hydrocephalus.
⭐ Medulloblastoma: Most common malignant pediatric brain tumor; often shows "Zuckerguss" (drop metastases) on spinal MRI.
- Pilocytic Astrocytoma: Cystic with enhancing mural nodule (cerebellum/optic pathway).
- Ependymoma: 4th ventricle, "plastic" (through foramina Luschka/Magendie), calcification.
- Brainstem Glioma (DIPG): Diffuse pontine enlargement, engulfs basilar artery, poor prognosis.
- Craniopharyngioma (Suprasellar): Cystic, calcification (adamantinomatous), "motor oil" cyst.
- Medulloblastoma: Midline (vermis), hyperdense (CT), ↓ADC, hydrocephalus.
Neurotrauma & Metabolic Disorders - Ouch & Oops
- Neurotrauma:
- EDH: Arterial, biconvex (lens-shaped). Lucid interval.
- SDH: Venous, crescent-shaped. Bridging veins. Interhemispheric in NAI.

- DAI: Shearing forces. Corpus callosum, brainstem. Petechial hemorrhages.
- NAI: ⚠️ Inconsistent history.
- Multiple healing fractures, metaphyseal lesions.
- Retinal hemorrhages.
- Interhemispheric SDH, posterior rib #.
- Metabolic Disorders:
- HIE: Basal ganglia, thalami, watershed zones. Pattern varies (age/severity).
- Kernicterus: Bilirubin in globus pallidus, subthalamic nucleus, hippocampus.
- MSUD: "MSUD edema": cerebellar white matter, brainstem, corticospinal tracts. Sweet odor.
- Leigh Disease: Symmetrical basal ganglia, brainstem, periaqueductal grey. ↑Lactate (MRS).
- Canavan Disease: ↑NAA (MRS). Spongy degeneration. Diffuse white matter swelling, macrocephaly.
⭐ Interhemispheric subdural hematomas and posterior rib fractures are highly specific NAI findings.
High‑Yield Points - ⚡ Biggest Takeaways
- Posterior fossa tumors (e.g., medulloblastoma, pilocytic astrocytoma) are common in children.
- Dandy-Walker malformation: Cystic 4th ventricle, vermian hypoplasia/agenesis, enlarged posterior fossa.
- Chiari II malformation is strongly associated with myelomeningocele and hydrocephalus.
- Neonatal HIE: Term infants show basal ganglia/thalamic injury; preterm show PVL.
- TORCH infections: CMV causes periventricular calcifications; Toxoplasmosis causes diffuse calcifications.
- NF1: Optic nerve gliomas, sphenoid wing dysplasia, UBOs. Tuberous Sclerosis: SENs, cortical tubers, SEGAs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

