Normal Growth & Variants - Bones in Bloom
- Ossification Centers: Primary (diaphysis), Secondary (epiphysis). Appearance/fusion age varies (e.g., elbow: CRITOE 📌).
- Order of elbow ossification: Capitellum (1yr), Radial head (3yr), Internal (medial) epicondyle (5yr), Trochlea (7yr), Olecranon (9yr), External (lateral) epicondyle (11yr).
- Physes (Growth Plates): Cartilaginous; weakest part of growing bone. Salter-Harris fractures involve physis.
- Zones: Resting, Proliferative, Hypertrophic (weakest), Calcification.
- Apophyses: Secondary ossification centers at tendon/ligament attachments (e.g., tibial tuberosity - Osgood-Schlatter, calcaneal - Sever's).
- Prone to avulsion fractures.
- Normal Variants Mimicking Fractures:
- Bipartite patella (superolateral fragment)
- Os trigonum (posterior to talus)
- Accessory navicular
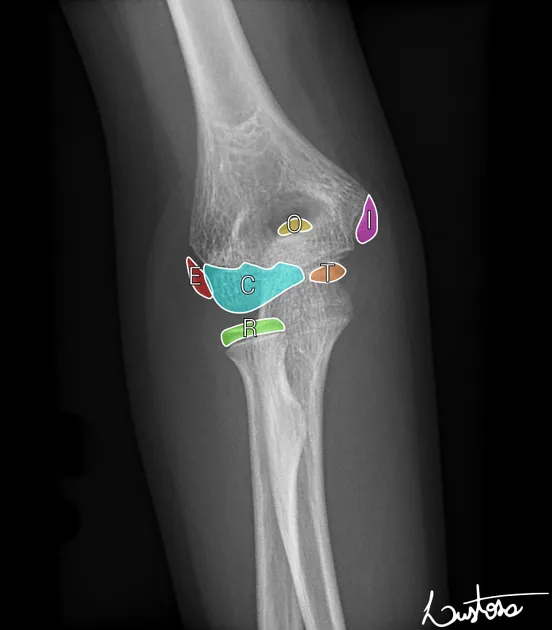
⭐ The physis is radiolucent and represents the weakest point in a child's bone, making it susceptible to Salter-Harris fractures, which can affect growth if not managed properly (especially types III, IV, V).
Pediatric MSK Trauma - Twigs & Snaps
- Incomplete Fractures (Elastic bones):
- Torus/Buckle: Compression causes cortex to bulge.
- Greenstick: Tension side breaks, compression side bends.
- Plastic Bowing: Bone bends, no distinct fracture line.
- Salter-Harris (Growth Plate Injuries) 📌 SALTER:
- I: Slipped (through physis)
- II: Above (physis + metaphysis) - Most common.
- III: Lower (physis + epiphysis)
- IV: Through (metaphysis, physis, epiphysis)
- V: Rammed (crush of physis)
- Common Sites: Supracondylar (elbow), distal radius.
- NAI Clues:
- Metaphyseal corner/bucket-handle fractures.
- Posterior rib fractures (squeezing).
- Multiple fractures, varied healing stages.
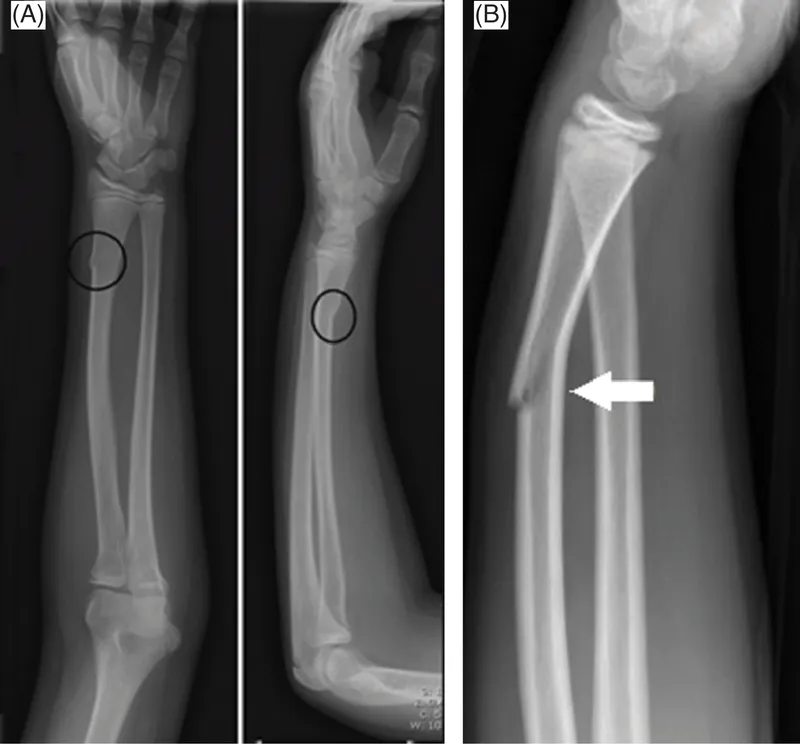
⭐ Salter-Harris Type II fractures are the most common type of physeal injury.
MSK Infections/Inflammation - Fiery Joints & Bones
- Osteomyelitis:
- Spread: Hematogenous (metaphysis in children), direct, contiguous.
- X-ray: Early: soft tissue swelling. Late (10-14 days): periosteal reaction, lytic lesions, sequestrum.
- US: Subperiosteal fluid/abscess, soft tissue edema.
- MRI: Most sensitive for early changes (marrow edema, abscess).
- Septic Arthritis: (Esp. Hip)
- US: Joint effusion (key!), synovial thickening. 📌 US guides aspiration.
- MRI: Cartilage/bone involvement, synovitis.
- Juvenile Idiopathic Arthritis (JIA):
- Key features: Periostitis, erosions (marginal), joint space narrowing (late), osteopenia. Affects large joints (knee, ankle, wrist).
⭐ MRI is the most sensitive imaging modality for early diagnosis of osteomyelitis, detecting marrow changes within 24-48 hours of onset.
Developmental Dysplasia of Hip (DDH) - Hip Hip Hooray?
- Risk Factors: 📌 Female, Firstborn, Family Hx, Frank breech, Oligohydramnios.
- Clinical: Barlow (provocative, dislocates), Ortolani (reductive, relocates), Galeazzi sign.
- Imaging:
- Ultrasound (<4-6m): Graf classification.
- Alpha angle (bony roof): Normal > 60°.
- Beta angle (cartilage roof).
- X-ray (>4-6m):
- Lines: Hilgenreiner (H), Perkin (P), Shenton (S-arch).
- Acetabular Index (AI): Normal < 25-30° (↑ in DDH).
- Center-Edge Angle (CE): Normal > 20-25° (↓ in DDH).

- Ultrasound (<4-6m): Graf classification.
⭐ Shenton's line disruption is a key X-ray sign indicating hip subluxation or dislocation.
Common Pediatric MSK Conditions - Growing Pains Plus
-
Legg-Calvé-Perthes (LCPD): Avascular necrosis, femoral head.
- Stages: Incipient, Fragmentation, Re-ossification, Healed.
- X-ray: Crescent sign, ↑medial joint space.
-
SCFE (Slipped Capital Femoral Epiphysis): Femoral epiphysis slips posteroinferiorly.
- Klein's line (AP view): Fails to intersect lateral epiphysis.
- Grading: Mild (<30% slip), Moderate (30-50%), Severe (>50%).
-
Rickets: Defective physeal mineralization. X-ray: Physeal cupping, fraying.
-
Benign Bone Lesions:
- Non-ossifying fibroma (NOF): Eccentric, cortically based, sclerotic rim.
- Osteochondroma: Cartilage-capped bony projection from metaphysis.
- Simple Bone Cyst (SBC): Central, lytic, well-defined.
⭐ SCFE is a common hip disorder in adolescents; bilateral involvement occurs in 20-40% of cases, often within 18 months of initial presentation on one side.
High‑Yield Points - ⚡ Biggest Takeaways
- DDH: Ultrasound < 6 months (Graf), X-ray > 6 months (Hilgenreiner, Perkin, Shenton lines).
- SCFE: Klein's line fails to intersect epiphysis; "ice cream off cone" sign.
- Legg-Calvé-Perthes: Avascular necrosis of femoral head; stages include fragmentation, re-ossification.
- Rickets: Widened, cupped, frayed physes; bowing deformities.
- NAI: Suspect with metaphyseal corner fractures, posterior rib fractures, multiple healing-stage fractures.
- Salter-Harris fractures: Involve growth plate; Type II most common.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

