Neonatal Obstruction - Blocked Pipes & Twisted Guts
Error generating content for this concept group: No object generated: the tool was not called.
Inflammation/Invagination - Fiery Bellies & Telescopes
Necrotizing Enterocolitis (NEC)
- Acute bowel inflammation/necrosis, mainly in premature infants. Risk factors: prematurity, formula feeding.
- Key X-ray findings:
- Pneumatosis intestinalis (intramural air) - hallmark.
- Portal venous gas (severe sign).
- Pneumoperitoneum (indicates perforation).
- Bell's Staging guides management. Complications: strictures, short bowel syndrome.
Intussusception
-
Telescoping of bowel segment; commonest cause of obstruction in children < 2 years (peak 6-36 months).
-
Typically ileocolic & idiopathic. Lead point (e.g., Meckel's diverticulum, polyp) more common in older children or recurrent cases.
-
Clinical: Sudden, severe, colicky abdominal pain; vomiting; red currant jelly stool (late sign). Palpable sausage-shaped mass.
-
Diagnosis & Management Flow:
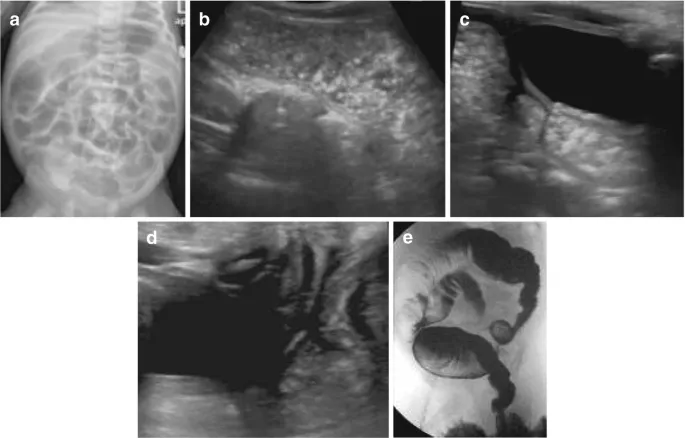
⭐ "Target sign" (concentric rings) on ultrasound is pathognomonic for intussusception.
Pediatric Abdominal Masses - Lumpy Tummy Terrors
- Wilms' Tumor (Nephroblastoma):
- Most common renal tumor (peak 3-4 yrs).
- Intrarenal, well-circumscribed, "claw sign".
- Assoc: WAGR, Denys-Drash, Beckwith-Wiedemann.
- Neuroblastoma:
- Most common extracranial solid tumor (median age <2 yrs).
- Adrenal/sympathetic chain; crosses midline; calcifications.
- ↑ VMA/HVA; N-myc. 📌 "N"euroblastoma: N-myc, Near midline, Nerve origin.
- Hepatoblastoma:
- Most common primary malignant liver tumor (peak 1-2 yrs).
- Solitary, large, ↑ AFP.
- Assoc: Beckwith-Wiedemann, FAP.
- Teratoma:
- Germ cell tumor; sacrococcygeal common.
- Mixed: solid, cystic, fat, calcification.
⭐ Neuroblastoma often presents with calcifications (seen in up to 85% on CT) and commonly crosses the midline, distinguishing it from Wilms' tumor which is typically intrarenal and does not cross the midline as frequently or extensively.
Hepatobiliary & Bowel - Yellow Babies & Lazy Bowels
- Biliary Atresia (BA):
- Conjugated hyperbilirubinemia (onset 2-8 wks).
- USG: Triangular Cord Sign (TCS) >4mm, small/absent GB, no post-feed contraction.
- HIDA (post-phenobarb): No bowel excretion at 24 hrs.
- Kasai <60-90 days.
- Choledochal Cyst:
- Todani Type I (most common). Cystic biliary dilatation.
- USG/MRCP diagnosis.
- Risks: Cholangitis, cholangiocarcinoma.
- Neonatal Hepatitis:
- Dx of exclusion. HIDA: Normal uptake, ↓/delayed excretion.
- Hirschsprung Disease (HD):
- Aganglionosis (distal bowel, rectosigmoid).
- Delayed meconium (>48 hrs).
- Contrast Enema: Transition zone, rectosigmoid ratio <1.
- Biopsy: Gold std (absent ganglion cells).
⭐ Triangular Cord Sign (TCS) on USG: >4mm echogenic density anterior to portal vein, highly specific for Biliary Atresia.
High‑Yield Points - ⚡ Biggest Takeaways
- Necrotizing Enterocolitis (NEC): Pneumatosis intestinalis is key; portal venous gas signifies severity.
- Intussusception: Target sign or doughnut sign on USG; air/contrast enema for diagnosis & therapy.
- Hypertrophic Pyloric Stenosis (HPS): USG shows pyloric muscle >3 mm thick, canal >14 mm long.
- Malrotation with Volvulus: Upper GI series shows corkscrew sign; USG may show whirlpool sign.
- Hirschsprung's Disease: Contrast enema reveals transition zone; rectal biopsy confirms.
- Wilms' Tumor: Most common childhood renal malignancy; claw sign on imaging.
- Neuroblastoma: Common extracranial solid tumor, often adrenal; may show calcifications on imaging.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

