Neonatal CXR - Breathing Pixels
Key CXR Interpretations:
- RDS (HMD): Premature; surfactant deficiency. Fine granular (ground-glass) opacities, air bronchograms, low lung volumes (↓volumes).
- TTN: Term/late preterm; delayed fluid clearance. Perihilar streaking, fissural fluid, increased lung volumes (↑volumes). Clears 24-72h.
- MAS: Term/post-term; meconium aspiration. Coarse, patchy infiltrates, hyperinflation. High risk of air leaks.
- Neonatal Pneumonia: GBS/E.coli; infection. Asymmetric patchy infiltrates, consolidation, pleural effusion. Can mimic RDS.
- Pneumothorax: Air in pleural space. Lucency, absent markings, visceral pleural line. Deep sulcus sign (supine).
Line Positions (Verify!):
- ETT: Tip 1-2 cm above carina (T2-T3).
- UVC: IVC-RA junction (T8-T9).
- UAC: High (T6-T9) or Low (L3-L4).
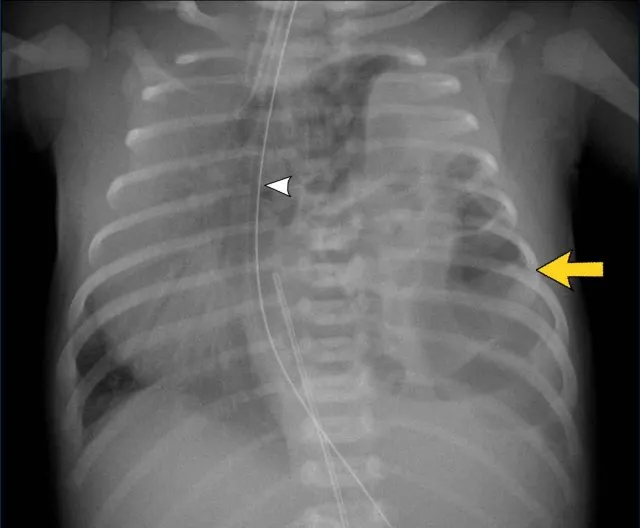
⭐ Sail sign (normal thymus) in neonatal CXR, not consolidation.
Neonatal Abdomen - Gut Reactions
- Necrotizing Enterocolitis (NEC):
- X-ray: Pneumatosis intestinalis (hallmark), portal venous gas (ominous), pneumoperitoneum (perforation: Rigler"s, football signs).
- Bell"s Staging (I-III).
- Congenital Obstructions:
- Duodenal Atresia: "Double bubble" sign (X-ray); no distal gas if complete.
- Jejunal/Ileal Atresia: Multiple dilated loops; microcolon (contrast enema).
- Malrotation ± Volvulus: UGI: abnormal DJ flexure, "corkscrew" duodenum. USG: "whirlpool" sign.
- Hirschsprung Disease: Delayed meconium (>24-48h). Contrast enema: transition zone, rectosigmoid ratio <1.
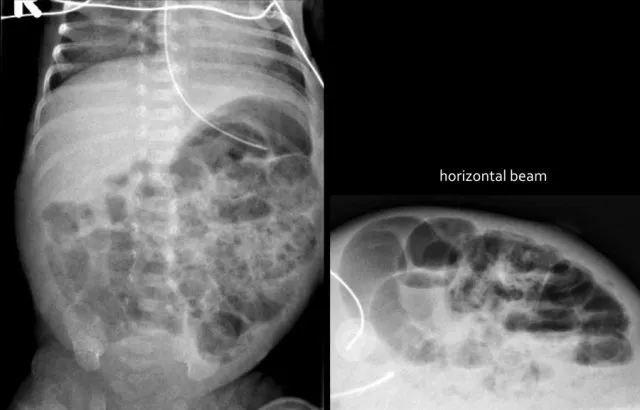
- Meconium Ileus: X-ray: "soap bubble" (Neuhauser), dilated loops. Enema: microcolon. Assoc. CF.
⭐ Portal venous gas in suspected NEC is ominous, indicating bowel necrosis and possible perforation.
Neonatal Neurosonography - Brainy Beams
- Role: First-line neuroimaging in neonates, especially preterm.
- Indications: Prematurity (<32 wks, <1500g), HIE, seizures, infection, hydrocephalus.
- Views: Standard coronal & sagittal via anterior fontanelle.
- Optional: posterior fontanelle, mastoid.
- Pathologies Detected:
- Intraventricular Hemorrhage (IVH): Papile Grading:
- I: Germinal matrix (GMH).
- II: IVH, no ventricular dilatation.
- III: IVH + ventricular dilatation.
- IV: IVH + intraparenchymal hemorrhage.
- Periventricular Leukomalacia (PVL): Early echogenicity → cysts.
- Hydrocephalus: ↑Ventricular size.
- Intraventricular Hemorrhage (IVH): Papile Grading:
- Pros: Bedside, radiation-free, real-time, repeatable.
⭐ The germinal matrix, highly vascular and fragile, is the primary site of hemorrhage in preterm infants, typically before 32-34 weeks gestation.
Lines & Tubes - Placement Puzzles
- Endotracheal Tube (ETT):
- Ideal: Tip 1-2 cm above carina; mid-trachea (T2-T4).
- Malpositions: R main bronchus, esophagus.
- Note: Neck flexion (↓ tip), extension (↑ tip).
- Umbilical Venous Catheter (UVC):
- Ideal: Tip at cavo-atrial junction (T8-T9).
- Path: Umbilical v. → L portal v. → ductus venosus → IVC.
- Malpositions: Portal vein (liver damage), RA (arrhythmia).
⭐ UVC tip ideally at the junction of IVC and right atrium (T8-T9 vertebral level).
- Umbilical Arterial Catheter (UAC):
- Ideal High: T6-T9 (avoids major branches). Low: L3-L4.
- Path: Umbilical a. → internal iliac a. → aorta.
- Malpositions: Too low/high, incorrect vessel.
- Nasogastric/Orogastric Tube (NGT/OGT):
- Ideal: Tip in stomach, below GE junction.
- Malpositions: Esophagus, coiled, tracheobronchial tree.
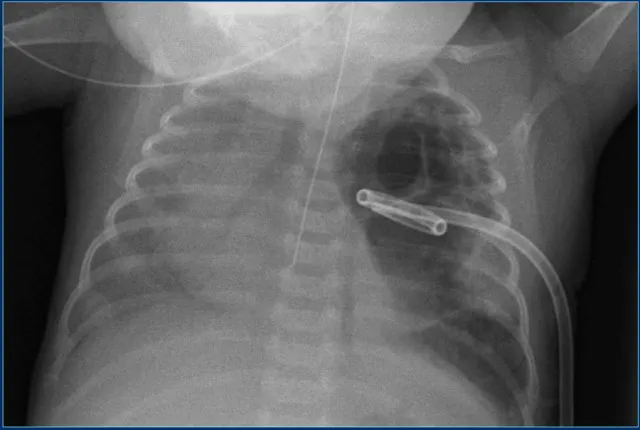
- Chest Tube (ICD):
- Pneumothorax: Apical. Effusion: Basal.
- All side holes within pleural space.
- PICC Line:
- Ideal: Tip lower SVC / cavo-atrial junction.
- Malpositions: Internal Jugular Vein (IJV), Right Atrium (RA).
High‑Yield Points - ⚡ Biggest Takeaways
- RDS: Characterized by diffuse ground-glass opacities, air bronchograms, and low lung volumes.
- TTN: Presents with perihilar streaking, fluid in fissures, and hyperaeration; resolves in 24-72 hours.
- MAS: Shows coarse, patchy infiltrates, hyperinflation, and increased risk of pneumothorax.
- NEC: Pneumatosis intestinalis is pathognomonic; look for portal venous gas or free air (perforation).
- CDH: Bowel loops in chest, mediastinal shift; Bochdalek hernia (left posterior) is most common.
- Duodenal Atresia: Exhibits the classic "double bubble" sign on X-ray; strongly associated with Trisomy 21.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

