Pediatric Neuro: Dev & Congenital - Brain Blueprints
- Neurulation (3-4 wks): Neural tube forms. Defects:
- Anencephaly: Absent cerebrum/vault, "frog-eye" sign.
- Encephalocele: Cranial content herniation, occipital common.
- Spina Bifida: Often with Chiari II malformation.
- Prosencephalic Development (5 wks): Forebrain cleavage. Defect:
- Holoprosencephaly (HPE): Alobar, semilobar, lobar. Facial anomalies common. ⭐ > Holoprosencephaly is strongly associated with maternal diabetes and Patau syndrome (Trisomy 13).
- Neuronal Migration (8-20 wks): Neurons travel to cortex. Defects:
- Lissencephaly: Smooth brain (agyria-pachygyria), "figure-8" MRI.
- Heterotopia: Ectopic gray matter.
- Organization (20 wks - postnatal): Cortical folding & layering. Defects:
- Polymicrogyria: Many small, disorganized gyri.
- Schizencephaly: Gray matter-lined CSF clefts.
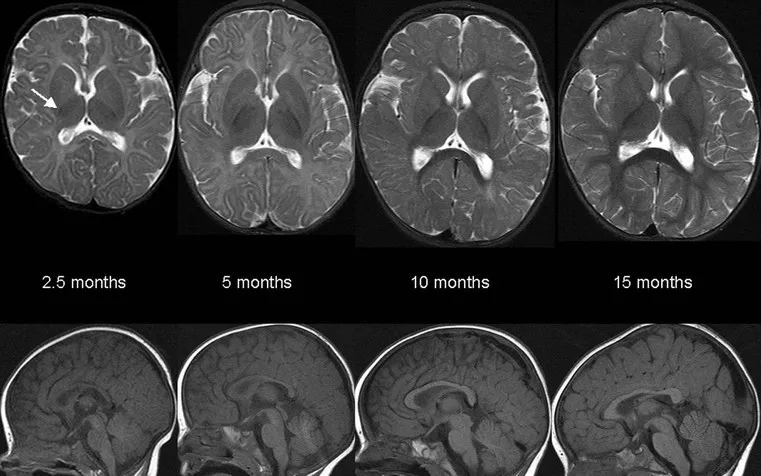
- Myelination (Birth - ~2 yrs): Pattern: Caudal→cranial, posterior→anterior, central→peripheral.
- MRI: T1W ↑ (hyperintense), T2W ↓ (hypointense) with maturation.
- Posterior Limb Internal Capsule (PLIC) myelinated by 7 months. Largely complete by 2 years.
Pediatric Neuro: HIE & Infections - Brain Battles
- Hypoxic-Ischemic Encephalopathy (HIE): Brain injury from O₂ deprivation.
- Term Infants:
- Pattern: Deep gray matter (basal ganglia, thalami), brainstem, perirolandic cortex, watershed zones.
- MRI: Early DWI changes (within 24-48 hrs), later T1 hyperintensity. MRS: ↑Lactate, ↓NAA.
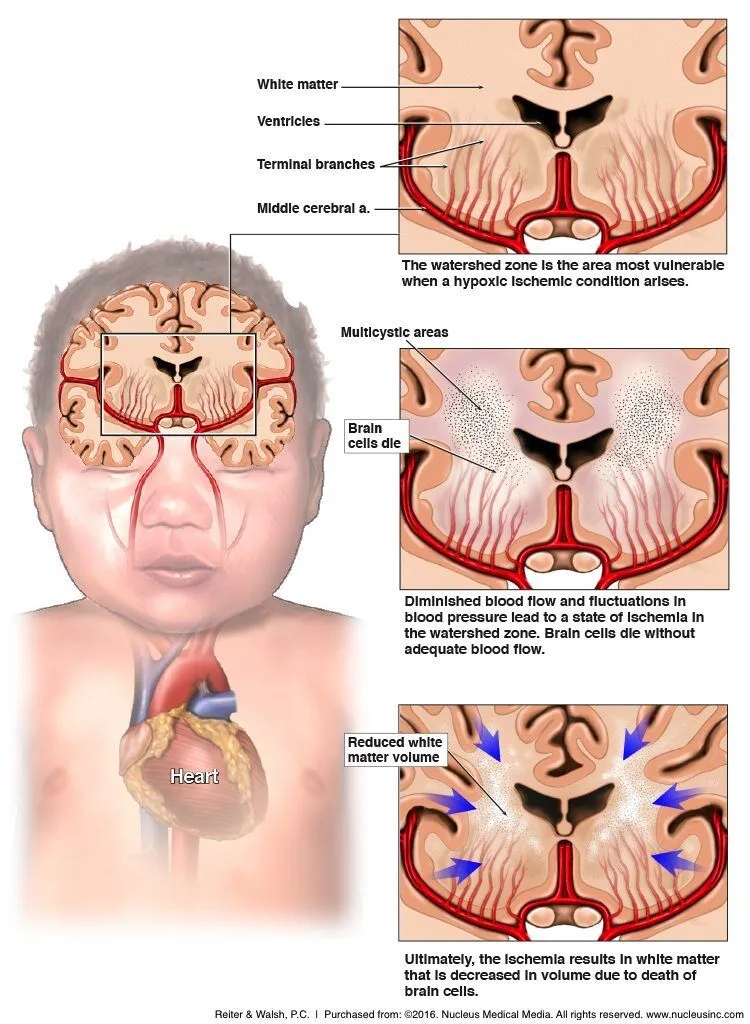
- Preterm Infants:
- Pattern: Periventricular Leukomalacia (PVL) - white matter injury, esp. near trigones.
- MRI: Cystic changes, gliosis.
- Term Infants:
- Infections:
- TORCH (Transplacental):
- CMV: Most common. Periventricular calcifications, ventriculomegaly, polymicrogyria, white matter abnormalities.
- Toxoplasmosis: Diffuse/basal ganglia calcifications, hydrocephalus, chorioretinitis (classic triad with convulsions).
- HSV: Hemorrhagic necrosis (temporal/frontal lobes), diffusion restriction early.
- Bacterial Meningitis:
- Complications: Hydrocephalus (communicating/obstructive), infarcts (vasculitis), empyema, ventriculitis, abscess.
- MRI: Leptomeningeal enhancement, DWI for pus/infarcts.
- TORCH (Transplacental):
⭐ CMV is the most common congenital infection causing brain abnormalities, classically presenting with periventricular calcifications and migrational defects like polymicrogyria.
Pediatric Neuro: Tumors - Tiny Tumors, Big Trouble
- General: Infratentorial common (childhood); supratentorial (infancy/adolescence).
- Medulloblastoma (PNET):
- Malignant. Cerebellar vermis. 📌 Malignant, Midline, Metastasis (CSF).
- Imaging: Hyperdense CT, restricted diffusion MRI, avid enhancement.
- Pilocytic Astrocytoma (WHO I):
- Most common benign. Cerebellum, optic pathway.
- Cystic with enhancing mural nodule ("cyst with a dot"). Rosenthal fibers.
- Ependymoma:
- 4th ventricle common. "Plastic tumor" - extends via foramina. Calcification (~50%).
- Craniopharyngioma:
- Suprasellar. Adamantinomatous (children): cystic, lobulated, calcification (90%), "machine oil".
- Germ Cell Tumors:
- Pineal (boys) or suprasellar. Germinoma (radiosensitive); Non-germinomatous (↑AFP/β-hCG).
⭐ Infratentorial tumors are more common than supratentorial tumors in children (approx. 2:1 ratio), reversing in adulthood. ``
Pediatric Neuro: Syndromes & Trauma - Skin & Skull Signs
- Neurocutaneous Syndromes (Phakomatoses):
- NF-1: Café-au-lait spots, axillary freckling, Lisch nodules. Skull: Sphenoid wing dysplasia, lambdoid suture defects.
- TSC: Ash-leaf spots (hypopigmented), facial angiofibromas, shagreen patch. Skull: Cortical/subependymal tubers (calcify), sclerotic lesions.
- Sturge-Weber Syndrome (SWS): Port-wine stain (facial nevus flammeus, V1 distribution). Skull: Gyriform cortical calcifications ("tram-track").
⭐ Sturge-Weber Syndrome: Unilateral facial port-wine stain (V1/V2), ipsilateral leptomeningeal angiomatosis, glaucoma. "Tram-track" gyriform calcifications on CT are pathognomonic.
- Encephalocraniocutaneous Lipomatosis (ECCL): Scalp lipomas, alopecia. Skull: Cranial asymmetry, intracranial lipomas.
- Pediatric Head Trauma - Skull Signs:
- Fractures: Linear, depressed, diastatic (suture separation > 2-3 mm), growing skull fracture (leptomeningeal cyst).
- Cephalohematoma: Subperiosteal, does not cross suture lines; may calcify.
- Caput Succedaneum: Subcutaneous edema, crosses suture lines; resolves quickly.
- Other Skull Findings:
- Craniosynostosis: Premature suture fusion (e.g., Apert, Crouzon syndromes).
- Wormian bones: Intrasutural bones (e.g., osteogenesis imperfecta, cleidocranial dysostosis).
High‑Yield Points - ⚡ Biggest Takeaways
- Medulloblastoma: Most common malignant pediatric brain tumor, typically posterior fossa.
- Hypoxic-Ischemic Encephalopathy (HIE): Term infants - basal ganglia/thalamus; Preterm - periventricular white matter.
- TORCH infections: CMV - periventricular calcifications; Toxoplasmosis - diffuse calcifications.
- Chiari II malformation is almost always associated with myelomeningocele.
- Neurofibromatosis Type 1 (NF1): Characterized by optic pathway gliomas and UBOs.
- Tuberous Sclerosis Complex (TSC): Presents with cortical tubers, subependymal nodules, and SEGAs.
- Dandy-Walker malformation: Key features are cystic dilation of 4th ventricle and vermian hypoplasia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

