Initial Imaging & Skull Fractures - Scan Smart, Spot Breaks
- Primary Scan: NCCT head is crucial for acute trauma.
- X-ray skull: Very limited role; mainly if CT unavailable.
- Key CT Indications:
- GCS < 15 (2h post-injury)
- Suspected open/depressed fracture
- Basal skull fracture signs (Battle's, raccoon eyes)
- Vomiting > 1 episode
- Age ≥ 65 years
- Retrograde amnesia > 30 min
- Dangerous mechanism
- Focal deficit, seizure
- Skull Fracture Types:
- Linear: Most common.
- Depressed: Fragment inward; surgery if > bone thickness.
- Basal: Clinical signs vital; CSF leak risk.
- Comminuted: Multiple fragments.
- Diastatic: Sutural separation (children).
- Growing: Leptomeningeal cyst (infants/young children).
⭐ NCCT head is the investigation of choice in acute head trauma, rapidly identifying life-threatening injuries.
EDH & SDH - Bleeds Between Layers
| Feature | Epidural Hematoma (EDH) | Subdural Hematoma (SDH) |
|---|---|---|
| Location | Between dura & skull inner table | Between dura & arachnoid |
| Vessel | Middle Meningeal Artery (arterial); skull fracture (pterion) | Bridging veins (venous); elderly/atrophy, coagulopathy |
| CT Shape | Biconvex (lentiform), hyperdense. 📌 "Lemon" | Crescentic, density varies (acute hyperdense). 📌 "Banana" |
| Sutures | Does NOT cross sutures | CROSSES sutures |
| Midline | Can cross midline reflections (falx/tentorium) | Limited by dural reflections (falx/tentorium) |
| Clinical | Lucid interval; rapid decline | Gradual onset; fluctuating consciousness |
⭐ The "lucid interval," a temporary improvement in neurological status after head trauma followed by rapid deterioration, is a classic presentation of EDH.
SAH & ICH/Contusions - Blood In Spaces & Substance
- Subarachnoid Hemorrhage (SAH): Blood in CSF spaces (sulci, cisterns).
- NCCT: Hyperdense CSF. Key sites: Sylvian fissure, basal cisterns.
- Causes: Trauma (overall #1), ruptured aneurysm (spontaneous #1).
- Complications: Vasospasm (Day 4-14), hydrocephalus.

- Intracerebral Hemorrhage (ICH) & Contusions: Blood in brain parenchyma.
- ICH: Frank bleed. Common: frontal, temporal lobes.
- Contusions: Cortical "bruises"; mixed density (hemorrhage + edema).
- Locations: Inferior frontal, anterior temporal (coup-contrecoup).
- May "blossom" (evolve) over 24-48h.
⭐ Overall most common cause of SAH is trauma; for spontaneous SAH, it's a ruptured berry aneurysm.
DAI, Herniation & Peds Pearls - Axons, Squeezes & Small Skulls
- Diffuse Axonal Injury (DAI)
- Mechanism: High-velocity rotational shear forces; axons stretch & tear.
- Key sites: Grey-white matter junction, corpus callosum (esp. splenium), brainstem (dorsolateral midbrain/pons).
- CT: Often normal or subtle petechial hemorrhages.
- MRI: Modality of choice. SWI/GRE for microhemorrhages; FLAIR/DWI for non-hemorrhagic lesions.
- 📌 Adams Staging: Grade 1 (lobar WM), Grade 2 (+corpus callosum), Grade 3 (+brainstem).
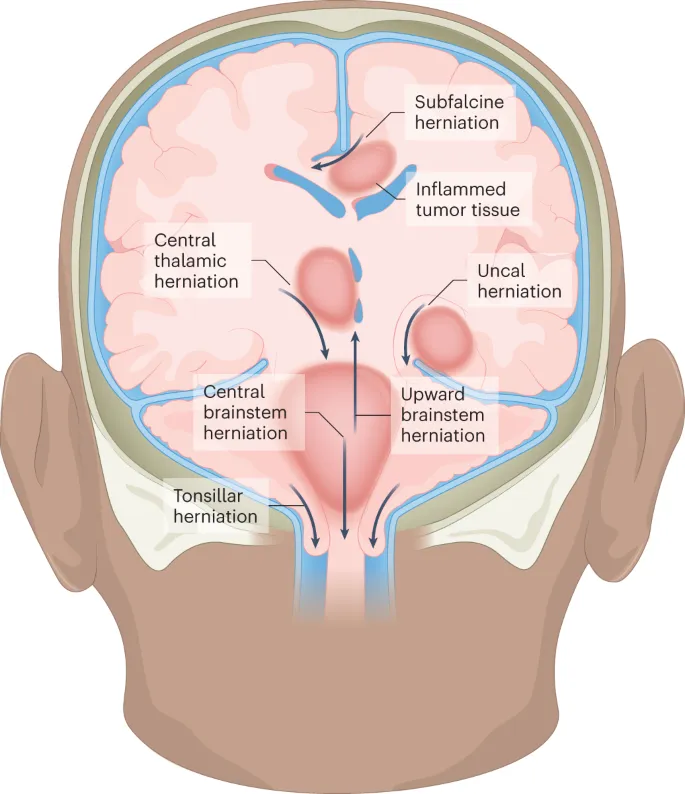
- Herniation Syndromes
- Subfalcine: Cingulate gyrus under falx → ACA compression.
- Uncal (Transtentorial): Medial temporal lobe (uncus) → CN III palsy (ipsilateral dilated pupil), contralateral hemiparesis (Kernohan's notch phenomenon). PCA often compressed.
- Central: Diencephalon/midbrain downward → Duret hemorrhages (secondary brainstem bleeds).
- Tonsillar: Cerebellar tonsils through foramen magnum → cardiorespiratory arrest.
- Pediatric Pearls
- Non-Accidental Injury (NAI): Suspect with interhemispheric SDH, unexplained skull fractures (esp. complex/diastatic), retinal hemorrhages.
- Growing skull fracture (Leptomeningeal cyst): Post-traumatic dural tear with CSF/brain herniation through fracture line.
- Brain: ↑water content, incomplete myelination → greater susceptibility to diffuse injury.
⭐ DAI lesions are classically found at the grey-white matter interface, corpus callosum, and dorsolateral brainstem; MRI is crucial as CT can be normal in up to 50% of cases.
High‑Yield Points - ⚡ Biggest Takeaways
- NCCT Head: Initial modality for acute trauma; identifies fractures, hematomas.
- EDH: Lentiform, arterial (MMA), doesn't cross sutures, lucid interval common.
- SDH: Crescentic, venous (bridging veins), crosses sutures, can be acute or chronic.
- Traumatic SAH: Blood in sulci/cisterns; common, may indicate severe injury.
- DAI: MRI superior for punctate hemorrhages (grey-white junction, corpus callosum, brainstem).
- Signs of raised ICP: Effacement of sulci/cisterns, midline shift, herniation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

