Bacterial Infections - Brain Under Siege
- Pyogenic Abscess:
- Stages:
- Cerebritis (Early/Late): Ill-defined edema, patchy enhancement → central necrosis, developing rim enhancement.
- Capsule (Early/Late): Thin, uniform enhancing rim → thick, collagenous rim; may show daughter loculi.
- Features: Ring enhancement, central DWI restriction, surrounding vasogenic edema.
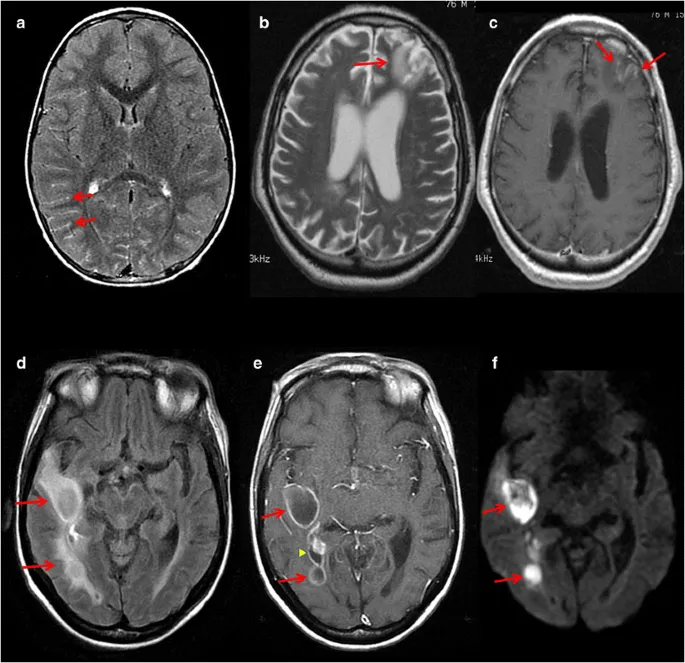
- Stages:
- Empyema:
- Subdural/Epidural collections, often crescentic or lentiform.
- Shows DWI restriction.
- Ventriculitis:
- Ependymal enhancement.
- Intraventricular debris/pus with DWI restriction.
- Meningitis Complications:
- Hydrocephalus.
- Infarcts.
- Cranial nerve enhancement.
⭐ Central diffusion restriction (bright on DWI, dark on ADC) is a hallmark of pyogenic brain abscess, differentiating it from many cystic neoplasms.
Viral Infections - Code Red Viruses
- Herpes Simplex Encephalitis (HSE)
- Type 1: Adults - affects temporal lobes, insula, cingulate gyrus; Neonates - diffuse pattern.
- Imaging: T2/FLAIR hyperintensity, DWI restriction, petechial hemorrhages, gyral enhancement.

⭐ Herpes Simplex Encephalitis (HSE) classically demonstrates bilateral but asymmetric involvement of the medial temporal lobes and limbic system.
- HIV Encephalopathy
- Presents with progressive cognitive decline.
- Imaging: Diffuse, symmetric periventricular/deep white matter T2/FLAIR hyperintensity, cerebral atrophy. Typically no mass effect or enhancement.
- Progressive Multifocal Leukoencephalopathy (PML)
- Caused by JC virus in immunocompromised individuals (e.g., HIV).
- Imaging: Asymmetric, multifocal subcortical and periventricular white matter lesions. Usually no enhancement or mass effect. Posterior fossa involvement is common.
Granulomas & Parasites - The Great Imitators
- Neurotuberculosis (TB):
- Meningitis: Thick basal cisternal enhancement (exudates), communicating hydrocephalus, vasculitic infarcts.
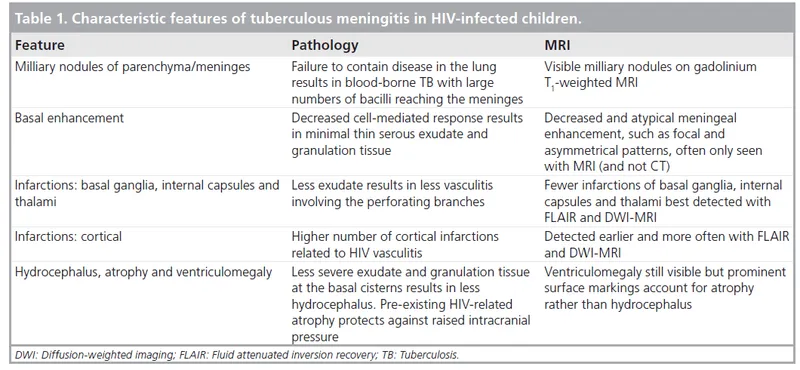

- Tuberculomas: Solitary/multiple ring-enhancing lesions; central caseation (often T2 hypointense, DWI restriction); 'target sign' (central calcification/T2 hypointensity with peripheral rim). Miliary spread possible.
- Meningitis: Thick basal cisternal enhancement (exudates), communicating hydrocephalus, vasculitic infarcts.
- Neurocysticercosis (NCC) - Taenia solium:
- Stages 📌 Mnemonic: "Very Cute Girl Now Calms Down" (Vesicular, Colloidal, Granular, Calcified).
- Locations: Common: parenchyma, subarachnoid space (racemose), ventricles. Intraventricular cysts may cause hydrocephalus.
> ⭐ The presence of an eccentric 'scolex' within a cystic lesion is pathognomonic for the vesicular stage of Neurocysticercosis.
- Toxoplasmosis - Toxoplasma gondii:
- Risk: Immunocompromised (esp. AIDS with CD4 < 100 cells/µL).
- Imaging: Multiple (often <10) ring-enhancing lesions, typically in basal ganglia & corticomedullary junction; surrounding vasogenic edema.
- 'Asymmetric target sign' (eccentric nodule).
- Differentiation: Thallium SPECT: Cold. PET: Hypometabolic (vs. lymphoma: hot/hypermetabolic).
Fungal Infections - Opportunistic Invaders
Primarily affect immunocompromised patients. Key CNS fungal infections include:
- Cryptococcosis (Cryptococcus neoformans)
-
Commonly presents as meningitis.
-
Gelatinous pseudocysts: Basal ganglia/thalami; T2 hyperintense, often non-enhancing.
-
Cryptococcomas: Ring or nodular enhancement.
-
- Aspergillosis (Aspergillus fumigatus)
- Angioinvasive, leading to infarcts and hemorrhage.
- Forms granulomas or abscesses.
- Often from sino-nasal disease extending intracranially.
- Mucormycosis (Rhizopus, Mucor spp.)
- Rhino-orbito-cerebral disease: Affects diabetics (DKA) & immunocompromised.
- Aggressive angioinvasion, thrombosis, infarction, perineural spread.
- Imaging: Lesions often T2 hypointense (iron/manganese).

⭐ Rhino-orbito-cerebral mucormycosis is a life-threatening emergency often seen in patients with diabetic ketoacidosis, characterized by rapid progression and angioinvasion.
High‑Yield Points - ⚡ Biggest Takeaways
- Ring-enhancing lesions: Differentiate pyogenic abscess (DWI restriction), toxoplasmosis (multiple, basal ganglia, eccentric target), tuberculoma (target sign/calcification).
- Neurocysticercosis (NCC): Scolex in cyst is pathognomonic; stages progress from vesicular to calcified.
- HSV encephalitis: Affects temporal lobes and limbic system; often hemorrhagic.
- PML: Subcortical white matter lesions in immunocompromised; no mass effect/enhancement.
- Cryptococcosis: Gelatinous pseudocysts (dilated Virchow-Robin spaces) in basal ganglia; possible leptomeningeal enhancement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

