Spine Anatomy & Modalities - Atlas & The Scanners
- Key Anatomy:
- Vertebral segments: Cervical (7), Thoracic (12), Lumbar (5).
- Atlas (C1): Ring-shaped, no body.
- Axis (C2): Odontoid process (dens).
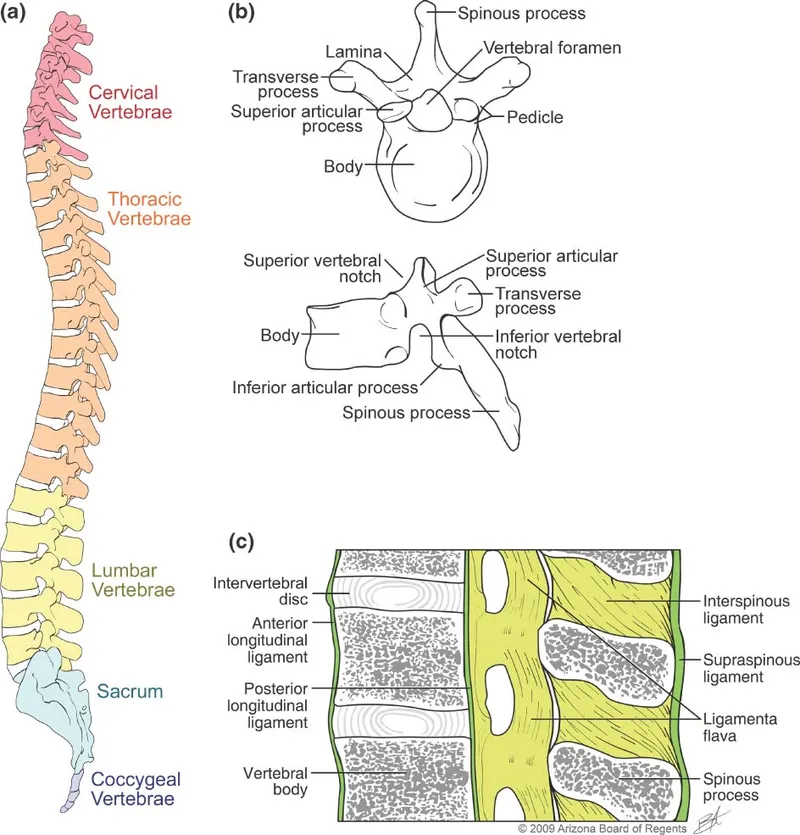
- Imaging Scanners:
- X-ray: First line for trauma, alignment. Views: AP, Lateral, Odontoid.
- CT: Superior for bone detail, complex fractures.
- MRI: Best for spinal cord, discs, nerves, ligaments. Key sequences: T1W, T2W, STIR.
- 📌 T2W: CSF/water is bright (hyperintense).
⭐ Jefferson fracture (C1 burst fracture) results from axial loading; assess transverse ligament integrity using "Rule of Spence" on open-mouth odontoid view.
Spinal Trauma - When Spines Snap
- Initial Imaging: X-ray (trauma series) if CT unavailable. CT is gold standard for bony injury. MRI for cord, ligaments, soft tissues.
- Stability: Denis 3-column theory (Anterior, Middle, Posterior). Instability if ≥2 columns involved.
- Cervical Fractures: Jefferson (C1 burst), Hangman's (C2 bilateral pedicle #), Odontoid (Type II unstable).
- Thoracolumbar Fractures: Compression (anterior column), Burst (all 3 columns, retropulsion), Chance (flexion-distraction, seatbelt injury).
- SCIWORA: Spinal Cord Injury Without Radiographic Abnormality, esp. in children.
⭐ MRI is crucial for detecting ligamentous injury, a key determinant of spinal instability, even with normal CT.
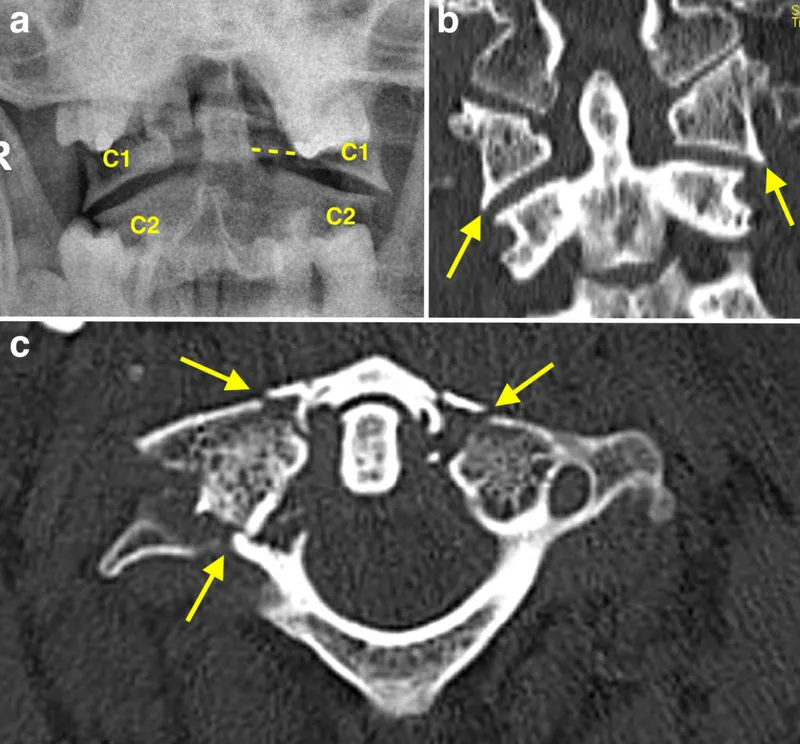
Degenerative Spine Disease - The Ageing Spine's Tale
- Spondylosis: Osteophyte formation, disc space narrowing, endplate sclerosis.
- Disc Degeneration:
- Desiccation (↓T2 signal), height loss, vacuum phenomenon.
- Herniation: bulge, protrusion, extrusion, sequestration.
- Annular fissures/tears.
- Facet Joint Arthropathy: Hypertrophy, osteophytes, joint effusion, subchondral cysts.
- Ligamentum Flavum: Hypertrophy, buckling, ossification.
- Spinal Stenosis:
- Central canal, lateral recess, or foraminal narrowing.
- Degenerative Spondylolisthesis: Anterior vertebral slippage (common at L4-L5).
⭐ Modic changes (vertebral endplate signal alterations): Type I (edema: ↓T1, ↑T2), Type II (fatty marrow: ↑T1, ↑T2), Type III (sclerosis: ↓T1, ↓T2).
Spinal Infections & Inflammation - Fiery Spine Foes
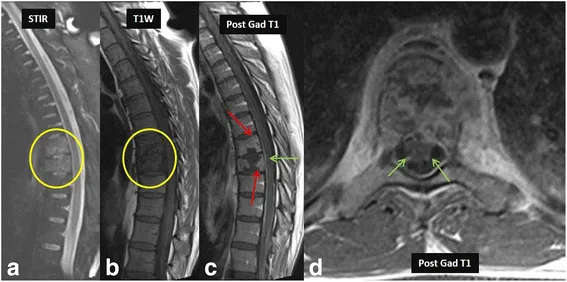
- Pyogenic Spondylodiscitis: S. aureus (MC). Hematogenous. Rapid disc destruction. MRI: T1↓, T2↑ disc/vertebrae, enhancement, abscess.
- Tuberculous Spondylitis (Pott's Spine): Thoracolumbar. Relative disc preservation (early). MRI: Subligamentous spread, large cold abscess, gibbus.
⭐ Pott's spine: Often multiple vertebral bodies, relative disc preservation (early), large cold abscess, subligamentous spread.
- Brucellar Spondylitis: Pedro Pons sign (anterior osteophytes), disc involvement.
- Ankylosing Spondylitis (AS): HLA-B27. Sacroiliitis (earliest sign, bilateral, symmetrical), syndesmophytes, bamboo spine.
 oka
oka
Spinal Tumors & Mimics - Unwanted Spine Guests
- Metastases (Mets): Most common malignant spinal tumors.
- Sources: Lung, breast, prostate, kidney, thyroid (📌 "BLT Kosher Pickle": Breast, Lung, Thyroid, Kidney, Prostate).
- Appearance: Lytic (commonest), blastic (prostate, breast), mixed.
- "Winking owl sign" (pedicle loss). Ivory vertebra (diffuse sclerosis).
- Multiple Myeloma: Punched-out lytic lesions, diffuse osteopenia.
- Primary Tumors:
- Osteoid Osteoma: Nocturnal pain, NSAID relief. Nidus <1.5 cm.
- Chordoma: Sacrococcygeal/clival, T2 hyperintense, locally aggressive.
- Mimics:
- Infection (TB/Pott's): Discitis, vertebral body destruction, paraspinal abscess.
- Degenerative: Modic changes, Schmorl's nodes.
⭐ Vertebral metastases are the most common malignant tumors of the spine, frequently from breast, lung, or prostate primaries.
High‑Yield Points - ⚡ Biggest Takeaways
- MRI: modality of choice for spinal cord, discs, infections, tumors.
- X-rays: initial for trauma, spondylolisthesis, scoliosis. Flexion-extension for instability.
- CT: superior for bony anatomy, complex fractures, osseous stenosis.
- Spondylolysis ("pars defect"): "Scotty dog" sign (X-ray); CT/SPECT confirms.
- T1W MRI: CSF dark, fat bright. T2W MRI: CSF bright, fat bright (unless suppressed).
- STIR sequence: best for bone marrow edema (fractures, osteomyelitis) by nulling fat.
- Vertebral hemangiomas: T1 & T2 hyperintense; "corduroy" or "polka dot" signs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

