Skeletal Infections Overview - Germs Get Going
- Definition: Microbial invasion of bone (osteomyelitis), joints (septic arthritis), or soft tissues.
- Common Culprits:
- Staphylococcus aureus (most common overall).
- Streptococci (neonates, cellulitis).
- Salmonella (sickle cell disease).
- Pseudomonas aeruginosa (IV drug users, puncture wounds).
- Mycobacterium tuberculosis (spinal - Pott's disease).
- Routes of Infection:
- Hematogenous spread (most common in children).
- Direct inoculation (trauma, surgery).
- Contiguous spread (adjacent soft tissue infection).

⭐ Staphylococcus aureus is the most common organism causing acute osteomyelitis across all age groups, except in specific conditions like sickle cell anemia (Salmonella) or IV drug use (Pseudomonas).
Osteomyelitis Imaging - Bone's Battleground
- X-ray (XR): Initial. Soft tissue swelling (early). Periosteal reaction, lytic lesions, sclerosis (10-21 days).
- Chronic: Sequestrum (necrotic bone), involucrum (new bone shell), cloaca (opening).
- MRI: Most sensitive & specific for early diagnosis & extent.
- T1: ↓ signal in marrow.
- T2/STIR: ↑ signal (edema).
- Post-contrast: Enhancing phlegmon/abscess.
- CT: Defines cortical destruction, sequestra, gas.
- 📌 SICK bones: Sequestrum, Involucrum, Cloaca, Know it's chronic!
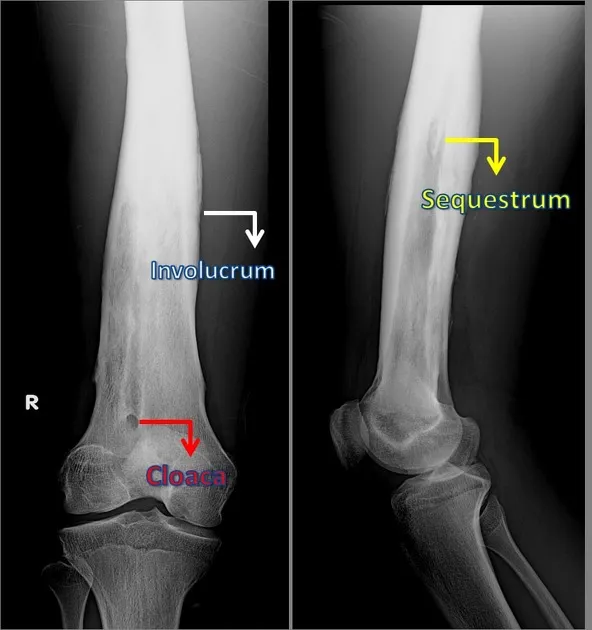
⭐ MRI is the imaging modality of choice for detecting osteomyelitis in its early stages (within 24-48 hrs) and for delineating soft tissue involvement.
Septic Arthritis Imaging - Synovial Showdown
- Early Signs (X-ray may be normal for 7-10 days):
- Soft tissue swelling
- Joint space widening (effusion)
- Later Signs (X-ray):
- Juxta-articular osteoporosis
- Joint space narrowing (cartilage destruction)
- Subchondral bone erosions (marginal or central)
- Periosteal reaction
- Ultrasound (USG):
- Detects joint effusion (earliest sign)
- Guides aspiration
- Synovial thickening, hyperemia (Doppler)
- MRI:
- Most sensitive & specific
- Shows synovial enhancement, marrow edema, abscess
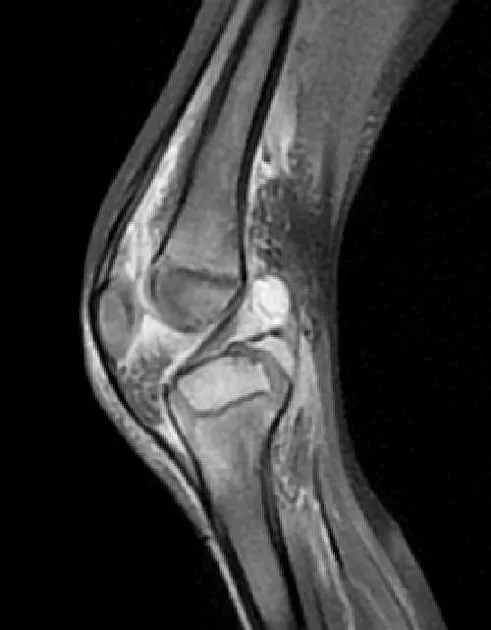
⭐ MRI is the gold standard for early diagnosis and assessing extent, especially for sacroiliitis or sternoclavicular joint involvement. Shows marrow edema, synovial enhancement, and fluid collections effectively.
Spinal Infections - Spinal Sabotage
- Spondylodiscitis: Infection of intervertebral disc (IVD) & adjacent vertebral bodies.
- Pyogenic: Staphylococcus aureus (most common); rapid, destructive.
- Granulomatous: Tuberculosis (Pott's spine); insidious, slow.
- Pott's Spine (TB Spondylitis):
- Thoracic spine most affected.
- Key signs: Paradiscal vertebral destruction, anterior wedging, cold abscess, gibbus deformity.
- Risk: Neurological deficits due to cord compression.

⭐ MRI is the gold standard for early diagnosis, assessing extent (e.g., epidural abscess), and guiding management of spinal infections.
Specific Infections & Mimics - Unique Unrest
- Tuberculosis (Pott's Spine): Thoracolumbar. Anterior vertebral body destruction, paraspinal (cold) abscess, gibbus. Disc spared early. Rice bodies.
- Brucellosis: Spondylodiscitis, sacroiliitis (unilateral common). Pedro Pons' sign (lumbar osteophyte). Disc often preserved.
- Fungal (Maduromycosis): "Dot-in-circle" sign. Chronic, foot.
- Hydatid Disease: Expansile lytic lesions, daughter cysts.
- Mimics: LCH (vertebra plana), SAPHO.

⭐ TB spine: disc typically spared early vs. pyogenic (rapid disc destruction).
High‑Yield Points - ⚡ Biggest Takeaways
- Staph. aureus: most common in pyogenic osteomyelitis.
- X-ray signs (periosteal reaction) in acute osteomyelitis are late (10-14 days).
- MRI: most sensitive for early osteomyelitis detection and extent.
- Brodie's abscess: chronic, localized osteomyelitis; lytic lesion, sclerotic rim.
- Chronic osteomyelitis: characterized by sequestrum, involucrum, cloaca.
- TB spondylitis (Pott's spine): thoracolumbar, vertebral destruction, cold abscess.
- Neonatal osteomyelitis: often epiphyseal, may cause septic arthritis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

