Osteoporosis - Bones Gone Brittle
-
Definition: ↓Bone mass/density, normal mineralization; microarchitectural decay, ↑fracture risk.
-
Types:
- Primary: Postmenopausal (Type I - rapid trabecular loss), Senile (Type II - cortical/trabecular loss).
- Secondary: Corticosteroids (commonest drug cause), endocrine (hyperparathyroidism, Cushing's), immobilization, myeloma, alcohol.
-
Pathophysiology: ↑Osteoclast activity relative to osteoblast activity.
-
Clinical: Asymptomatic until fracture. Sites: Vertebrae (compression), hip, distal radius (Colles').
-
Radiographic Features:
- Osteopenia (radiolucency), cortical thinning.
- Prominent primary, lost secondary trabeculae.
- Vertebrae: "Codfish" (biconcave), wedge, compression fractures.
- Singh Index: Grade < 3 (femoral neck).
-
Diagnosis:
⭐ DEXA (gold standard): T-score ≤ -2.5 SD (osteoporosis). T-score between -1.0 and -2.5 SD (osteopenia).
Rickets & Osteomalacia - Soft Bones Saga
*Defective mineralization of bone (osteomalacia) & growth plate cartilage (rickets).
- Etiology: Vitamin D deficiency (most common) → ↓Ca absorption. Or phosphate deficiency.
- Pathophysiology: ↓Vit D → ↓Serum Ca & ↓Serum P (eventually) → ↑PTH → ↑bone resorption.
- Labs: ↓Serum 25(OH)D, ↓Ca (or normal), ↓P, ↑ALP (marked), ↑PTH.
- Rickets (Children - open physes):
- Clinical: Craniotabes, rachitic rosary, Harrison's sulcus, limb bowing (genu varum/valgum).
- X-ray: Metaphyseal widening, fraying, cupping, splaying. Growth plate widening.
- Osteomalacia (Adults - closed physes):
- Clinical: Bone pain, proximal muscle weakness, fractures.
- X-ray: Osteopenia, indistinct trabeculae, biconcave (codfish) vertebrae.
⭐ Looser zones (pseudofractures) are pathognomonic for osteomalacia: incomplete, transverse radiolucencies perpendicular to cortex (e.g., scapula, ribs, pelvis, proximal femur).
Hyperparathyroidism - Calcium Chaos Crew
- Excess PTH: ↑Serum Ca, ↓Serum P (or normal/↑ in secondary/tertiary), ↑ALP.
- Types:
- Primary: Adenoma (~80%), hyperplasia, carcinoma.
- Secondary: CKD (most common), Vit D deficiency.
- Tertiary: Autonomous PTH after prolonged secondary.
- Mechanism: ↑PTH → ↑Osteoclast activity → ↑Bone resorption.
- 📌 Classic: "Bones, stones, abdominal groans, psychic moans."
- Radiological Features (Osteitis Fibrosa Cystica - OFC):
- Subperiosteal resorption (pathognomonic): Radial aspect of middle phalanges, distal clavicles.
- Brown tumors (lytic lesions; osteoclasts & hemosiderin).
- "Salt & pepper" skull.
- Osteopenia/Osteoporosis.
- Chondrocalcinosis.
⭐ Subperiosteal bone resorption on the radial aspect of the 2nd and 3rd middle phalanges is a hallmark of hyperparathyroidism.
Paget's Disease - Mixed-Up Remodeling
- Chronic disorder: excessive bone resorption, disorganized ↑ new bone.
- Phases:
- Lytic (osteoclasts ↑): "blade of grass/flame sign" (long bones); osteoporosis circumscripta (skull).
- Mixed: lytic + blastic activity.
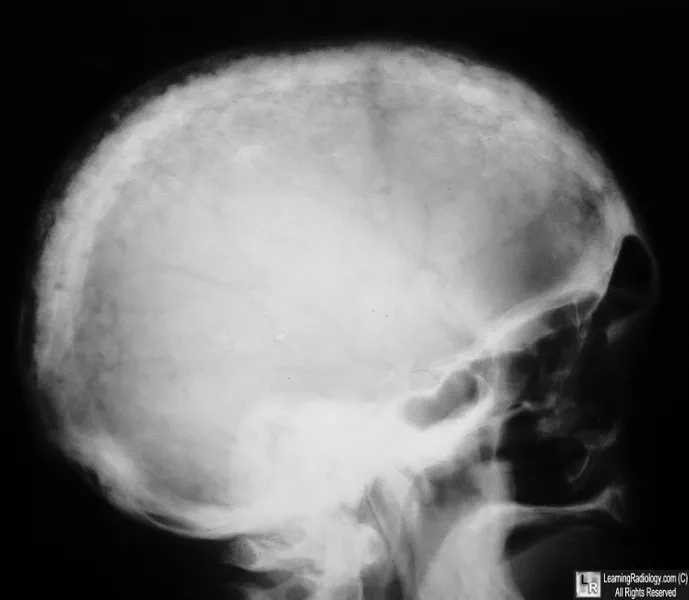
- Sclerotic (osteoblasts ↑): thickened cortices/trabeculae; "cotton wool" skull.
- Clinical: Often asymptomatic. Bone pain, deformity (bowing), fractures.
- Labs: ↑ ALP; normal Ca, PO4. ↑ Urine hydroxyproline.
- Imaging:
- Pelvis: iliopectineal line thickening (brim sign), protrusio acetabuli.
- Spine: "picture frame/ivory" vertebra.
- Long bones: cortical thickening, bowing, fissure (banana) fractures.
- Complications: Pathological fractures, deafness, nerve compression, high-output CHF, osteosarcoma (<1%).
⭐ Most common site for Paget's sarcoma is the femur, followed by pelvis and humerus (in decreasing order of frequency).
High‑Yield Points - ⚡ Biggest Takeaways
- Osteoporosis: DEXA T-score ≤ -2.5; commonest cause of vertebral compression fractures.
- Rickets/Osteomalacia: Vitamin D deficiency leads to Looser's zones (pseudofractures) and cupped/frayed metaphyses in children.
- Primary Hyperparathyroidism: Subperiosteal resorption (pathognomonic), brown tumors, salt-and-pepper skull, osteitis fibrosa cystica.
- Paget's Disease: Presents with lytic and sclerotic phases, cotton wool skull, and blade of grass sign.
- Scurvy: Vitamin C deficiency causes subperiosteal hemorrhages and Wimberger's ring sign.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

