Introduction - See & Treat Magic
- Theranostics: A paradigm combining diagnostics (Dx) and therapy (Tx) using a single agent or platform.
- Core Principle: "See what you treat, treat what you see."
- Diagnostic component visualizes the target (e.g., tumor, receptor).
- Therapeutic component delivers treatment to the visualized target.
- Mechanism: Utilizes molecules that can be labeled with either an imaging isotope (for Dx) or a therapeutic isotope/drug (for Tx).
- Often involves a targeting moiety (e.g., peptide, antibody) linked to a radionuclide.

- Goal: Personalized medicine - precise localization and targeted treatment, minimizing systemic toxicity.
⭐ Theranostics embodies the 'magic bullet' concept envisioned by Paul Ehrlich, aiming for highly specific drug delivery to diseased cells.
- Key advantage: Allows for patient selection, treatment planning, and monitoring response effectively.
Radiopharmaceutical Pairs - Dynamic Duos
Theranostics employs 'dynamic duos': a diagnostic radiopharmaceutical to visualize a target, and a therapeutic counterpart to treat it. Both agents bind to the same molecular entity. These pairs enable personalized medicine by confirming target presence before therapy.
📌 Iodine ($^{123}I$/$^{131}I$): Imaging and Internal radiotherapy for thyroid.
| Diagnostic Partner | Therapeutic Partner | Molecular Target | Primary Clinical Use(s) |
|---|---|---|---|
| $^{68}Ga$-DOTATATE/-NOC/-TOC | $^{177}Lu$-DOTATATE, $^{90}Y$-DOTATOC | SSTR | Neuroendocrine Tumors (NETs) |
| $^{68}Ga$-PSMA-11/-I&T | $^{177}Lu$-PSMA-617, $^{225}Ac$-PSMA | PSMA | Prostate Cancer |
| $^{123}I$ or $^{131}I$ (low dose) | $^{131}I$ (high dose) | NIS (Sodium-Iodide Symporter) | Differentiated Thyroid Cancer (DTC) |
| $^{99m}Tc$-MDP/HMDP | $^{153}Sm$-EDTMP, $^{223}RaCl_2$ | Hydroxyapatite (Bone) | Painful Bone Metastases |
| $^{111}In$-Pentetreotide | $^{90}Y$-DOTATOC, $^{177}Lu$-DOTATATE | SSTR | NETs (SPECT option/therapy) |
Key Clinical Uses - Cancer Combat Zones
-
Prostate Cancer (PCa):
- Target: Prostate-Specific Membrane Antigen (PSMA).
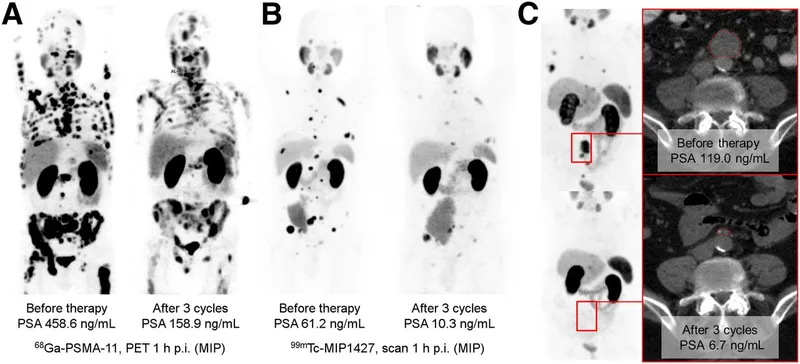
- Diagnostic: $^{68}Ga$-PSMA PET/CT (staging, recurrence).
- Therapeutic: $^{177}Lu$-PSMA (metastatic Castration-Resistant PCa, mCRPC).
- Threshold: High PSMA expression on PET.
⭐ $^{177}Lu$-PSMA therapy shows significant survival benefits in mCRPC patients post prior therapy failure.
-
Neuroendocrine Tumors (NETs):
- Target: Somatostatin Receptors (SSTRs).
- Diagnostic: $^{68}Ga$-DOTATATE/TOC PET/CT.
- Therapeutic: Peptide Receptor Radionuclide Therapy (PRRT) with $^{177}Lu$-DOTATATE / $^{90}Y$-DOTATATE.
- 📌 Mnemonic: 'DOTATATE targets SSTRs - Don't Hesitate, Radiate!'
- Key: High SSTR expression; Ki-67 < 20% often preferred for PRRT.
-
Differentiated Thyroid Cancer (DTC):
- Target: Sodium-Iodide Symporter (NIS).
- Diagnostic: $^{123}I$ or low-dose $^{131}I$ Whole Body Scan (WBS).
- Therapeutic: High-dose $^{131}I$ (remnant ablation, metastatic disease).
-
Flowchart: PSMA Therapy Selection for mCRPC
Dosimetry & Future - Scan, Plan, Advance!
- Dosimetry:
- Calculates absorbed radiation dose (Gy) for personalized theranostics.
- Utilizes imaging (SPECT/CT, PET/CT) & MIRD schema.
- Optimizes tumor dose vs. normal tissue toxicity.
- Future Horizons:
- Alpha-emitters ($^{225}Ac$, $^{213}Bi$): High LET, short-range for potent, localized kill.
- New radiopharmaceuticals & targets.
- AI in planning & response prediction.
- Combination therapies (e.g., immunotherapy).
⭐ Alpha-emitters like $^{225}Ac$ are highly promising due to their high Linear Energy Transfer (LET) and short path length, delivering potent, localized cytotoxicity with minimal damage to surrounding healthy tissue.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Theranostics uniquely combines diagnostic imaging and targeted radionuclide therapy.
- Core concept: "See what you treat, treat what you see", enabling personalized treatment.
- Lu-177 DOTATATE is pivotal for imaging and treating neuroendocrine tumors (NETs).
- Lu-177 PSMA targets prostate-specific membrane antigen (PSMA) in advanced prostate cancer.
- I-131 remains a cornerstone for both diagnosis and therapy of thyroid disorders.
- Radium-223 (Xofigo), an alpha-emitter, is used for bone metastases in prostate cancer.
- Enables patient-specific treatment selection and monitoring of therapeutic response.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

