Vascular Access Techniques: Prep & Prudence - Ground Zero
- Indications: Diagnostic (angiography), Therapeutic (embolization, stenting).
- Contraindications:
- Absolute: Active infection at site, severe uncorrectable coagulopathy.
- Relative: Moderate coagulopathy, patient refusal.
- Pre-procedural Workup:
- History: Allergies, renal function, anticoagulants/antiplatelets.
- Exam: Pulses, Allen's test (radial).
- Labs: CBC, PT/INR (< 1.5-1.8), aPTT, Creatinine, Platelets (> 50,000/μL).
- Informed Consent: 📌 PRBA (Procedure, Risks, Benefits, Alternatives).
⭐ Allen's test is crucial before radial artery cannulation to ensure ulnar artery collateral circulation.
Vascular Access Techniques: Site Seeing - Entry Points
Arterial Access:
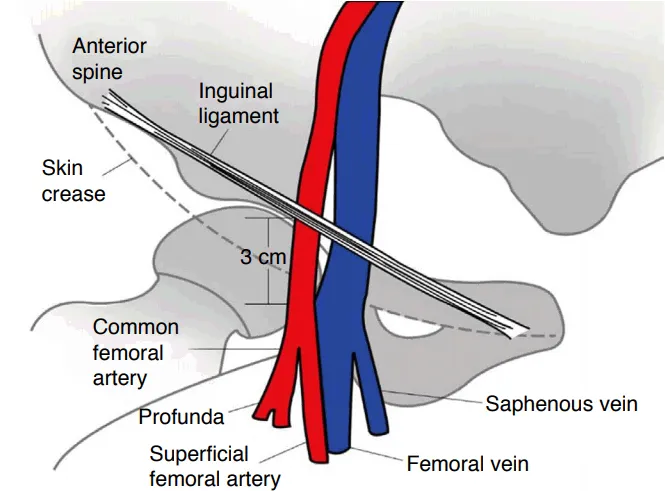
- Common Femoral Artery (CFA): Most common. Landmark: Inguinal ligament, femoral pulse. 📌 NAVEL (Lateral to Medial: Nerve, Artery, Vein, Empty space, Lymphatics).
- Pros: Large vessel, easy access.
- Cons: Retroperitoneal bleed risk, infection.
- Radial Artery (RA): ↑Patient comfort, ↓complications. Landmark: Styloid process of radius, radial pulse.
- Pros: ↓Bleeding, early ambulation.
- Cons: Smaller vessel, spasm risk.
- Brachial Artery (BA): Landmark: Medial to biceps tendon, brachial pulse.
- Pros: Alternative if CFA/RA unsuitable.
- Cons: ↑Nerve injury risk (median nerve).
Venous Access:
- Internal Jugular Vein (IJV): Preferred for central lines. Landmark: Triangle b/w sternal & clavicular heads of Sternocleidomastoid (SCM) muscle, carotid pulse (medial).
- Pros: ↓DVT/pneumothorax vs subclavian.
- Cons: Carotid puncture risk.
- Femoral Vein (FV): Medial to CFA. Landmark: Inguinal ligament, femoral pulse.
- Pros: Easy access in emergencies.
- Cons: ↑DVT risk, infection.
- Subclavian Vein (SCV): Landmark: Junction of medial 1/3 & lateral 2/3 of clavicle.
- Pros: Patient comfort.
- Cons: ↑Pneumothorax/hemothorax risk.
- Peripheral Arm Veins: (Basilic, Cephalic) For PICCs.

⭐ The Seldinger technique is the cornerstone of percutaneous vascular access, involving needle puncture, guidewire insertion, sheath placement over wire, and finally catheter introduction through sheath.
Vascular Access Techniques: Needle Ninjutsu - Technique Toolkit
- Seldinger Technique: Core method for vascular access.
- Modified Seldinger (Micropuncture):
- Initial access with smaller 21G needle & 0.018" wire.
- System then upsized if needed.
- Benefits: Reduced vessel trauma, safer for challenging or small vessels.
- Ultrasound Guidance: Real-time needle and vessel visualization.
- Views: Transverse (short-axis/out-of-plane) vs. Longitudinal (long-axis/in-plane).
- Advantages: ↑ first-pass success, ↓ attempts, ↓ mechanical complications (e.g., hematoma, pneumothorax).
- Fluoroscopic Guidance: X-ray imaging confirms final wire/catheter position, often using bony landmarks.
- Aseptic Technique: Critical. Includes sterile field, skin prep (chlorhexidine preferred), sterile attire, draping.

⭐ The most common site for iatrogenic arterial injury during central line placement is the carotid artery when attempting internal jugular vein access on the same side.
Vascular Access Techniques: Gizmos & Gadgets - The IR Arsenal
- Needles:
- Types: Bevelled (sharp for initial puncture), trocar-tipped (blunt dissection).
- Sizes: 18G (standard Seldinger), 21G (micropuncture).
- Guidewires:
- Diameters: 0.018" (micropuncture), 0.035" (standard workhorse).
- Tips: J-tip (atraumatic navigation), angled, straight. Stiffness: floppy to stiff.
- Coatings: Hydrophilic (↓friction), heparin (↓thrombogenicity).
- Catheters: $Fr = \text{Outer Diameter (mm)} \times 3$.
- Types: Diagnostic (e.g., pigtail, vertebral) vs. Guiding (support).
- Material: Polyurethane, nylon, polyethylene.
- Sheaths: Introducer with hemostatic valve & side port (flushing/infusion).
⭐ The 0.035" guidewire is the most versatile and commonly used size for a wide range of general angiography and interventions. 📌 Nice Green Cars Shine (Needles, Guidewires, Catheters, Sheaths).
oka
Vascular Access Techniques: Code Red - Oops & Outcomes
- Access Site Complications:
Complication Key Sign(s) Mgmt Hint Hematoma Swelling, pain (most common) Compression Pseudoaneurysm Pulsatile mass, to-and-fro Doppler US-Thrombin Inj. AV Fistula Thrill/bruit, continuous Doppler Repair Dissection Intimal flap, ↓flow Stent/Surgery Thrombosis ↓flow, ischemia Anticoagulation - Systemic/Other: Contrast reaction, air embolism, infection, nerve injury (brachial/femoral).
- ⚠️ Retroperitoneal hemorrhage: High femoral access (above inguinal lig.).
- 📌 PAIN: Pseudoaneurysm, AV fistula, Infection, Nerve injury.
- VCDs (Vascular Closure Devices): Active/Passive. Risks: failure, infection, stenosis.
⭐ Femoral puncture above the inguinal ligament (i.e., above inferior epigastric artery origin) significantly ↑ risk of retroperitoneal hemorrhage.
High‑Yield Points - ⚡ Biggest Takeaways
- Seldinger technique is fundamental for percutaneous vascular access.
- Common femoral artery: most common arterial access; Allen's test for radial artery patency.
- Ultrasound guidance is standard for central venous access; improves safety for arterial access.
- Micropuncture kits (e.g., 21G needle) reduce access site complications.
- Key complications: hematoma, pseudoaneurysm, AV fistula, infection, retroperitoneal bleed.
- Catheter sizes in French (Fr) (1 Fr = 0.33 mm); guidewires in inches.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

