Ablation Fundamentals - Zap & Control
- Goal: Localized tumor destruction via chemical or thermal energy.
- Intent: Curative, palliative, or bridge to transplant.
- Mechanisms:
- Thermal: Heat (RFA, MWA, Laser, HIFU); Cold (Cryoablation).
- Chemical: Ethanol, Acetic Acid.
- Non-thermal: Irreversible Electroporation (IRE).
- Key Factors: Tumor size/location, proximity to vital structures.
- Ablation Zone: Tumor + 0.5-1 cm safety margin.
- Guidance: Ultrasound (US), CT, MRI.

⭐ Ablation is a key treatment for non-surgical candidates with early-stage HCC (e.g., BCLC Stage 0/A).
Thermal Ablation - Heat vs. Cold
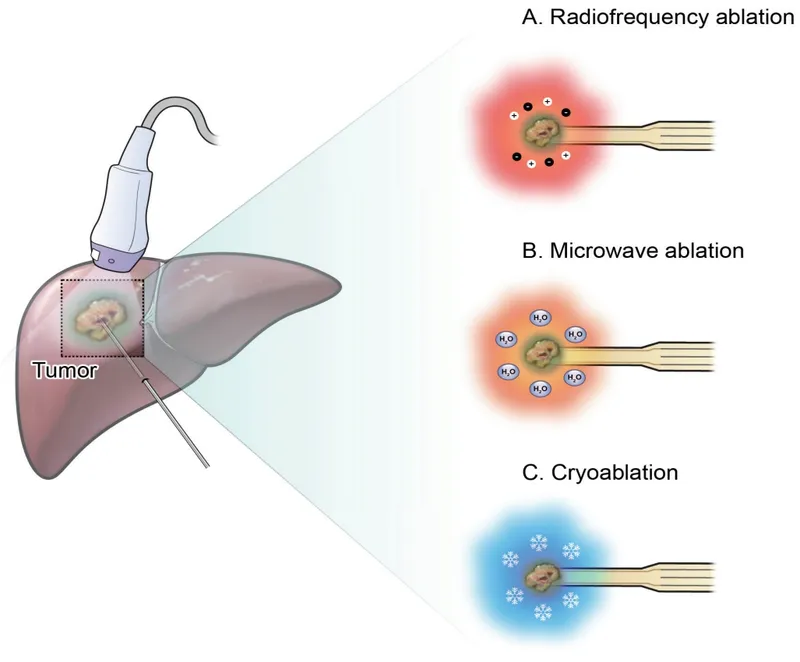
Thermal ablation uses extreme temperatures for tumor destruction. Heat-based: RFA, MWA. Cold-based: Cryoablation.
- Mechanisms:
- RFA: Frictional heat ($\textbf{60-100}$°C).
- MWA: Dielectric heat ($> \textbf{100}$°C).
⭐ MWA is less susceptible to 'heat sink' effect vs RFA; better for perivascular tumors.
- Cryoablation: Joule-Thomson effect, ice ball ($< \textbf{-40}$°C).

Comparative Overview:
| Feature | RFA | MWA | Cryoablation |
|---|---|---|---|
| Principle | Frictional heat | Dielectric heat (volumetric) | Joule-Thomson (ice ball) |
| Target Temp. | $\textbf{60-100}$°C | $> \textbf{100}$°C | $< \textbf{-40}$°C |
| Heat Sink | High susceptibility | Low susceptibility | N/A (cold effect) |
| Ablation Zone | Slower, smaller | Faster, larger | Visible ice ball, well-defined |
| Advantages | Cost-effective, established | Rapid, ↓ heat sink, larger zones | Real-time visible, analgesic, spares collagen |
| Disadvantages | Heat sink effect, charring, pain | Higher cost, larger unpredictable zones | Longer procedure, cryoshock (rare), hemorrhage |
Non-Thermal & Chemical - Shock & Dissolve
- Irreversible Electroporation (IRE)
- Mechanism: High-voltage, short electrical pulses create nanopores in cell membranes → apoptosis.
- Non-thermal; spares extracellular matrix, vessels, ducts.
⭐ Irreversible Electroporation (IRE) is a non-thermal technique that preserves surrounding connective tissue matrix, making it suitable near delicate structures like bile ducts or major vessels.
- Chemical Ablation
- Agents: Ethanol (95-100%), Acetic Acid.
- Mechanism: Cellular dehydration, protein denaturation, tumor necrosis.
- Used for: Hepatocellular carcinoma (HCC), thyroid cysts, venous malformations.
 and Chemical Ablation techniques in tumor treatment)
and Chemical Ablation techniques in tumor treatment)
Procedural Blueprint - Plan, Guide, Follow
- Plan:
- Pre-procedural imaging (CT/MRI/US): tumor characterization, localization, access planning.
- Select ablation modality (e.g., RFA, MWA), anesthesia.
- Guide:
- Imaging Guidance:
- US: Real-time, no radiation, portable.
- CT: Excellent spatial resolution, deep lesions.
- MRI: Superior soft tissue contrast, no radiation.
- Accurate probe placement is critical.
- Imaging Guidance:
- Follow:
- Post-ablation imaging: Contrast CT/MRI at 1 month, then 3-6 monthly.
- Assess treatment response; monitor complications.
⭐ Post-ablation success is typically defined by complete lack of enhancement in the treated zone on contrast-enhanced CT/MRI at 1-month follow-up.
Ablation Aftermath - Risks & Fixes
- Common:
- Pain: Analgesics.
- Bleeding: Monitor; embolization if severe.
- Infection/Abscess: Antibiotics, drainage.
- Specific Risks:
- Pneumothorax (lung/liver): Chest tube.
- Non-target injury (nerve, bowel): Supportive/surgical.
- Skin burns (RF/MW): Prevention crucial.
- Tract seeding (rare): Tract ablation.
⭐ Post-ablation syndrome (fever, malaise, myalgia, leukocytosis) is a common, self-limiting systemic inflammatory response, not necessarily infection.
High‑Yield Points - ⚡ Biggest Takeaways
- Radiofrequency Ablation (RFA): Most common thermal ablation for small tumors (<3 cm), e.g., HCC.
- Microwave Ablation (MWA): Larger ablation zones, less heat sink effect, good near vessels.
- Cryoablation: Freezes tumors ("ice ball"), good for pain palliation (bone mets), renal tumors.
- Irreversible Electroporation (IRE): Non-thermal, spares vessels/ducts, used for pancreatic/hilar tumors.
- Ethanol (PEI): Chemical ablation for cystic lesions, small HCCs.
- Image guidance (US/CT) is crucial for precise targeting and safety.
- Key risks: Pain, bleeding, non-target ablation, post-ablation syndrome.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

