TIPS Basics - Shuntastic Voyage
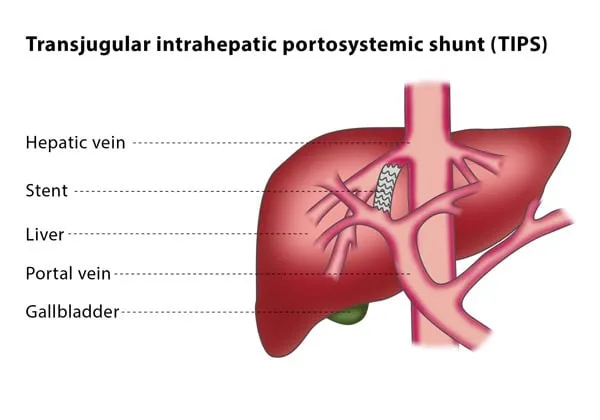
- Definition: A radiologically created shunt connecting the portal vein (PV) to a hepatic vein (HV) through the liver parenchyma.
- Access: Typically via the right internal jugular vein.
- Mechanism: A stent-graft is placed, creating a low-resistance pathway for portal blood to bypass the cirrhotic liver, directly entering systemic circulation.
- Goal: ↓ Portal pressure, alleviating complications of portal hypertension.
- Key Effect: Reduces portosystemic gradient (PSG).
⭐ Successful TIPS typically reduces the portosystemic gradient (PSG) to below 12 mmHg or by at least 50% from baseline to effectively manage variceal bleeding risk and refractory ascites.
The TIPS Procedure - Navigating the Liver
- Access Route: Right Internal Jugular Vein (Rt. IJV) preferred → Superior Vena Cava (SVC) → Right Atrium (RA) → Inferior Vena Cava (IVC) → Hepatic Vein (HV), typically Right HV.
- Guidance & Initial Steps: Fluoroscopy (primary); Ultrasound (IJV access). Wedged hepatic venography & portography (visualize Portal Vein).
- Parenchymal Puncture: From HV, advance needle (e.g., Colapinto) anteriorly/medially into intrahepatic Portal Vein (PV) branch. Confirm PV access.
- Shunt Creation & Stenting: Guidewire into PV (e.g., Superior Mesenteric Vein/Splenic Vein). Dilate tract (8-10 mm balloon). Deploy covered stent-graft (PTFE) from PV to HV.
- Hemodynamic Goal: Target Portosystemic Gradient (PSG) < 12 mmHg or ≥50% reduction from baseline.
⭐ Covered stents (e.g., Viatorr) significantly improve primary patency by reducing bile duct injury and intimal hyperplasia compared to bare metal stents.
TIPS Hurdles - Shunt Shenanigans
Contraindications (CI): ⚠️
- Absolute:
- CHF, severe pulm HTN (mPAP > 45 mmHg)
- Severe tricuspid regurgitation
- Polycystic liver disease (extensive)
- Uncontrolled sepsis/infection
- Unrelieved biliary obstruction
- Relative:
- Active HCC
- Severe coagulopathy (INR > 5, Plt < 20k), uncorrectable
- Central tumors obstructing IVC/hepatic veins
Complications:
- Early (< 30 days):
- HE (most common, ~30-50%)
- Hemorrhage (capsular/intraperitoneal), neck hematoma
- Stent issues: malposition, migration, infection, thrombosis
- Acute liver failure, hemolysis
- Late (> 30 days):
- Shunt stenosis/occlusion (common late)
- Worsening/refractory HE
- Progressive liver failure
Shunt Dysfunction:
- Causes:
- Neointimal hyperplasia (commonest for stenosis)
- Thrombosis (acute/chronic)
- Stent migration or kinking
- Sx: Recurrent ascites, variceal bleed
- Dx: Doppler US (flow changes), portography
⭐ > New or worsening hepatic encephalopathy: most common post-TIPS complication, affects up to 50%.

TIPS Check-up - Shunt Surveillance
- Goal: Maintain shunt patency & prevent complications (e.g., hepatic encephalopathy, shunt stenosis/occlusion).
- Initial Check: Doppler Ultrasound (DUS) within 24-72 hours post-TIPS.
- Routine Surveillance (DUS):
- At 1, 3, 6 months post-procedure.
- Then every 6-12 months lifelong.
- Key Parameters Assessed:
- Shunt patency and morphology.
- Peak Shunt Velocity (PSV): Normal range 90-190 cm/s.
- Signs of Dysfunction on DUS:
- PSV < 90 cm/s or > 190 cm/s.
- Significant PSV change from baseline (e.g., ↑ > 50% or ↓ > 40%).
- Focal velocity ↑ (stenosis); no flow (occlusion).
- Clinical: Recurrence of ascites or variceal bleeding.
⭐ Doppler ultrasound is the primary non-invasive modality for routine TIPS surveillance, assessing flow velocities and identifying stenosis or occlusion.
- Management of Dysfunction: Confirm with portography/venography & pressure measurements; consider angioplasty, re-stenting, or parallel TIPS if indicated.
High‑Yield Points - ⚡ Biggest Takeaways
- TIPS: Shunt between hepatic vein (e.g., RHV) and portal vein (e.g., RPV) via stent.
- Primary indications: Refractory variceal hemorrhage and refractory ascites.
- Most common significant complication: New or worsening hepatic encephalopathy.
- Key contraindications: Severe heart failure (NYHA III/IV), severe pulmonary hypertension, uncontrolled systemic infection.
- Doppler ultrasound is primary for monitoring shunt patency.
- Therapeutic goal: ↓ Portosystemic gradient (PSG) to <12 mmHg or by >50%.
- Covered stents preferred over bare stents for ↑ long-term patency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


