GI Bleed & Portal Hypertension - Stop Leaks, Ease Pressure
GI Bleeding (Non-Variceal):
- Diagnosis: CTA first, then DSA (Digital Subtraction Angiography) for active bleed localization.
- Intervention: Trans-arterial Embolization (TAE).
- Indications: Failed endoscopy, high-risk stigmata (e.g., active spurting).
- Agents: Coils, Gelfoam, PVA particles, N-butyl cyanoacrylate (NBCA).
- Complications: Bowel ischemia, non-target embolization, rebleed, access site issues.
- Image:

Portal Hypertension & TIPS:
- TIPS (Transjugular Intrahepatic Portosystemic Shunt): Creates shunt (hepatic vein to portal vein).
- Goal: Reduce portal pressure; target Portosystemic Gradient ($PSG = PVP - IVCP$) <12 mmHg.
- Indications: Refractory variceal bleed, refractory ascites/hepatic hydrothorax.
- Contraindications (Absolute): Severe heart failure (↑RAP), uncontrolled hepatic encephalopathy (Grade III-IV), active systemic infection, severe pulmonary HTN (>45 mmHg mPAP).
- Complications: Hepatic encephalopathy (most common, ~30%), shunt stenosis/occlusion, heart failure. 📌 Mnemonic: SHENT (Stenosis, Heart failure, Encephalopathy, New liver failure, Thrombosis).
- Image:
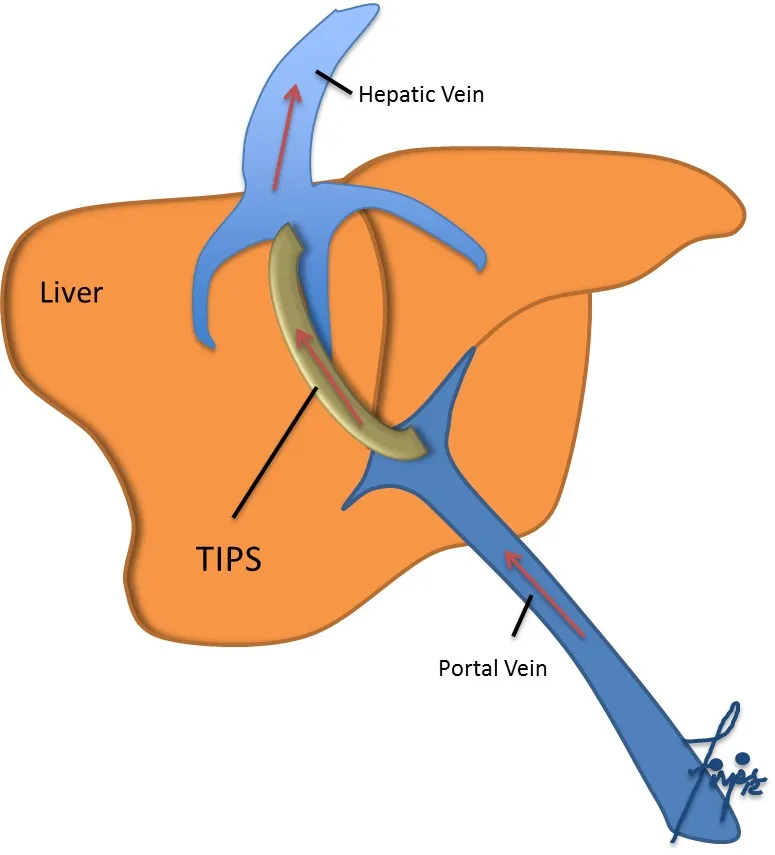
⭐ > BRTO (Balloon-occluded Retrograde Transvenous Obliteration) is preferred for gastric varices with a gastrorenal shunt, while TIPS is for diffuse portal hypertension.
Biliary & Enteric Interventions - Unblock Pathways, Restore Flow
Percutaneous Transhepatic Biliary Drainage (PTBD):
- Indications: Obstructive jaundice (e.g., bilirubin >5-10 mg/dL), acute cholangitis, biliary leaks/fistulas, pre-operative decompression.
- Technique: Ultrasound/fluoroscopy-guided transhepatic puncture of bile duct, catheter placement.
- Drainage Options:
- External drainage catheter.
- Internal-external drainage catheter.
- Internal stent (plastic or metallic).
Biliary Stent Comparison:
| Feature | Plastic Stents | Metallic Stents (SEMS) |
|---|---|---|
| Material | Polyethylene, Teflon | Nitinol, Stainless steel |
| Diameter | Smaller (e.g., 7-12 Fr) | Larger (e.g., 8-10 mm lumen) |
| Patency | Shorter (3-6 months) | Longer (6-12+ months) |
| Indication | Benign strictures, short-term use | Malignant strictures, longer-term |
| Cost | Lower | Higher |
| Removability | Easily removable/exchangeable | Covered SEMS: Yes; Uncovered: No |
GI Tract Stenting (Esophageal, Duodenal, Colonic):
- Indications: Palliation of malignant obstruction (dysphagia, gastric outlet obstruction, colonic obstruction); selected benign strictures.
- Types: Self-Expanding Metallic Stents (SEMS) - covered (prevents tumor ingrowth, allows removal) or uncovered (better anchoring, embeds into wall).
- Complications: Migration, occlusion (tumor, food), perforation, bleeding, pain.
Percutaneous Gastrostomy (PG) / Jejunostomy (PJ):
- Indications: Long-term enteral feeding (>4-6 weeks), gastric decompression.
- Techniques: Ultrasound/fluoroscopy-guided puncture; Seldinger or "push/pull" methods.
- Contraindications: Uncorrectable coagulopathy, massive ascites, overlying bowel, active gastric/jejunal disease at site.

Flowchart: Malignant Biliary Obstruction Management
GI Tumors & Abscesses - Target & Drain Precisely
-
Transarterial Therapies (HCC/Liver Mets):
- TACE (Transarterial Chemoembolization): Uses chemotherapy (e.g., Doxorubicin, Cisplatin) + embolic agents for unresectable Hepatocellular Carcinoma (HCC) or liver metastases. Primarily palliative or bridging to transplant.
- TARE/SIRT (Transarterial Radioembolization): Uses Y-90 microspheres for internal radiation. For HCC/mets; can be used for downstaging or in patients with portal vein thrombosis (PVT).
⭐ TARE (Y-90) delivers radiation directly to the tumor, often better tolerated than TACE in patients with borderline liver function or portal vein thrombosis.
Feature TACE TARE/SIRT Agent Chemo (Doxorubicin) + Embolic Y-90 (Radiation) Primary Goal Cytotoxicity + Ischemia Localized Radiotherapy Child-Pugh Best: A/B; Contra: C Tolerates borderline function better PVT Relative contraindication Often feasible Tumor Burden Limit Avoid if >50-70% liver involvement Can treat higher burden if segmental -
Tumor Ablation (RFA/MWA): For unresectable liver, kidney, lung tumors in non-surgical candidates.
- RFA (Radiofrequency Ablation): Best for tumors <3 cm.
- MWA (Microwave Ablation): For larger tumors (up to 5-6 cm), faster ablation, less heat-sink effect near vessels.
-
Percutaneous Abscess Drainage:
- Indications: Intra-abdominal/pelvic abscesses, symptomatic collections.
- Guidance: Ultrasound (US) or CT. Catheters placed using Seldinger/Trocar techniques.
- Success Rate: Typically >80-90%.

High‑Yield Points - ⚡ Biggest Takeaways
- TIPS creation is vital for refractory variceal bleeding/ascites; hepatic encephalopathy is a key risk.
- PTBD drains obstructed biliary systems if ERCP fails; watch for sepsis, bleeding.
- Angioembolization is crucial for acute arterial GI bleeds unresponsive to endoscopic control.
- Thermal ablation (RFA/MWA) effectively treats small primary/metastatic liver tumors.
- TACE/TARE (SIRT) are standard palliative options for unresectable HCC.
- Esophageal stenting relieves dysphagia from malignant esophageal strictures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

