Embolization: Core Concepts - Sealing the Pipes
- Definition: Therapeutic, catheter-guided endovascular occlusion of blood vessels.
- Primary Aims:
- Control/prevent hemorrhage (e.g., GI bleed, trauma, postpartum, epistaxis).
- Devascularize tumors (e.g., HCC, RCC, fibroids) or abnormal tissue (e.g., AVMs, AVFs).
- Reduce blood flow pre-operatively or for palliation.
- Mechanism: Precise, angiographically-guided delivery of embolic agents to target sites.
- Desired Physiological Effect: Achieve stasis, ↓ blood flow, leading to target ischemia, necrosis, or thrombosis, while sparing non-target tissues.
- Access Routes: Primarily femoral artery; alternatives include radial, brachial arteries, or venous access.
⭐ Uterine Artery Embolization (UAE) is a key minimally invasive option for symptomatic uterine fibroids, offering uterine preservation and symptom relief.
Embolic Materials - Blocker's Arsenal
- Temporary (Absorbable):
- Gelfoam (Gelatin Sponge):
- Mechanism: Mechanical block, promotes thrombosis.
- Resorption: Weeks to months.
- Forms: Pledgets, powder, slurry.
- Autologous Blood Clot:
- Mechanism: Physiological thrombosis.
- Resorption: Variable, often rapid lysis.
- Gelfoam (Gelatin Sponge):
- Permanent (Non-Absorbable):
- Particulate Agents:
- Polyvinyl Alcohol (PVA): Irregular particles (100-1200 µm). Mechanical occlusion.
- Microspheres (e.g., Embospheres): Spherical, calibrated sizes. Predictable occlusion level.
- Mechanical Devices:
- Coils (Platinum, Steel): Fibered or bare. Induce thrombosis, mechanical block.
- Vascular Plugs (e.g., Amplatzer): Nitinol mesh. For larger vessels, precise.
- Liquid Embolics:
- N-Butyl Cyanoacrylate (NBCA/"Glue"): Rapid polymerization with ions. Mixed with Lipiodol.
- Onyx (EVOH - Ethylene Vinyl Alcohol Copolymer): Non-adhesive, lava-like. DMSO solvent. Precipitates with blood/saline.
- Ethanol (Absolute): Sclerosant, protein denaturation. ⚠️ High risk of non-target effects.
- Particulate Agents:
⭐ For effective vessel occlusion, coils should be 20-30% larger in diameter than the target vessel to ensure stable placement and prevent migration.
Clinical Embolization - Plugging Problems
- Hemorrhage Control (Life-saving):
- Acute GI Bleeding (e.g., peptic ulcer, diverticular)
- Traumatic: Solid organ (spleen, liver, kidney), pelvic fractures
- Postpartum Hemorrhage (PPH): Uterine artery embolization
- Bronchial Artery Embolization (BAE) for massive hemoptysis
- Tumor Management (Palliative/Adjunctive):
- Hepatocellular Carcinoma (HCC): TACE (drug-eluting beads), TARE (Y-90)
- Renal Cell Carcinoma (RCC), Uterine Fibroids (UFE)
- Pre-operative devascularization of hypervascular tumors (e.g., meningiomas, JNA)
- Vascular Anomalies & Conditions:
- Arteriovenous Malformations (AVMs), Venous Malformations (sclerotherapy)
- Varicocele (gonadal vein), Pelvic Congestion Syndrome (ovarian vein)
- Pulmonary AVMs in Hereditary Hemorrhagic Telangiectasia (HHT)
- Splenic Artery Embolization: For hypersplenism, portal hypertension (e.g., partial splenic embolization - PSE).
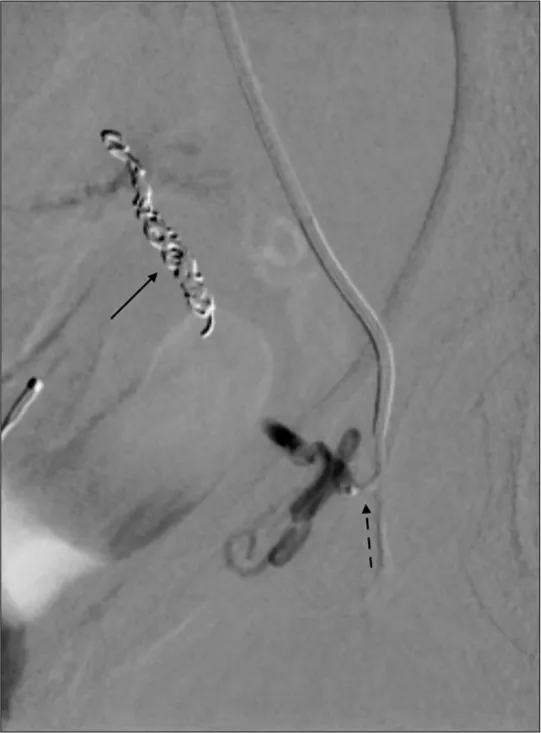
⭐ Transarterial Chemoembolization (TACE) is a standard palliative treatment for unresectable Hepatocellular Carcinoma (HCC), often improving survival and quality of life by local tumor control and reducing tumor burden.
Embolization: How & Hazards - Navigating Flow
- How: Catheter-directed delivery of agents to occlude target blood flow.
- Access: Femoral (common), radial.
- Guidance: Fluoroscopy, DSA.
- Agents: Coils, particles (PVA, Gelfoam), liquids (glue, Onyx).
- Technique: Superselective catheterization.
- Hazards:
- Non-target embolization (NTE) → ischemia.
- Post-embolization syndrome (PES): Fever, pain, nausea (common, self-limiting).
- Access site: Hematoma, pseudoaneurysm.
- Vessel injury, contrast allergy.
- Navigating Flow:
- Crucial: Vascular anatomy, flow dynamics.
- Control: Balloon occlusion, flow-directed catheters.

⭐ Non-target embolization (NTE) is a critical complication; meticulous technique and anatomical knowledge are vital to prevent it.
High‑Yield Points - ⚡ Biggest Takeaways
- Embolization treats active bleeding (trauma, GI), tumors (HCC via TACE), and uterine fibroids (UAE).
- Agents: Gelfoam (temporary), coils & particles (permanent), glue, Onyx.
- BAE is life-saving in massive hemoptysis.
- PVE promotes liver remnant hypertrophy before major hepatectomy.
- TACE combines targeted chemotherapy with ischemia for HCC.
- Post-embolization syndrome (fever, pain) is a common, expected outcome.
- Non-target embolization is a serious complication to avoid.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

