Introduction & Indications - Gunk Be Gone!
- Image-guided, minimally invasive procedures to aspirate or drain pathological fluid collections (pus, bile, urine, serous fluid).
- Aims:
- Diagnostic: Obtain fluid for analysis (microbiology, cytology).
- Therapeutic: Relieve pressure, control sepsis, decompress obstructed systems.
- Common Indications:
- Abscesses: Intra-abdominal, pelvic, hepatic, renal.
- Pathological Fluid: Pleural effusion (empyema), ascites, pericardial effusion, cysts, bilomas, urinomas, lymphoceles.
- Obstructive Processes: Biliary (PTBD), Urinary (PCN).

⭐ Percutaneous drainage is often preferred over surgical drainage due to lower morbidity, shorter hospital stay, and cost-effectiveness.
Pre-Procedure Planning - Plan Before Puncture
- Patient Evaluation:
- Clinical status, comorbidities.
- Coagulation: INR < 1.5, Platelets > 50,000/µL.
- Renal function (e.g., for contrast if CT-guided).
- Allergies.
- Informed Consent: Documented discussion of risks, benefits, alternatives.
- Antibiotics: Prophylactic, as per institutional protocol.
- Imaging Review & Route Planning:
- USG: Initial assessment, fluid characterization.
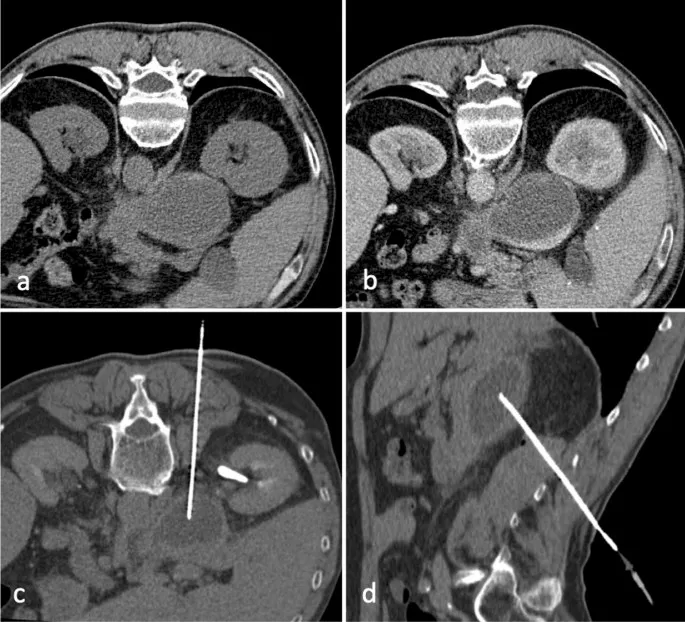
- CT: Defines collection extent, relation to vital structures, optimal access window.
- Plan safest, shortest access route.
⭐ Always confirm coagulation parameters (INR < 1.5, Platelets > 50,000/µL) are met before needle puncture to minimize bleeding complications.
Techniques & Equipment - Pokes & Pipes
- Imaging Guidance: Choose based on target visibility, depth, safety.
- Ultrasound (USG): Real-time, no radiation; best for superficial, fluid-filled collections.
- Computed Tomography (CT): Excellent anatomical detail, deep access; uses ionizing radiation.
- Fluoroscopy: Dynamic imaging, contrast use; for biliary/urinary systems, catheter checks.
- Access Techniques (Pokes):
- Seldinger Technique: Needle → guidewire → dilator(s) → catheter. Preferred for safety, especially deep/vascular.
- Trocar Technique: Direct puncture with catheter over sharp stylet. Faster, for superficial, easily accessible collections.
- Drainage Catheters (Pipes): Material: Polyurethane, silicone.
- Pigtail: Locking loop prevents migration. Common sizes: 8-14 Fr.
- Malecot: Winged tip for anchoring.
- Sump: Double lumen (drainage + air vent); prevents vacuum, for viscous/debris-laden fluid.
⭐ The Seldinger technique is the most widely used method for obtaining percutaneous access for drainage procedures due to its controlled, sequential nature, minimizing complications.
Common Drainage Procedures - Drainage Drilldown
- Percutaneous Abscess Drainage (PAD)
- Abdominal/Pelvic: Seldinger or trocar technique. Catheter 8-14 Fr. Guided by US/CT.
- Soft Tissue: Primarily US-guided. Smaller catheters often suffice.
- Percutaneous Transhepatic Biliary Drainage (PTBD)
- Indications: Obstructive jaundice (malignant/benign), cholangitis.
- Access: Right mid-axillary line, intercostal approach into bile duct.
- Complications: Hemorrhage, sepsis, bile leak/peritonitis.
- Percutaneous Nephrostomy (PCN)
- Indications: Obstructive uropathy, urinary diversion, access for interventions.
- Access: US/fluoroscopy-guided posterolateral approach (below 12th rib) into renal pelvis.
- Catheter: 8-12 Fr pigtail.
- Pleural/Pericardial Fluid Drainage
- Pleural: US-guided thoracentesis/chest tube.
Post-Procedure Care & Complications - Oops & Outcomes
- Care: Monitor vitals, drain output (volume, character), site. Flush with 10-20 mL saline q8-12h.
- Removal Criteria: Output < 10-20 mL/24h; clinical & imaging resolution.
- Complications:
- Early: Hemorrhage, pain, pneumothorax (thoracic).
- Late: Infection, catheter blockage/dislodgement.
- Blockage: ↓Output. Attempt flush; check position if fails.
⭐ Key for drain removal: Output < 10-20 mL/day, infection signs resolved, and collection resolution on follow-up imaging.
High‑Yield Points - ⚡ Biggest Takeaways
- Abscess drainage is the cornerstone of IR drainage, targeting localized infections.
- Ultrasound (US) and Computed Tomography (CT) are the workhorse guidance modalities.
- Pigtail catheters are favored for their atraumatic insertion and self-retaining design.
- Crucial pre-procedure: Ensure INR <1.5 and platelet count >50,000/μL.
- Key complications: Hemorrhage, sepsis, organ injury, and catheter malfunction.
- Seldinger technique offers precise access, especially for deep or small collections.
- Drainage effectively palliates malignant pleural effusions and ascites.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


