Biliary Anatomy & Access - Gut's Golden Pipes
- Intrahepatic Ducts: Right & Left hepatic ducts converge to form Common Hepatic Duct (CHD).
- Extrahepatic Ducts:
- Gallbladder → Cystic Duct.
- Cystic Duct + CHD → Common Bile Duct (CBD).
- CBD + Pancreatic Duct → Ampulla of Vater → Duodenum.
- Percutaneous Access:
- Right-sided: Mid-axillary line, transhepatic, commonest.
- Left-sided: Subxiphoid, for isolated left ductal system.
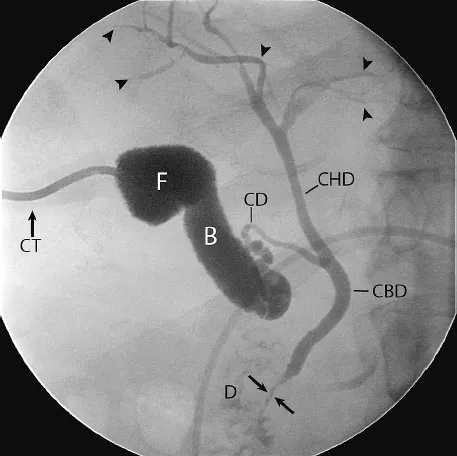
⭐ The most common percutaneous biliary access is via a right mid-axillary transhepatic approach, targeting a peripheral right hepatic duct (segments 6 or 7).
Indications & Contraindications - Green Light, Red Light
⭐ PTBD is often preferred for high biliary obstructions (e.g., Klatskin tumors), while ERCP is typically first-line for distal obstructions.
Biliary Procedures - The IR Plumber's Toolkit
-
Percutaneous Transhepatic Biliary Drainage (PTBD): Decompresses obstructed biliary system.
- Access: Typically Rt. mid-axillary, US/fluoroscopy guided.
- Drainage Types: Internal-external (across stricture) or purely external.
- Key Uses: Malignant/benign obstructive jaundice, acute cholangitis, pre-operative decompression.
-
Biliary Stenting: Maintains biliary duct patency post-dilatation or for palliation.
- Plastic Stents: Temporary, smaller diameter; for benign strictures, require frequent exchanges.
- Self-Expanding Metallic Stents (SEMS): Larger diameter, longer patency; for malignant obstructions.
- Covered SEMS: Prevent tumour ingrowth, potentially removable; higher migration risk.
- Uncovered SEMS: Embed into wall, less migration; risk of tumour ingrowth/epithelial hyperplasia causing occlusion.
-
Percutaneous Cholecystostomy (PC): Drains gallbladder in high-risk patients.
- Main Indication: Acute cholecystitis when surgery is contraindicated.
- Technique: US-guided transhepatic or transperitoneal catheter placement.
-
Other Interventions:
- Biliary Dilatation: Balloon catheters for benign/malignant strictures.
- Stone Extraction: Using baskets (e.g., Dormia) or balloons, often via T-tube tract or PTBD access.

⭐ In malignant biliary obstruction, SEMS (Self-Expanding Metallic Stents) offer superior long-term patency compared to plastic stents.
Complications & Management - Navigating Rough Waters
- Hemorrhage:
- Arterial: Angioembolization.
- Venous: Pressure, often self-limiting.
- Sepsis/Cholangitis:
- IV antibiotics.
- Ensure/optimize biliary drainage.
⭐ Acute cholangitis (Charcot's triad: fever, jaundice, RUQ pain) is a critical risk; manage with IV antibiotics & urgent biliary drainage.
- Bile Leak/Biloma:
- Percutaneous drainage of collection.
- Consider stent adjustment/new placement.
- Pancreatitis:
- Usually mild; supportive care (NPO, analgesia).
- Pneumothorax (supracostal access):
- Observe if small; chest tube if symptomatic/large.
- Catheter Issues (Dislodgement/Occlusion):
- Fluoroscopic repositioning.
- Flush; if fails, exchange catheter.
High‑Yield Points - ⚡ Biggest Takeaways
- PTBD is vital for biliary obstruction if ERCP fails or is contraindicated.
- Right-sided PTBD access is standard, targeting peripheral ducts to minimize risks.
- Key PTBD complications: hemobilia, sepsis, bile leak, pneumothorax.
- Metallic stents offer superior long-term patency over plastic stents in malignant strictures.
- Percutaneous cholecystostomy drains acute cholecystitis in surgically high-risk patients.
- Rendezvous technique combines percutaneous and endoscopic routes for challenging biliary access.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

