QIBs: The Basics - Numbers Game Unlocked
- QIB: Objective, quantifiable image-derived metric; measures (patho)physiology.
- Purpose: Disease detection, staging, prognosis, monitoring treatment response.
- Hallmarks (📌 RARP): Repeatability, Accuracy, Reproducibility, Precision.
- Key Examples:
- ADC (DWI): Low values (e.g., < 1.0 x $10^{-3} \text{ mm}^2/\text{s}$) suggest restricted diffusion (tumors, ischemia).
- SUV (PET): High values (e.g., SUVmax > 2.5) often indicate malignancy.
- RECIST: Standardized tumor response criteria.
- Workflow:
⭐ QIBs like ADC and SUV are crucial for differentiating benign vs. malignant lesions and assessing early treatment response.
PET QIBs - Sweet Spots & Hot Counts
- Standardized Uptake Value (SUV): Primary PET QIB.
- $SUV_{max}$: Max uptake in Region of Interest (ROI).
- $SUV_{mean}$: Avg. uptake in ROI.
- $SUV_{peak}$: Avg. in small ROI around $SUV_{max}$; robust.
- Influencers: Blood glucose, uptake time, patient size, reconstruction.
- Metabolic Tumor Volume (MTV): Volume of tumor with uptake > threshold.
- Total Lesion Glycolysis (TLG): $MTV \times SUV_{mean}$; total metabolic burden.
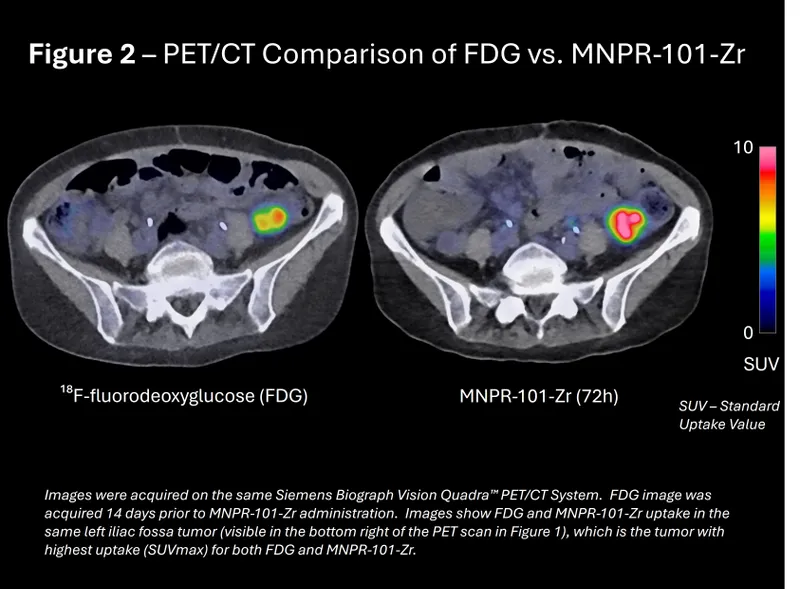
- PERCIST 1.0: Standardizes solid tumor PET response.
- Uses $SUL_{peak}$ (SUV normalized to liver). Tracks up to 5 lesions.
⭐ $SUV_{peak}$ is preferred in PERCIST: less noise-sensitive, more reproducible than $SUV_{max}$.
- Deauville Score (Lymphoma): 5-point FDG-PET response.
- Compares lesion to mediastinum (M) & liver (L).
- 1: No uptake. 2: Uptake ≤M. 3: Uptake >M but ≤L. 4: Mod. >L. 5: Marked >L/new.
- Scores 1-3 often indicate good response/Complete Metabolic Response (CMR).
MRI QIBs - Mapping Micro‑Worlds
- MRI QIBs: Objective, numerical data on tissue properties.
- Key Techniques:
- DWI/ADC: Measures water diffusion. ADC ($mm^2/s$) ↓ in tumors, ischemia; ↑ in cysts.
⭐ ADC values are critical for differentiating malignant from benign lesions and assessing early ischemic stroke.
- DTI/FA: White matter integrity. FA (0-1) reflects diffusion directionality. For TBI, MS.
- DCE-MRI: Perfusion & permeability ($K^{trans}$, $v_e$, $k_{ep}$). Tumor angiogenesis.
- MRS: Metabolite levels (NAA, Cho, Cr, Lac). 📌 "Chopping Tumors": Cho ↑ (tumors). NAA ↓ (neuronal injury).
- ASL: Non-contrast perfusion (CBF in $mL/100g/min$).
- Relaxometry (T1, T2, T2 maps):* Quantitative relaxation times. T1: myocardial fibrosis; T2: cartilage; T2*: iron.
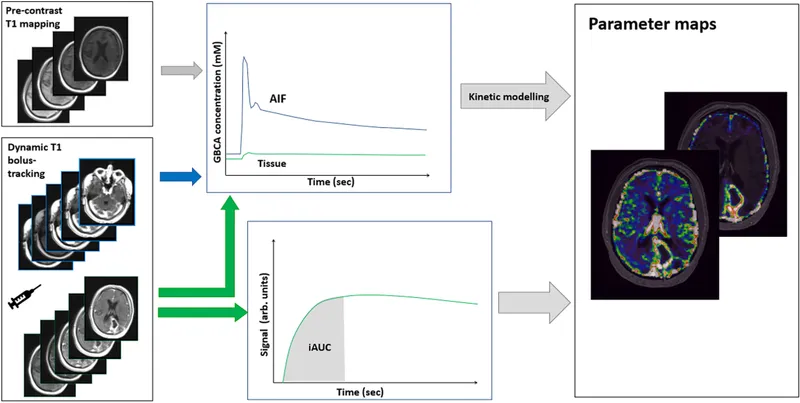
- DWI/ADC: Measures water diffusion. ADC ($mm^2/s$) ↓ in tumors, ischemia; ↑ in cysts.
QIBs: Validation & Clinics - Trust The Numbers
QIBs provide objective measures, but rigorous validation is crucial for clinical confidence and "trusting the numbers."
- Validation Pathway:
- Technical: Confirms QIB measurement integrity (Accuracy, Precision, Repeatability, Reproducibility).
- Biological/Clinical: Establishes QIB relevance to disease status or treatment efficacy.
- Clinical Significance:
- Enhances diagnostic accuracy, staging, and prognostic assessment.
- Objectively monitors therapy response (e.g., RECIST, ADC [malignancy often < 1.0 x $10^{-3}$ mm²/s], SUV).
- QIBA (Quantitative Imaging Biomarkers Alliance) spearheads standardization efforts.
⭐ ADC values (DWI) are pivotal QIBs; ↓ADC often indicates malignancy due to restricted diffusion in dense cellular areas.
- Adoption Challenges: Achieving widespread standardization, managing inter-scanner/operator variability, seamless clinical workflow integration.
High‑Yield Points - ⚡ Biggest Takeaways
- QIBs: Objective, measurable features from images, enabling quantitative medical assessment.
- Vital for diagnosis, staging, prognosis, and tracking treatment response accurately.
- Common examples: ADC (DWI), SUV (PET), HU (CT), T1/T2 maps (MRI).
- Allow non-invasive monitoring of disease activity and therapeutic effects.
- Reproducibility and standardization are crucial for reliable clinical application.
- Challenges: Technical variability, ensuring robust validation across diverse settings.
- Key drivers for precision medicine, radiomics, and AI in healthcare.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

