Functional MRI - Brain's Busy Blood
- Measures brain activity by detecting changes in blood flow. Relies on the Blood-Oxygen-Level Dependent (BOLD) effect.
- BOLD Mechanism:
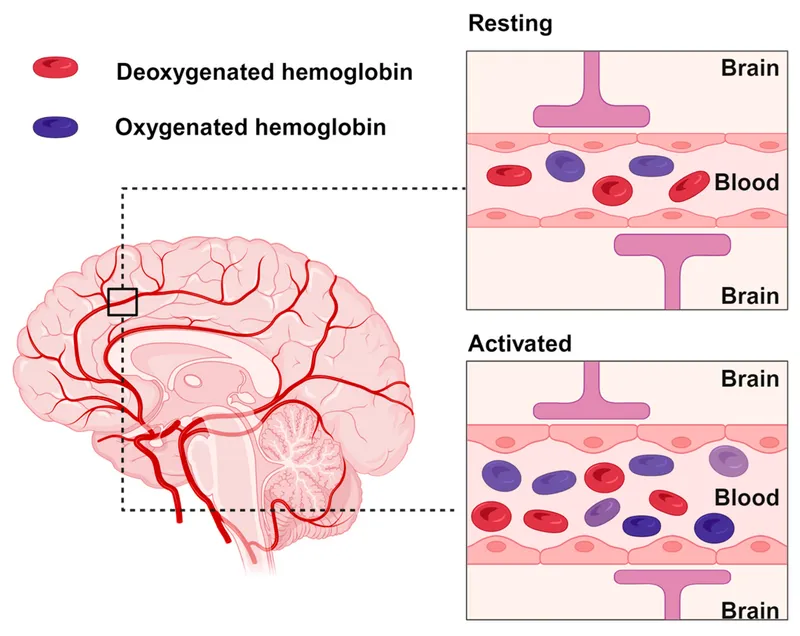
- Neuronal activation ↑ → Local blood flow ↑ & oxygen delivery ↑.
- Results in ↑ oxyhemoglobin (diamagnetic) & ↓ deoxyhemoglobin (paramagnetic).
- Deoxyhemoglobin acts as an endogenous contrast agent.
- Signal: ↑ Neural activity → ↓ deoxyhemoglobin → ↑ T2* signal.
- Sequence: Typically T2*-weighted Gradient Echo (GRE) Echo-Planar Imaging (EPI).
- Uses: Pre-surgical mapping of eloquent cortex (e.g., motor, language areas), neuroscience research.
- Pros: Non-invasive, no ionizing radiation, good spatial resolution.
- Cons: Indirect measure of neural activity, relatively poor temporal resolution (seconds), susceptible to motion artifacts.
⭐ Deoxyhemoglobin is paramagnetic, acting as an endogenous contrast agent in BOLD fMRI.
Functional MRI - Probing the Mind
-
Measures brain activity via Blood-Oxygen-Level-Dependent (BOLD) signal, an indirect marker of neural activity. Relies on neurovascular coupling: ↑ neural activity → ↑ local blood flow & oxygenation → ↑ $T_2^*$ signal.
-
Experimental Paradigms:
Design Type Stimuli Power Temp. Res. Block Alternating states ↑ Higher ↓ Lower Event-Related Discrete, brief ↓ Lower ↑ Higher 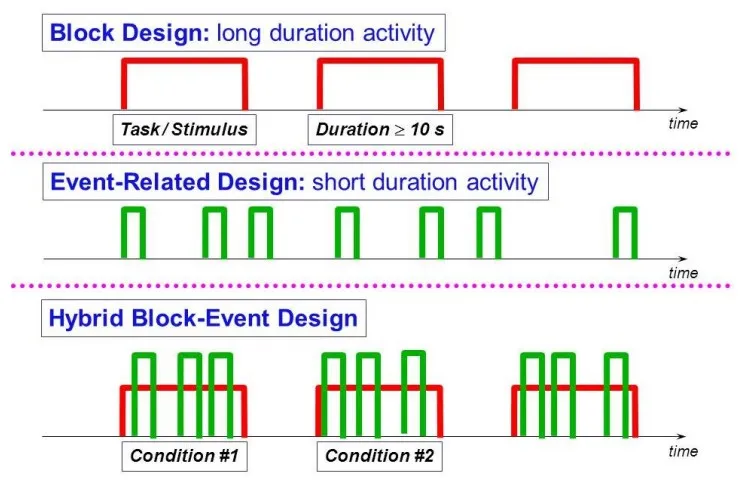
-
fMRI Acquisition Steps:
⭐ Block designs generally offer higher statistical power for detecting activation, while event-related designs provide better temporal resolution for individual stimuli.
- Key sequence: Echo-Planar Imaging (EPI) for rapid $T_2^*$-weighted images, crucial for capturing BOLD changes.
Functional MRI - Unmasking Activity
- Measures brain activity by detecting changes in blood flow: Blood-Oxygen-Level-Dependent (BOLD) signal.
- Neural activity → ↑ regional blood flow → ↑ oxyhemoglobin / ↓ deoxyhemoglobin ratio → ↑ T2* signal.
- Applications: Mapping motor, sensory, cognitive functions; presurgical planning for eloquent cortex.
- Key Preprocessing Steps: 📌 Many Smart Colleagues Need Sleep (Motion Correction, Slice Timing Correction, Coregistration, Normalization, Smoothing).
- Typical Parameters:
- Spatial resolution: 2-4 mm.
- Temporal resolution: 1-3 s.
- Smoothing kernel (FWHM): 4-8 mm.
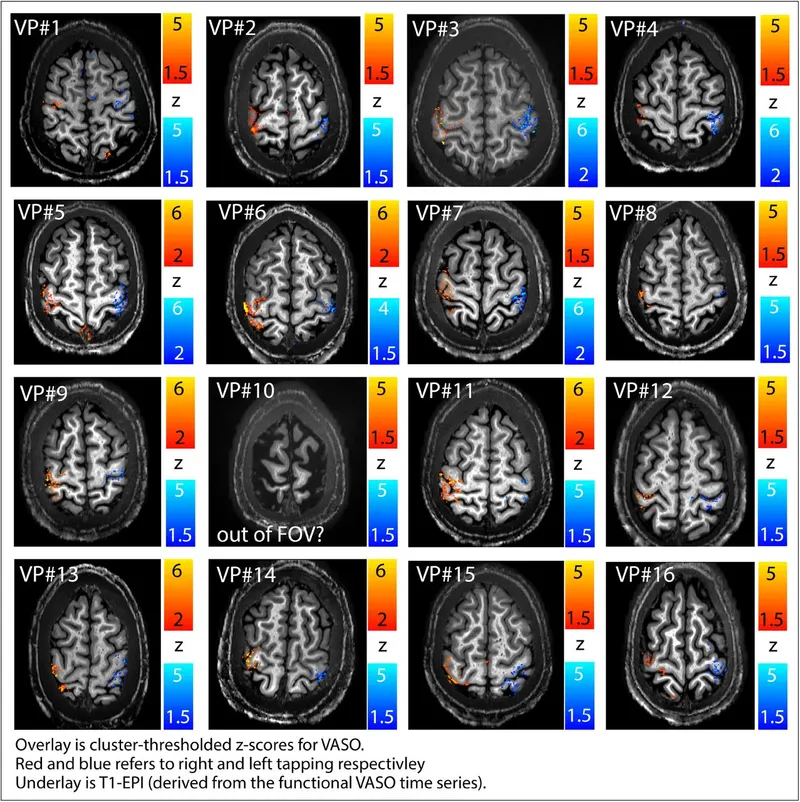
⭐ Motion correction is a critical preprocessing step in fMRI, as even small head movements (e.g., >1-2mm) can introduce significant artifacts, corrupting BOLD signal interpretation and localization of activity.
Functional MRI - Mapping & Mysteries
- Principle: Blood-Oxygen-Level Dependent (BOLD) contrast.
- Neuronal activity → ↑ blood flow → ↑ oxyHb/↓deoxyHb ratio → ↑ T2* signal.
- Neurovascular Coupling: Links neural activity to local hemodynamic changes.
- Key Applications:
- Presurgical Mapping: Motor, sensory, language areas; identifies eloquent cortex near lesions (e.g., tumors, AVMs).
- Language Lateralization: Dominant hemisphere identification (Broca's, Wernicke's areas).
- Research: Cognitive functions, psychiatric disorders.
- Types:
- Task-based fMRI: Subject performs specific tasks during scanning.
- Resting-state fMRI (rs-fMRI): Measures spontaneous brain activity, assessing functional connectivity.
- Mysteries & Limitations:
- Indirect measure of neuronal activity.
- Susceptible to motion & susceptibility artifacts (signal dropout, e.g., near sinuses).
- Relatively lower spatio-temporal resolution vs. direct electrophysiology.
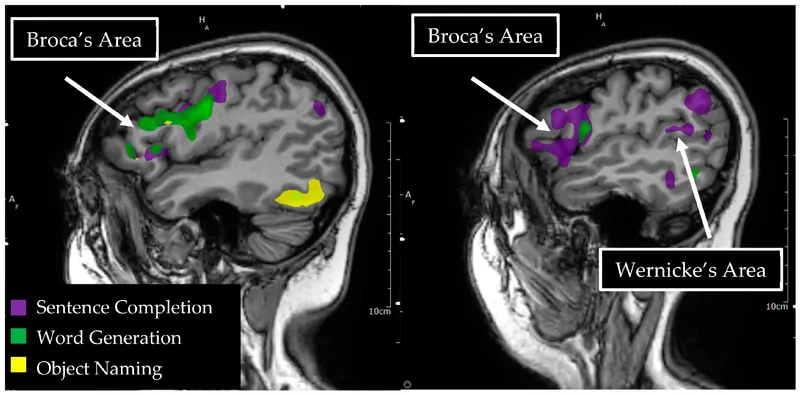
⭐ Presurgical fMRI for language lateralization (e.g., identifying Broca's and Wernicke's areas) is a key application to minimize post-operative neurological deficits in neurosurgery for lesions near eloquent cortex.
High‑Yield Points - ⚡ Biggest Takeaways
- fMRI primarily utilizes BOLD (Blood-Oxygen-Level Dependent) contrast.
- It non-invasively maps brain activity by detecting hemodynamic responses.
- Deoxyhemoglobin is paramagnetic, creating local field inhomogeneities.
- Increased neural activity leads to ↑ blood flow, ↓ deoxyhemoglobin, and ↑ T2 signal*.
- Crucial for presurgical mapping of motor, sensory, and language areas.
- Resting-state fMRI (rs-fMRI) assesses functional connectivity between brain regions.
- Susceptible to motion artifacts and physiological noise; requires patient cooperation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

