Aortic Dissection & AAA Rupture - Aorta's Acute Agonies
Aortic Dissection: Acute tear in aortic intima, blood enters media.
- Classifications:
-
Stanford: 📌 A = Ascending aorta involved (surgical emergency); B = Beyond (descending only, medical Rx typically).
-
DeBakey: I (Ascending + Arch/Descending), II (Ascending only), III (Descending only).
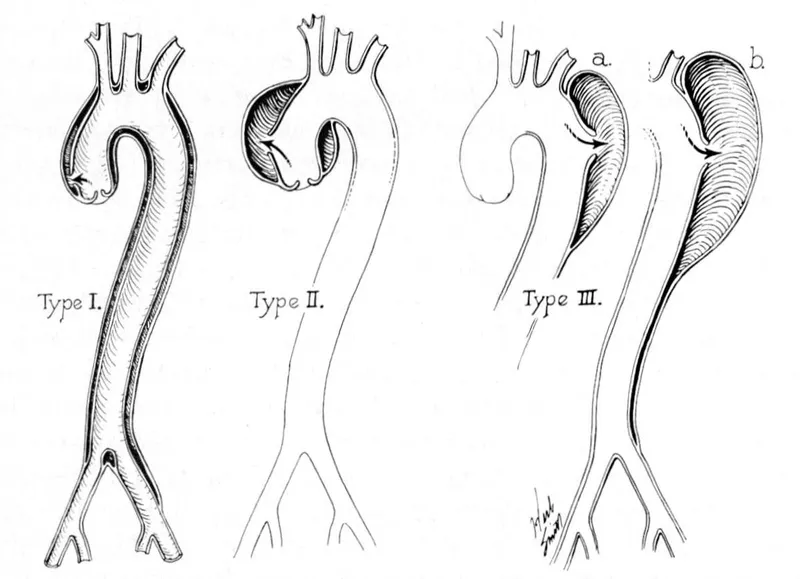
-
- CTA Findings:
- Intimal flap (key).
- True lumen (compressed), False lumen (larger, often thrombosed, beak sign).
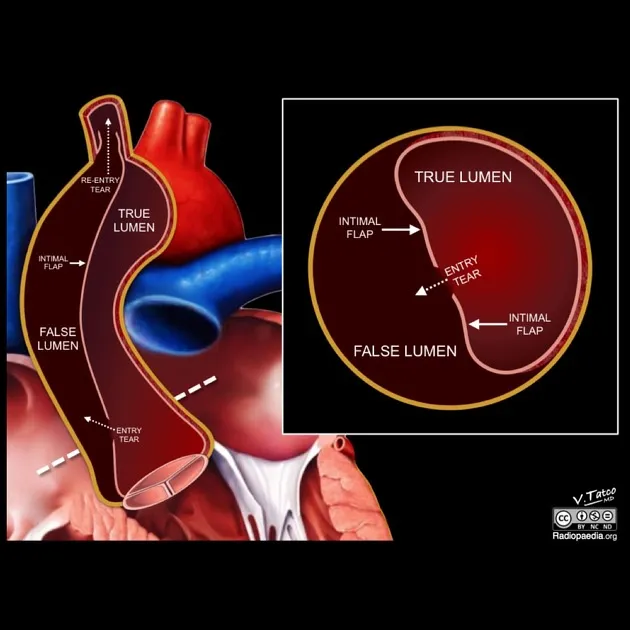
- Complications: Malperfusion, rupture.
Ruptured Abdominal Aortic Aneurysm (AAA):
- Aorta diameter > 3 cm; rupture risk ↑ if > 5.5 cm.
- CTA Signs of Rupture:
- Retroperitoneal hematoma (most common).
- Active contrast extravasation.
- Draped aorta sign.
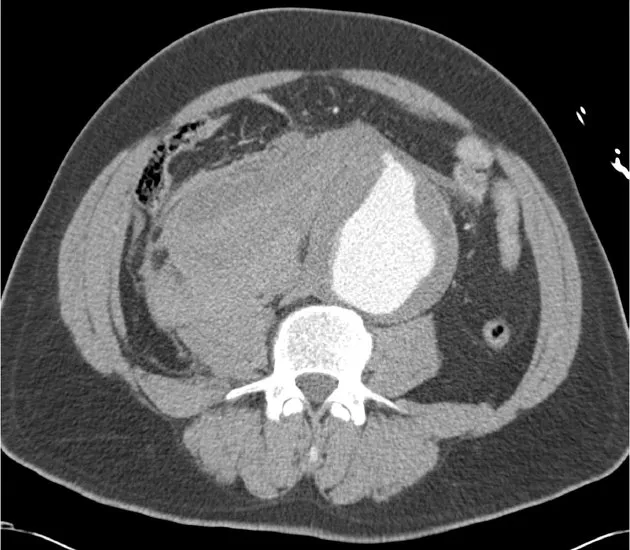
⭐ Sudden "tearing" chest/back pain is classic for aortic dissection.
Pulmonary Embolism - Clots' Lung Lodge
-
Risk stratification via Wells or Geneva scores guides investigation.
-
Diagnostic Algorithm:
-
CTPA (Gold Standard):
- Direct signs: Central filling defects (partial/complete occlusion), "polo mint" sign (cross-section), railway track sign (longitudinal).
- Saddle embolus: Large clot at main pulmonary artery bifurcation.
-
Ancillary Signs (CXR/CT):
- Westermark sign: Regional oligemia distal to embolus.
- Hampton's hump: Peripheral wedge-shaped opacity (infarct).
- Right heart strain: RV dilatation (RV/LV diameter ratio >1.0 on axial CT), septal bowing.
-
V/Q Scan: For CTPA contraindications (e.g., renal failure, contrast allergy); identifies ventilation-perfusion mismatches.
⭐ The "polo mint" sign on CTPA, representing a central filling defect surrounded by contrast, is a direct sign of acute PE.
Acute Stroke Imaging - Brain's Blood Blockade
-
Non-Contrast CT (NCCT): First-line to exclude hemorrhage.
- Early ischemic signs (<6 hrs): Hyperdense MCA sign (clot), loss of grey-white differentiation, insular ribbon sign (obscuration), sulcal effacement.
- Early ischemic signs (<6 hrs): Hyperdense MCA sign (clot), loss of grey-white differentiation, insular ribbon sign (obscuration), sulcal effacement.
-
CT Angiography (CTA): Identifies vessel occlusion site (e.g., LVO).
-
CT Perfusion (CTP): Differentiates core (irreversible damage: ↓CBF, ↓CBV) from penumbra (salvageable tissue: ↓CBF, normal/↑CBV, ↑MTT/TTP).
-
MRI Brain: Gold standard for early infarct.
- DWI: Hyperintense (restricted diffusion) within minutes. ADC map: Corresponding hypointensity.
-
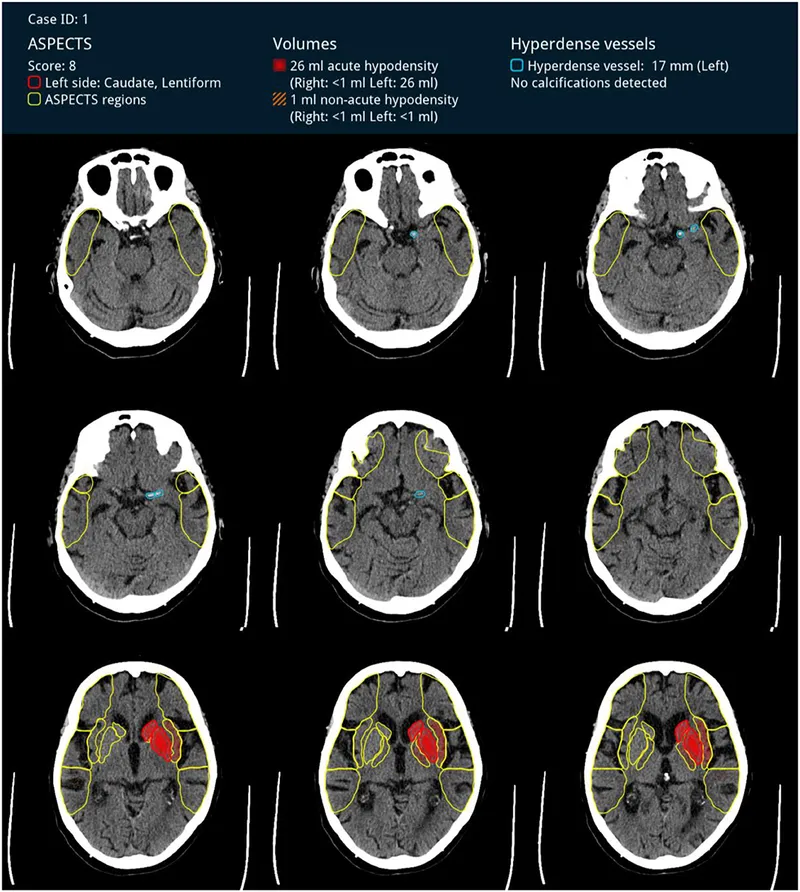
ASPECTS (Alberta Stroke Program Early CT Score): Quantifies early MCA ischemic changes on NCCT. Score 0-10 (10=normal). Lower score = worse outcome.
- 📌 Areas: Caudate, Lentiform nucleus, Internal capsule, Insular cortex, plus M1-M6 (MCA cortical regions).
⭐ DWI is the most sensitive sequence for detecting acute ischemic stroke within minutes of onset.
Mesenteric & Limb Ischemia - Gut & Limb Peril
-
Mesenteric Ischemia: Critical reduction in intestinal blood flow.
-
Arterial (AMI): SMA most common. Embolic (AFib) or thrombotic.
- CTA (Gold Standard): SMA/IMA occlusion; bowel wall changes (thickening/hyperemia → thin/↓enhancement); pneumatosis intestinalis; portal venous gas (PVG).
-
Venous (MVT): SMV common. Hypercoagulable states, portal HTN.
- CTA: SMV/portal vein filling defect, bowel wall thickening, mesenteric congestion. ⭐ > Pneumatosis intestinalis & portal venous gas on CTA: ominous signs of advanced mesenteric ischemia, suggest infarction.
-
-
Acute Limb Ischemia (ALI): Sudden ↓limb perfusion; threatens viability. 📌 6 P's (Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia).
- Doppler US: Initial; confirms ↓/absent flow, locates occlusion.
- CTA: Definitive; shows occlusion/stenosis (level/extent), collaterals. "Meniscus sign" or abrupt cut-off.
High‑Yield Points - ⚡ Biggest Takeaways
- Aortic Dissection: CTA gold standard; Stanford A (ascending) surgical, Type B medical.
- Pulmonary Embolism: CTPA diagnostic choice; shows pulmonary artery filling defects.
- DVT: Compression US (CUS) reveals non-compressible deep veins.
- Acute Mesenteric Ischemia: CTA crucial; shows bowel wall thickening, pneumatosis.
- Ischemic Stroke: Initial NCCT head excludes hemorrhage; MRI (DWI) for acute infarct.
- SAH: NCCT head detects blood; CTA identifies aneurysm.
- Traumatic Vascular Injury: CTA shows active extravasation, pseudoaneurysm, dissection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

