Trauma Imaging Protocols - Code Red First Scans
-
eFAST (Extended Focused Assessment with Sonography for Trauma)
- Views: Pericardial (subxiphoid), RUQ (hepatorenal), LUQ (splenorenal), Pelvic (suprapubic), Anterior thoracic (lung sliding).
- Detects: Free fluid (pericardial, pleural, peritoneal, pelvic), pneumothorax.
- 📌 Mnemonic (FAST views): "Right Upper, Left Upper, Pelvic, Cardiac" (RUQ, LUQ, Pelvic, Subxiphoid).
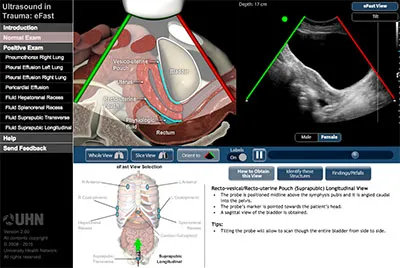
⭐ eFAST: High specificity (95-100%) for intraperitoneal free fluid (detects ≥100-200 ml).
-
Chest X-ray (CXR - AP Supine)
- Assess: Lines/tubes, pneumothorax, hemothorax, widened mediastinum (>8 cm), rib fractures, pulmonary contusion.
-
Pelvis X-ray (AP View)
- Indications: Pelvic pain/instability, altered sensorium, distracting injury.
- Look for: Fractures (e.g., pubic rami, SI joint disruption), malalignment.
-
Other Portable X-rays (if CT delayed/unavailable)
- C-spine: Lateral view (must see C7-T1).
- Extremities: Based on clinical findings for suspected fractures.
Trauma Imaging Protocols - Pan-Scan Power Play
- Whole-Body CT (WBCT) / Pan-Scan: Rapid, comprehensive CT for major trauma.
- Indications:
- High-energy trauma (e.g., fall >5m, RTC >60km/hr)
- Multiple injuries (≥2 body regions)
- Altered sensorium (GCS <13)
- Unstable but transient responder to resuscitation
- Specific injury patterns (e.g., seatbelt sign)
- Protocol Components:
- NCCT Head & C-spine
- CECT Chest (arterial phase)
- CECT Abdomen & Pelvis (portal venous phase; consider arterial for active bleed, delayed for urothelial injury)
- Advantages: Rapid assessment, ↓ time to diagnosis, potential improved survival in select polytrauma.
- Disadvantages: Radiation (effective dose ~10-25 mSv), contrast risks (CIN, allergic reaction), potential over-investigation.
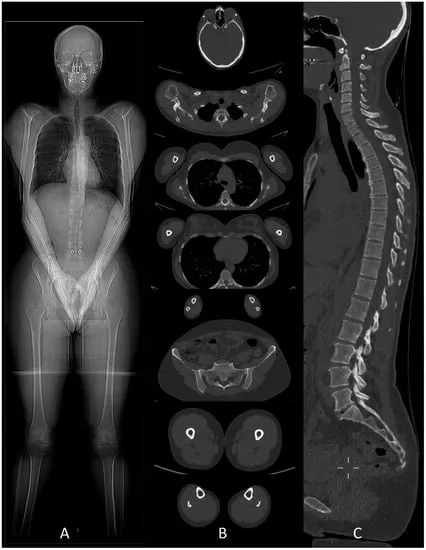
⭐ WBCT is associated with a survival benefit in patients with severe trauma (Injury Severity Score ISS > 15).
Trauma Imaging Protocols - Injury Zone Imaging
- Head Trauma:
- NCCT Head: Key for EDH, SDH, SAH, IVH, contusions, DAI signs.
- CT Angio/Venography: Indicated for suspected vascular injury (e.g., dissection, occlusion with specific fracture patterns like skull base #, penetrating trauma).
- Spine Trauma:
- CT C-spine, T-spine, L-spine: Indications based on NEXUS/Canadian C-Spine rules (CCR) 📌.
- MRI: For neurological deficit unexplained by CT, suspected ligamentous injury, spinal cord injury (SCI), epidural hematoma.
- Cervical Spine Clearance Algorithm:
- Thoracic Trauma:
- Beyond initial CECT chest: CT Aortogram for suspected traumatic aortic injury (mediastinal hematoma, abnormal aortic contour, intimal flap).
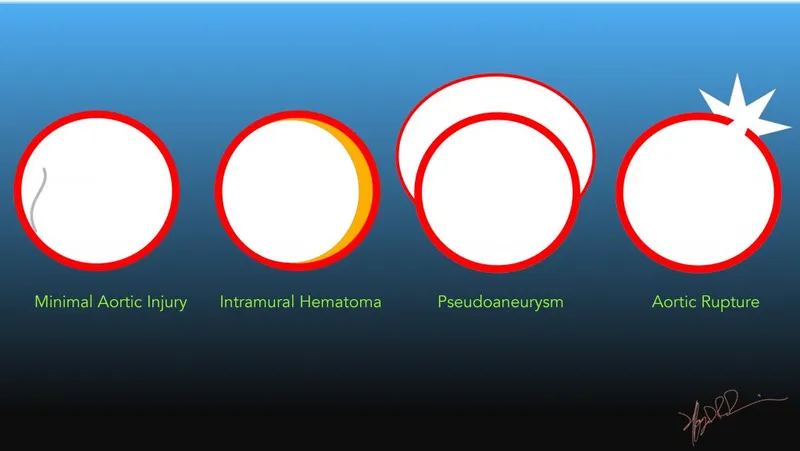
- Beyond initial CECT chest: CT Aortogram for suspected traumatic aortic injury (mediastinal hematoma, abnormal aortic contour, intimal flap).
- Abdominal/Pelvic Trauma:
- Triple Contrast CT (oral, rectal, IV): Consider for suspected bowel/hollow viscus injury (less common now).
- CT Cystography (direct contrast instillation): For suspected bladder rupture.
⭐ The most common site of traumatic aortic injury is the aortic isthmus, typically just distal to the origin of the left subclavian artery.
Trauma Imaging Protocols - Special Cases & Safety
- Contrast Media in Trauma:
- IV iodinated contrast for CECT: assess solid organ/vascular injury, active bleeding.
- Risks: Contrast-Induced Nephropathy (CIN), allergic reactions (premedicate if prior history), manage extravasation.
- Pediatric Trauma Imaging:
- Adhere to Image Gently & ALARA principles.
- Prioritize USS/MRI; use age/weight-adjusted CT protocols (↓kVp, ↓mAs); consider focused CT.
⭐ In pediatric trauma, the 'Image Gently' campaign emphasizes dose reduction strategies without compromising diagnostic quality.
- Pregnant Trauma Patients:
- Maternal life is priority; shield fetus when possible.
- USS/MRI preferred; CT justified if benefits outweigh risks; counsel patient.
- Fetal radiation effects: dose/gestation-dependent (threshold >50-100 mGy).
- Radiation Safety:
- Justification (is scan necessary?) & Optimization (ALARA - as low as reasonably achievable).
- Awareness of cumulative radiation dose.
High‑Yield Points - ⚡ Biggest Takeaways
- ABCDE approach dictates trauma imaging priorities.
- eFAST is key for initial assessment of hemoperitoneum and pneumothorax in unstable patients.
- Whole-Body CT (WBCT) is preferred for stable polytrauma patients.
- CT C-spine is superior to X-ray; use NEXUS/Canadian C-Spine Rule for clearance.
- CECT is essential for organ/vascular injury and detecting active bleeding.
- X-rays remain useful for extremity fractures and initial chest/pelvis views.
- Rapid imaging protocols are crucial for timely intervention.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

