Acute Stroke Imaging - Brain Attack Basics
- Goal: Rapidly differentiate ischemic vs. hemorrhagic stroke; guide reperfusion therapy. "Time is Brain!"
- Initial Imaging: Non-Contrast CT (NCCT)
- Primary: Exclude hemorrhage (hyperdense).
- Early ischemic signs: Loss of grey-white differentiation, sulcal effacement, hyperdense MCA sign.
- ASPECTS score (0-10) on NCCT for MCA stroke.
- Ischemic Stroke Workup:
- MRI: Gold standard.
- DWI: Positive within minutes.
- ADC map: Confirms restricted diffusion.

- CTA: Detects Large Vessel Occlusion (LVO).
- CTP: Identifies core infarct vs. penumbra (target for reperfusion).
- MRI: Gold standard.
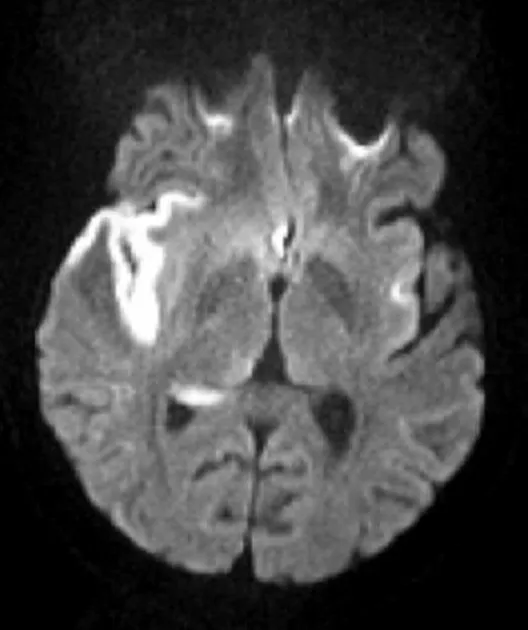
⭐ DWI hyperintensity with corresponding ADC hypointensity signifies restricted diffusion, visible within minutes (<30 min) of acute ischemic stroke onset.
CNS Infections - Brain Invaders
- Bacterial Meningitis:
- CT: Often normal; may show hydrocephalus, basal cistern effacement. Post-contrast: meningeal enhancement.
- MRI: Superior for leptomeningeal enhancement (FLAIR, T1+C); DWI for restricted diffusion of pus in sulci.
- Viral Encephalitis (Herpes Simplex - HSV):
- Typically affects temporal lobes, insula.
- CT: Early stages often normal; later may show hypodensity, edema.
- MRI: Characteristic T2/FLAIR hyperintensity, DWI restriction, petechial hemorrhages.
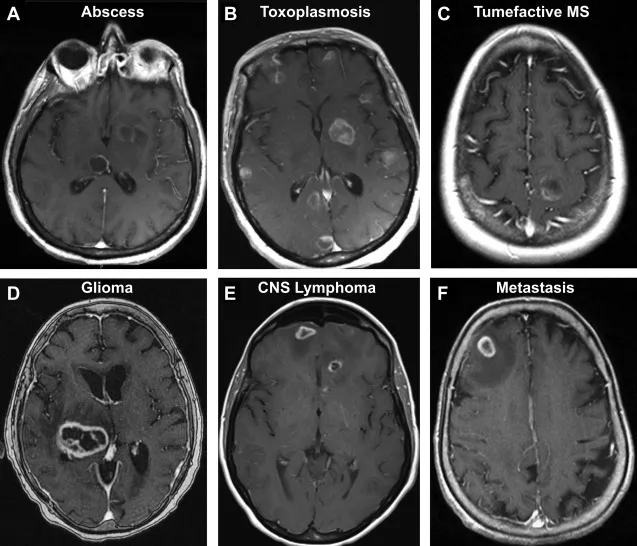
- Brain Abscess:
- CT/MRI: Central area of liquefaction necrosis, surrounded by a thick, enhancing rim and vasogenic edema.
- DWI: Central restricted diffusion is key for pyogenic abscess.
-
⭐ DWI restriction in the core of a pyogenic abscess is typical.
- Tuberculous Meningitis:
- Features: Thick basal meningeal enhancement, hydrocephalus, tuberculomas (ring-enhancing lesions). Infarcts common due to associated vasculitis.
Seizures & Status - Electric Storms
- Imaging Goal: Identify structural causes (e.g., tumor, stroke, infection, malformation) or complications.
- New-onset seizure: Non-contrast CT (NCCT) head initially to exclude acute bleed/mass.
- MRI: Superior for subtle epileptogenic lesions (e.g., mesial temporal sclerosis, cortical dysplasia, encephalitis).
- Status Epilepticus: May show reversible cortical/subcortical DWI restriction, T2/FLAIR hyperintensity, ↑perfusion; hippocampal changes common.

⭐ MRI is superior to CT for detecting subtle epileptogenic lesions; CT is often first-line in emergency new-onset seizures to exclude acute bleed/mass effect immediately threatening life or requiring urgent neurosurgical intervention (e.g. large hematoma, hydrocephalus).
Raised ICP & Hydrocephalus - Pressure Cooker Brain
- Raised ICP: Symptoms: Headache, vomiting, papilledema. Late: Cushing's triad. CT findings: Effaced sulci, compressed ventricles/cisterns.
- Hydrocephalus: ↑CSF volume causing ventricular dilatation (Evan's Index > 0.3).
- Acute sign: Transependymal CSF flow (periventricular lucency on CT / T2 hyperintensity on MRI).
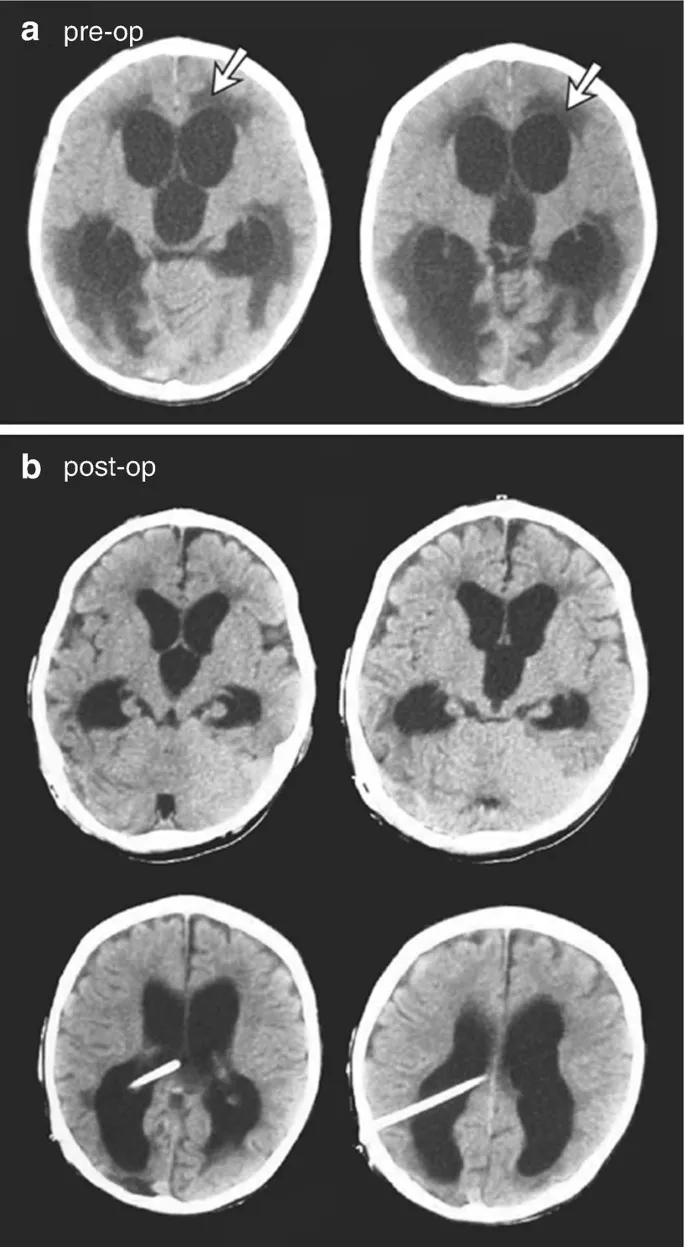
- ⭐
Transependymal CSF seepage (periventricular lucency on CT / T2 hyperintensity on MRI) indicates acute/uncompensated hydrocephalus.
- Differentiating Types:
Other Vascular Crises - Vessel Vendettas
| Aspect | Subarachnoid Hemorrhage (SAH) | Cerebral Venous Thrombosis (CVT) |
|---|---|---|
| Key NCCT Sign(s) | Hyperdense blood (cisterns) | "Cord sign", "Dense triangle sign" |
| Key CECT Sign(s) | - (CTA for aneurysm) | "Empty delta sign" (esp. SSS) |
| Grading / Gold Std. | Fisher Grade (CT blood); CTA (aneurysm) | MRV/CTV: Filling defect (gold) |
⭐ The "empty delta sign" on contrast-enhanced CT is a classic finding in superior sagittal sinus thrombosis.
High‑Yield Points - ⚡ Biggest Takeaways
- AIS: NCCT head first (no bleed); MRI (DWI) is most sensitive for early infarct.
- ICH: NCCT shows type, location, mass effect; CTA for underlying vascular causes.
- SAH: NCCT for acute blood; Angiography (CTA/DSA) vital for aneurysms.
- CVT: MRV/CTV are diagnostic; look for "empty delta sign" on CECT.
- CNS Infections: Contrast MRI for complications (e.g., abscess); DWI is key for herpes.
- PRES: MRI (FLAIR/T2) shows posterior reversible edema, typically parieto-occipital.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

