Imaging Modalities & Basics - Tools of Trade
- X-ray (Radiography):
- First-line for suspected fractures/dislocations.
- Requires 2+ orthogonal views (e.g., AP, Lateral); special views (scaphoid, mortise) if needed.
- Pros: Widely available, quick, inexpensive. Cons: Poor soft tissue detail, ionizing radiation.
- CT (Computed Tomography):
- Indications: Complex/occult fractures (articular involvement), pre-operative planning, spinal trauma.
- Pros: Excellent bone detail, multiplanar reconstruction. Cons: Higher radiation dose, more expensive.
- MRI (Magnetic Resonance Imaging):
- Indications: Soft tissue injuries (ligaments, tendons, menisci, cartilage), occult fractures (bone marrow edema), spinal cord injury, osteomyelitis, AVN.
- Pros: Superior soft tissue contrast, no ionizing radiation. Cons: Expensive, time-consuming, contraindications.
- US (Ultrasonography):
- Indications: Superficial soft tissue injuries (tendons, muscles), joint effusions, foreign bodies, pediatric fractures (cartilage), dynamic assessment.
- Pros: Real-time, dynamic, no radiation, portable. Cons: Operator-dependent, limited deep penetration.
⭐ Initial imaging for suspected fracture is X-ray (at least 2 orthogonal views).

Appendicular Skeleton Trauma - Limbs in Distress
Rapid identification of fracture patterns and dislocations is crucial. Common injuries include:
| Injury Type | Key X-ray Signs / Eponyms / Notes |
|---|---|
| Upper Limb | |
| Shoulder Dislocation | Anterior (>95%): Subcoracoid. Bankart, Hill-Sachs lesions. Posterior (rare): "Lightbulb" sign, trough line. Axillary view essential. |
| Colles' Fracture | Distal radius, dorsal displacement & angulation. "Dinner fork" deformity. FOOSH. |
| Smith's Fracture | Distal radius, volar displacement & angulation. "Garden spade" deformity. Reverse Colles'. |
| Monteggia Fracture | Proximal ulna fracture + anterior dislocation of radial head. |
| Galeazzi Fracture | Distal third radial shaft fracture + dislocation of distal radioulnar joint (DRUJ). |
| Lower Limb | |
| Hip Fracture | Intracapsular (subcapital, transcervical): Garden classification I-IV. High risk of AVN. Extracapsular (intertrochanteric, subtrochanteric). |
| Ankle Fracture (Weber) | Relates to fibula # level reference to syndesmosis. A: Below. B: At level. C: Above. Stability decreases A→C. |
📌 Mnemonic (GRIMUS): Galeazzi - Radius #, Inferior (Distal) RUJ dislocation; Monteggia - Ulna #, Superior (Proximal) Radial head dislocation.

Axial & Special Cases - Core & Unique Injuries
-
Physeal Injuries (Salter-Harris Classification):
- 📌 SALTER Mnemonic:
- I: Slipped (through physis)
- II: Above (physis + metaphysis)
- III: Lower (physis + epiphysis, intra-articular)
- IV: Through (metaphysis + physis + epiphysis, intra-articular)
- V: ERasure/Rammed (crush of physis)
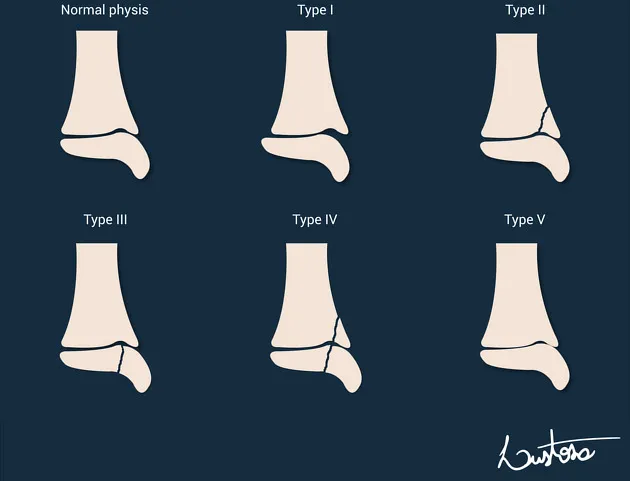
⭐ Salter-Harris Type II is the most common physeal fracture, involving fracture through the physis and metaphysis.
- 📌 SALTER Mnemonic:
-
Pelvic Ring Injuries: Stability is paramount.
- Young-Burgess: APC, LC, VS, CM. Tile: A (Stable), B (Rotationally Unstable), C (Vertically & Rotationally Unstable).
- Initial Stability Assessment:
- Spinal Trauma:
- Unstable examples: Jefferson (C1 burst), Hangman's (C2 pedicles), Chance (flexion-distraction).
- Denis 3-column theory: Involvement of ≥2 columns often implies instability.
High‑Yield Points - ⚡ Biggest Takeaways
- X-ray is first-line for suspected fractures/dislocations; obtain two orthogonal views.
- CT excels for complex/occult fractures (scaphoid, femoral neck) and surgical planning.
- MRI is best for soft tissue injuries (ligaments, tendons, menisci) and bone marrow edema.
- Salter-Harris fractures affect pediatric growth plates; accurate classification is vital.
- Positive fat pad signs (e.g., elbow) strongly suggest an occult fracture.
- Ultrasound (MSK) useful for superficial soft tissues, effusions, and dynamic assessment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

