Indications & Modalities - First Look, Right Scan
- Glasgow Coma Scale (GCS): Severity & Action
- Mild: 13-15
- Moderate: 9-12
- Severe: ≤8 (📌 Consider intubation)
- CT Head - Key Indications (Canadian CT Head Rule for GCS 13-15):
- GCS < 15 at 2h post-injury
- Suspected open/depressed skull fracture
- Signs of basal skull fracture (e.g., Battle's sign, raccoon eyes)
- Vomiting ≥2 episodes
- Age ≥65 years
- Amnesia before impact >30 min
- Dangerous mechanism (e.g., fall >3ft/5 stairs, MVA)
- Imaging Choice:
- CT (NCCT): Primary scan in acute trauma. Fast; detects bleeds, fractures.
- MRI: Subacute/chronic phase, suspected Diffuse Axonal Injury (DAI), if CT inconclusive.

⭐ In minor head trauma (GCS 13-15), CT is indicated if high/medium risk factors as per the Canadian CT Head Rule are present to rule out clinically important brain injury.
Skull Fractures & Extracranial - Bone Deep & Beyond
- Linear Fracture: Most common, simple break.
- Depressed Fracture: Fragment displaced in; >1 cm depression may need surgery.
- Basilar Fracture: Skull base. Signs: 📌 Battle's sign, Raccoon eyes, CSF leaks (otorrhea/rhinorrhea), hemotympanum.
- Diastatic Fracture: Widens sutures (infants).
- Associated Complications: Vascular injury (MMA tear → EDH), Cranial Nerve (CN) palsy (CN VII/VIII).
- Scalp Hematomas:
- Caput Succedaneum: Edema, crosses sutures, at birth.
- Cephalohematoma: Subperiosteal, respects sutures, hours post-birth.
- Subgaleal: Crosses sutures, large blood loss risk.

⭐ Linear fractures are the most common type of skull fracture.
Intracranial Hemorrhages - The Bleeding Brain
| Feature | Epidural Hematoma (EDH) | Subdural Hematoma (SDH) | Traumatic Subarachnoid Hemorrhage (tSAH) | Intracerebral Hemorrhage (ICH) / Contusion |
|---|---|---|---|---|
| Location | Skull-Dura (potential space) | Dura-Arachnoid (potential space) | Subarachnoid space (sulci, cisterns) | Brain parenchyma |
| CT Appearance | Biconvex (lentiform) 📌 Lemon; hyperdense. Does NOT cross sutures. | Crescentic 📌 Banana; hyperdense (acute), isodense (subacute), hypodense (chronic). CAN cross sutures. | Hyperdense in sulci, cisterns, fissures. | Hyperdense areas; coup/contrecoup injuries. |
| Source | Middle meningeal artery (arterial) | Bridging veins (venous) | Ruptured pial/cortical vessels | Small penetrating arteries/capillaries |
| Key Association | Young, skull fracture, lucid interval | Elderly, alcoholics, anticoagulation, brain atrophy | Most common traumatic bleed | Direct impact, acceleration-deceleration |
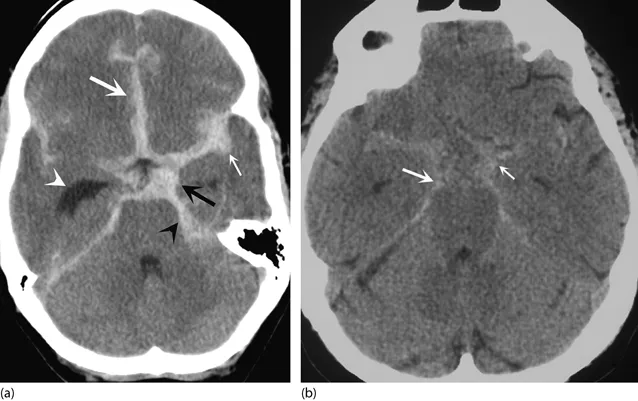
- General CT Signs: Assess for mass effect (sulcal/ventricular effacement) and midline shift (significant if >5mm).
- Intraventricular Hemorrhage (IVH): Blood within ventricles. Often indicates severe injury and poorer prognosis. Can be an extension from tSAH or ICH.
- CT Density: Acute blood is hyperdense (~60-80 HU).
Parenchymal Injury & Herniation - Brain Bruises & Squeezes
- Diffuse Axonal Injury (DAI):
- Mechanism: Shearing (acceleration-deceleration).
- Locations: Grey-white matter junction, corpus callosum, brainstem.
- CT: Often normal or tiny petechiae. MRI (T2/FLAIR, SWI) best for lesions.
⭐ MRI, especially SWI/GRE sequences, is far more sensitive than CT for detecting DAI.
- Cerebral Edema: CT shows loss of grey-white differentiation, sulcal effacement.
- Raised ICP Signs (CT): Effaced sulci/cisterns, compressed ventricles (slit-like), midline shift.
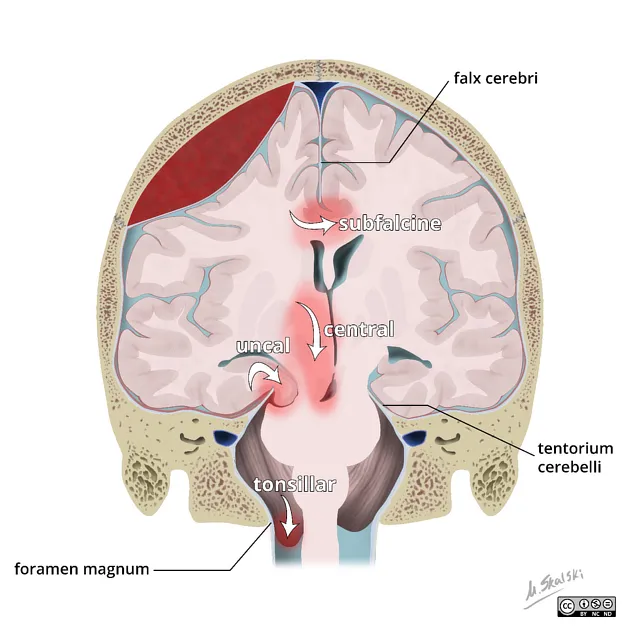
- Herniation Syndromes:
- Subfalcine: Cingulate gyrus under falx → midline shift; ACA compression risk.
- Uncal (Transtentorial): Medial temporal lobe (uncus) through tentorial incisura → ipsilateral CN III palsy (dilated pupil), contralateral hemiparesis (Kernohan's notch).
- Tonsillar: Cerebellar tonsils >5 mm below foramen magnum → brainstem compression, cardiorespiratory compromise (Cushing's triad).
 diagrams and MRI of Diffuse Axonal Injury (DAI))
diagrams and MRI of Diffuse Axonal Injury (DAI))
High‑Yield Points - ⚡ Biggest Takeaways
- NCCT Head is initial choice for acute head trauma.
- EDH: Lentiform, arterial, not crossing sutures. Lucid interval is key.
- SDH: Crescentic, venous, crosses sutures, respects dural folds.
- Traumatic SAH: Blood in sulci/cisterns. Consider CTA for vascular injury.
- DAI: Shearing injury; CT often normal, MRI superior. Look for punctate lesions.
- Signs of ↑ICP: Effaced sulci, compressed ventricles, midline shift >5mm.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

