Trauma Triage Imaging - First Look Wins
ATLS® guides initial imaging in chest trauma. Speed is critical.
- Portable Supine CXR (AP view): Essential first screen. Detects gross pneumothorax, hemothorax, major fractures.
- Limitations: Lower sensitivity for subtle injuries.
- eFAST: Rapid bedside ultrasound. Key for pneumothorax (loss of lung sliding), hemothorax, pericardial tamponade.
- 📌 Remember: "Air, Blood, Fluid around heart".
- MDCT Chest with IV Contrast: Gold standard for stable patients or equivocal findings.
- Definitive evaluation of parenchyma, pleura, mediastinum, vessels.

⭐ In trauma, eFAST has a significantly higher sensitivity (approx. 86-98%) for pneumothorax detection compared to supine CXR (approx. 39-52%).
Pleural & Lung Hits - Air, Blood, Bruises
- Pneumothorax (PTX): Air in pleural space.
- CXR: Visceral pleural line, absent lung markings. Supine: Deep sulcus sign.
- Tension PTX: Mediastinal shift, diaphragm depression.
- CT: Most sensitive for occult PTX.
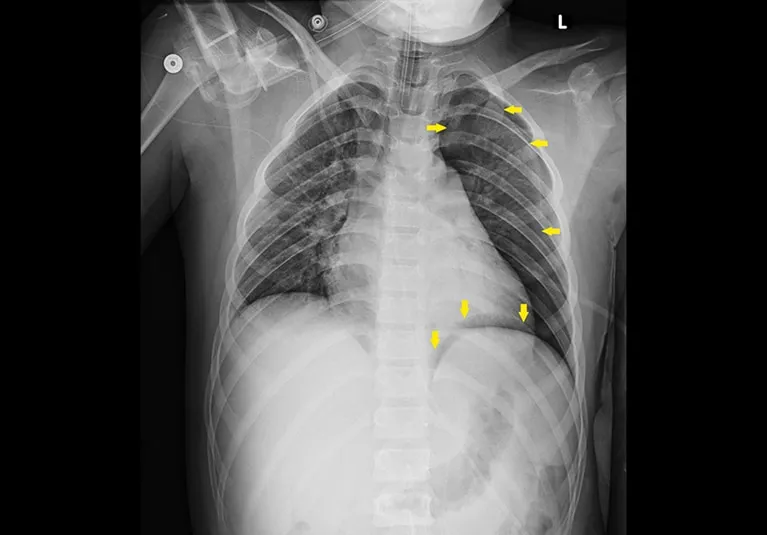
- Hemothorax (HTX): Blood in pleural space.
- CXR: Meniscus sign, opacification.
- CT: Fluid (35-70 HU). Sentinel clot sign (active bleed).
- Massive: >1.5 L initial or >200 mL/hr for 2-4 hrs.
- Pulmonary Contusion: Lung "bruise".
- CXR: Patchy, non-segmental opacities (within 6 hrs, resolves 3-10 days).
- CT: Ground-glass opacities (GGOs), consolidations.
- Pulmonary Laceration: Parenchymal tear.
- CT: Air/blood-filled cavities (traumatic pneumatocele/hematoma). Often with PTX/HTX.
⭐ CT is gold standard for traumatic pleural/parenchymal lung injuries, superior to CXR for sensitivity and specificity.
Mediastinal & Airway Alarms - Central Dangers
- Aortic Injury (High Mortality):
- CXR clues: Widened mediastinum (>8cm), abnormal aortic contour, L apical cap, deviated trachea/NGT.
- CTA (definitive): Intimal flap, pseudoaneurysm, intramural hematoma, active extravasation.

- Tracheobronchial Injury (TBI):
- Location: Typically within 2.5cm of carina.
- Signs: Persistent pneumothorax (despite chest drain), massive subcutaneous emphysema, pneumomediastinum.
- CT: "Fallen lung" sign (pathognomonic), ETT cuff abnormalities.
⭐ The "fallen lung" sign on imaging is highly specific for complete mainstem bronchus transection.
- Esophageal Injury:
- Clues: Pneumomediastinum, pleural effusion (often left), hydropneumothorax, subcutaneous emphysema.
- Diagnosis: Contrast esophagography (Gastrografin, then Barium if no leak/aspiration risk), CT with oral contrast.
- ⚠️ Delayed diagnosis (>24hrs) significantly ↑ mortality.
Wall & Diaphragm Wrecks - Skeletal & Barrier Breaches
-
Rib Fractures: Most common chest skeletal injury.
- 1st-3rd ribs: Risk: major vascular/bronchial injury.
- 9th-12th ribs: Risk: intra-abdominal (liver, spleen) injury.
- 📌 Flail Chest: ≥3 consecutive ribs, ≥2 places each. Paradoxical movement.
-
Sternal Fractures: High-energy trauma. Risk: cardiac/great vessel injury. Lateral CXR or CT best.
-
Scapular Fractures: Indicates severe trauma. Associated: pulmonary contusion, neurovascular injuries.
-
Diaphragmatic Rupture:
- Left more common (~85%); liver protects right. Blunt: large radial tears; Penetrating: small defects.
- CXR signs: Elevated hemidiaphragm, intrathoracic bowel gas/NG tube, "collar sign".
- CT (modality of choice): "Dependent viscera sign", "dangling diaphragm sign", direct tear visualization.
⭐ Diaphragmatic rupture often missed on initial CXR (12-60%), particularly in blunt trauma.
-
Preferred Imaging:
- CXR: Initial survey.
- MDCT with IV contrast: Gold standard for detailed evaluation.
High‑Yield Points - ⚡ Biggest Takeaways
- eFAST for hemothorax/pneumothorax in unstable patients; CT chest with contrast for stable.
- Tension pneumothorax: clinical diagnosis; CXR shows mediastinal shift but don't delay needle decompression.
- Aortic injury CT signs: mediastinal hematoma, abnormal aortic contour, intimal flap.
- Flail chest (≥3 ribs, ≥2 places) indicates severe trauma, often with pulmonary contusion.
- Left diaphragmatic rupture is common; look for bowel in chest on imaging.
- Tracheobronchial injury: suspect with persistent large air leak or subcutaneous emphysema after chest tube placement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

