NSF Introduction - Gadolinium's Dark Fibrosis
- Rare, debilitating, and potentially fatal systemic fibrosing disorder.
- Strongly associated with exposure to Gadolinium-Based Contrast Agents (GBCAs).
- Primarily identified in patients with pre-existing significant renal dysfunction:
- Acute Kidney Injury (AKI).
- Chronic Kidney Disease (CKD) Stage 4 or 5 ($eGFR < \textbf{30} \text{ mL/min/1.73}\text{m}^2$).
- Patients requiring dialysis (hemodialysis or peritoneal).
- Characterized by progressive fibrosis of skin, joints, muscles, and internal organs.
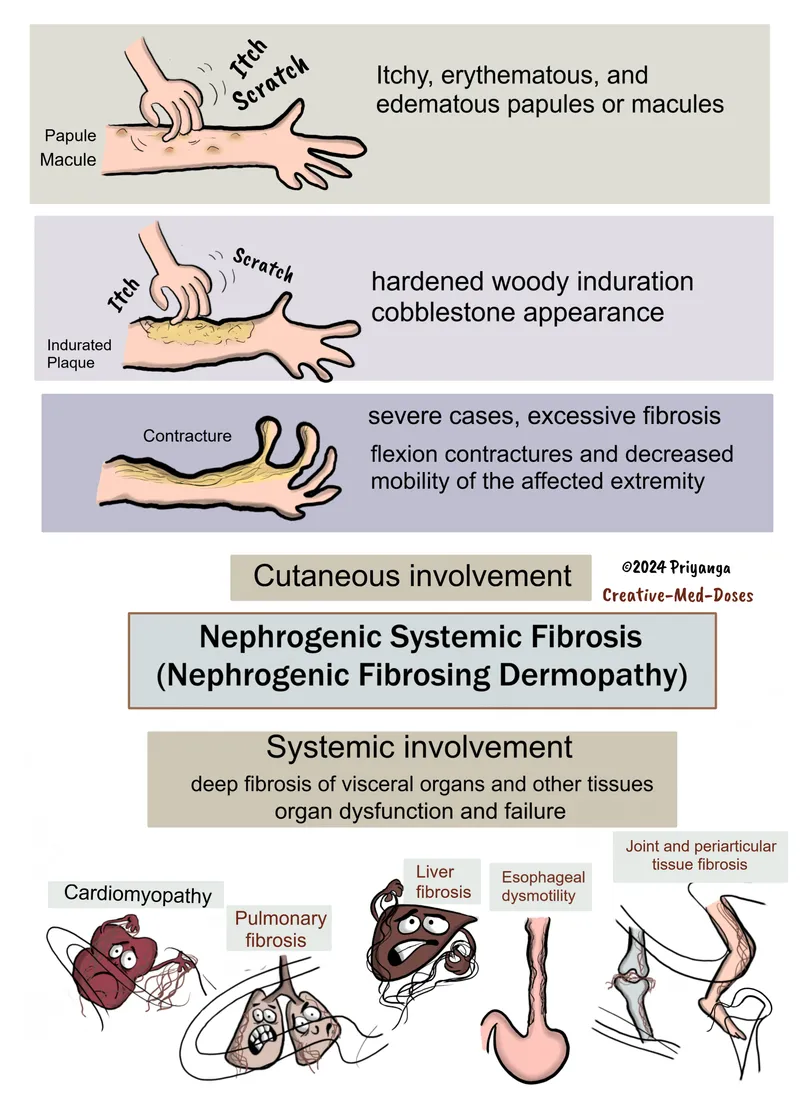
⭐ Most NSF cases are linked to older, group I (linear, higher risk) GBCAs, especially gadodiamide.
Pathogenesis & Risk Factors - Unmasking the Triggers
- Mechanism: Dissociation of Gadolinium (Gd³⁺) from less stable GBCAs (transmetallation) → free Gd³⁺ tissue deposition → recruits circulating fibrocytes (CD34+) → ↑collagen, fibrosis. TGF-β1 implicated.
- Key Risk Factors:
- Renal Impairment (Highest Risk):
- Severe CKD (eGFR < 30 mL/min/1.73m²), AKI.
- Dialysis patients (HD/PD).
- GBCA Type & Dose:
- ↑ Risk: Group I (linear, less stable) GBCAs (e.g., Gadodiamide).
- ↓ Risk: Group II (macrocyclic, more stable) GBCAs.
- High or repeated doses.
- Concurrent Pro-inflammatory States: Sepsis, major surgery, active infection, thrombosis.
- Metabolic acidosis.
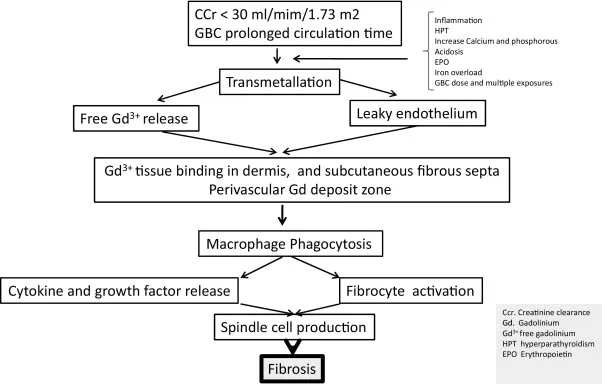
- Renal Impairment (Highest Risk):
⭐ Group I GBCAs (linear) in patients with eGFR < 30 mL/min/1.73m² pose the greatest NSF risk.
Clinical Features & Diagnosis - Spotting the Signs
- Onset: 2-4 weeks (can be days to years) post-GBCA.
- Skin (Key):
- Symmetrical, painful, itchy, red plaques/papules → hard, "woody" skin.
- "Peau d'orange" look.
- Sites: Extremities (spares face), trunk.
- Joint contractures, ↓ mobility.

- Systemic: Fibrosis of lungs, heart, muscles; can be fatal.
- Diagnosis:
- History: GBCA + eGFR < 30 mL/min/1.73m².
- Clinical skin changes.
- Deep skin biopsy: Spindle cells, ↑collagen, mucin, CD34+ fibrocytes, minimal inflammation.
⭐ Strongly linked to Group I GBCAs in severe renal dysfunction (eGFR < 30 mL/min/1.73m²) or AKI.
Prevention & Management - Shielding & Strategies
- Prevention First: 📌 S.A.F.E.R. approach for GBCAs:
- Screen: Identify high-risk (eGFR < 30 mL/min/1.73m², AKI).
- Avoid: Group I GBCAs (e.g., gadodiamide).
- Favour: Group II/III agents (e.g., gadobutrol) if contrast essential.
- Ensure: Lowest effective dose, adequate pre/post-hydration.
- Renal Dialysis Patients: Consider prompt HD (ideally within 2-4 hrs) post-GBCA.
- Management Strategies:
- No definitive cure; supportive & symptomatic focus.
- Physiotherapy: For contractures, skin changes.
- Pain management.
- Experimental: Extracorporeal Photopheresis (ECP), sodium thiosulfate.
- Renal transplant: May halt/improve.
⭐ The cornerstone of NSF prevention is strict avoidance of Group I GBCAs in patients with eGFR < 30 mL/min/1.73m².
High‑Yield Points - ⚡ Biggest Takeaways
- Nephrogenic Systemic Fibrosis (NSF) is strongly linked to gadolinium-based contrast agents (GBCAs), especially older, less stable Group I GBCAs.
- Primarily affects patients with severe renal dysfunction (eGFR < 30 mL/min/1.73m²), particularly those on dialysis.
- Characterized by progressive, painful skin thickening and hardening, often on extremities, leading to joint contractures.
- Can involve systemic fibrosis affecting internal organs like lungs, heart, and muscles.
- No definitive cure exists; management focuses on improving renal function (e.g., kidney transplant) and physiotherapy.
- Prevention is crucial: screen for renal impairment; avoid GBCAs in high-risk patients or use safer Group II/III GBCAs cautiously.
- Deep skin biopsy showing spindle cells, thickened collagen bundles, and elastic fibers confirms diagnosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

