UCA Basics - Bubble Power!
- Definition: Gas-filled microbubbles (1-10 µm diameter) that enhance ultrasound signals.
- Purpose: Improve visualization of blood flow, vascularity, and tissue perfusion by ↑ acoustic backscatter.
- Mechanism: Microbubbles resonate (expand/contract) with ultrasound waves, producing strong echoes and ↑ blood echogenicity.
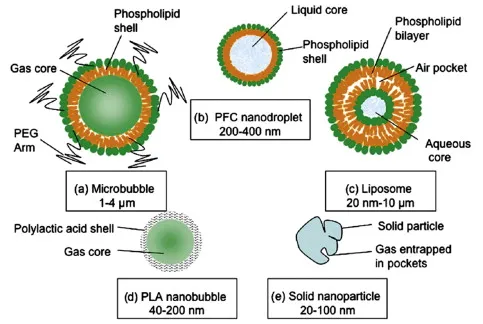
- Composition: Inert gas core (e.g., perfluorocarbon, $SF_6$) stabilized by a biocompatible shell (lipid, albumin, or polymer).
- Administration: Intravenous injection.
⭐ UCAs are purely intravascular agents and do not extravasate into the interstitium in normal conditions.
UCA Types - Gas & Shell Game
- Gas Core: Determines echogenicity & persistence.
- 1st Gen (e.g., Levovist): Air, Nitrogen (less stable, rapid diffusion).
- 2nd Gen (e.g., SonoVue, Definity, Optison): Perfluorocarbons (PFCs), Sulfur Hexafluoride ($SF_6$) (high MW, low solubility → ↑stability, ↑persistence).
- Shell Material: Stabilizes bubble, influences biocompatibility.
- Lipids (phospholipids): Flexible, common (e.g., SonoVue, Definity).
- Proteins (albumin): e.g., Optison.
- Polymers: Less common.
⭐ Second-generation UCAs utilize high molecular weight, poorly soluble gases like perfluorocarbons (e.g., sulfur hexafluoride, SF6) encapsulated in a flexible shell, leading to increased stability and persistence in circulation.
UCA PK & Safety - Bubble Journey
- Administration & Distribution:
- IV injection; strictly intravascular (blood pool agents).
- Do not cross intact capillary walls.
- Elimination ("Bubble Fate"):
- Gas Core: Exhaled via lungs.
- Shell: Metabolized (liver/RES) or renal excretion.
- Safety & Adverse Effects:
- Generally safe; well-tolerated.
- Mild/transient reactions common (headache, nausea).
- Serious reactions (e.g., anaphylaxis) rare (<0.01%).
- Contraindications:
- Known hypersensitivity.
- Severe/unstable cardiopulmonary disease.
- Significant right-to-left cardiac shunts.
- ⚠️ Mechanical Index (MI): Keep low to avoid bubble destruction & potential bioeffects.
⭐ The gas component of UCAs is eliminated primarily via exhalation through the lungs, while the shell material is metabolized by the liver or reticuloendothelial system.
UCA Applications - Bubble Vision!
Contrast-Enhanced Ultrasound (CEUS) revolutionizes imaging by visualizing microvasculature.
- Liver Lesion Characterization:
- Differentiates benign vs. malignant focal liver lesions (FLLs).
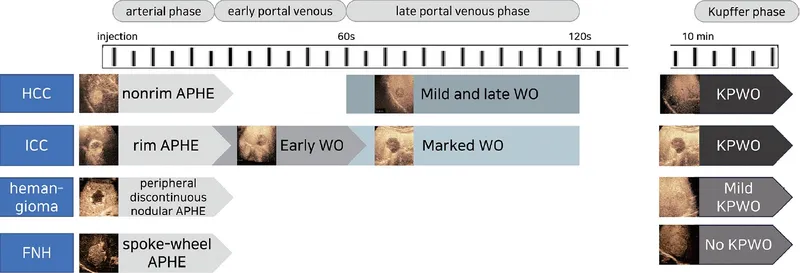
- HCC: Arterial Phase Hyperenhancement (APHE), late washout.
- Metastases: Rim APHE, rapid washout.
- Hemangioma: Peripheral nodular enhancement, centripetal fill.
⭐ In Contrast-Enhanced Ultrasound (CEUS) for focal liver lesions, hepatocellular carcinoma (HCC) typically shows arterial phase hyperenhancement (APHE) followed by late (portal venous or delayed phase) washout.
- Renal Applications:
- Characterizes complex renal cysts (Bosniak classification).
- Evaluates renal masses, esp. with contrast allergy/renal failure.
- Vascular Imaging:
- Detects endoleaks post-EVAR.
- Assesses carotid plaque neovascularization.
- Other Key Uses:
- Splenic & pancreatic imaging.
- Guidance for biopsies/ablations.
- Echocardiography (left ventricular opacification).
High‑Yield Points - ⚡ Biggest Takeaways
- Ultrasound contrast agents (UCAs) are gas-filled microbubbles with a stabilizing shell.
- They are strictly intravascular, enhancing blood pool and perfusion imaging.
- Key use: characterization of focal liver lesions (e.g., FNH, HCC).
- Improves Doppler signals and lesion detection/conspicuity.
- Also used in echocardiography (LVO, myocardial perfusion) and vascular imaging.
- Contraindicated in severe pulmonary hypertension and right-to-left shunts.
- Second-generation UCAs offer improved stability and duration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

