Definition & Incidence - Kidney Contrast Chaos
- Definition: Acute Kidney Injury (AKI) occurring after intravascular contrast media (CM) administration, characterized by:
- Serum creatinine ($SCr$) absolute increase $\ge \textbf{0.3 mg/dL}$ OR
- $SCr$ percentage increase $\ge \textbf{25-50%}$ from baseline.
- Typically occurs within $\textbf{48-72 hours}$ post-CM exposure.
- Requires exclusion of other nephrotoxic insults.
- Incidence:
- General population with normal renal function: <2%.
- High-risk patients (e.g., pre-existing CKD, diabetes): 10-30%, can reach up to 50%.
⭐ CIN is a significant cause of hospital-acquired AKI, often cited as the third leading cause.
Pathophysiology - How Contrast Harms
- Primary Mechanisms:
- Direct Tubular Toxicity:
- Contrast media (CM) directly injures proximal tubular cells.
- Generation of Reactive Oxygen Species (ROS) → oxidative stress.
- Osmotic load → tubular cell swelling (osmotic nephrosis).
- Renal Medullary Hypoxia:
- Intrarenal vasoconstriction (↓ Renal Blood Flow, RBF), mediated by adenosine, endothelin.
- Increased blood viscosity.
- Reduced O₂ delivery to the vulnerable outer medulla (high metabolic activity).
- Leads to medullary ischemia, inflammation, and Acute Tubular Necrosis (ATN).
- Direct Tubular Toxicity:
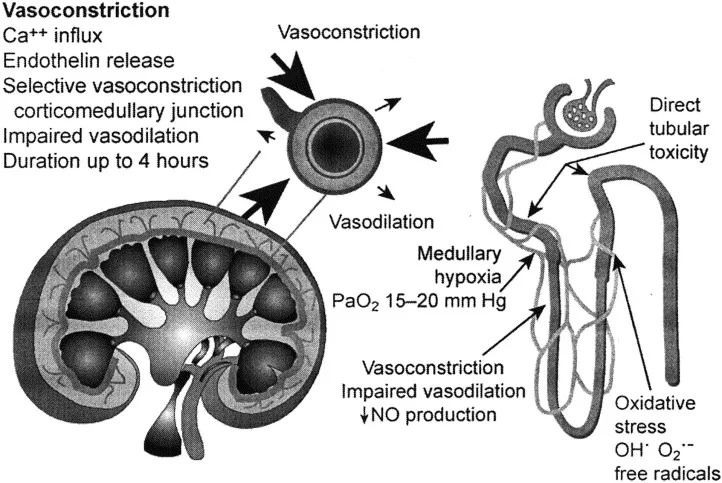
⭐ The renal medulla is particularly susceptible to CIN due to its marginal oxygen supply relative to its high metabolic demand for solute transport.
Risk Factors & Stratification - Danger Zones
| Category | Risk Factor | Key Detail / Threshold |
|---|---|---|
| Patient | Pre-existing CKD | eGFR <60 mL/min/1.73m² (Most critical) |
| Diabetes Mellitus | Especially with nephropathy | |
| Age | >75 years | |
| Volume Depletion | (Hypovolemia) | |
| Severe CHF | NYHA Class III/IV | |
| Nephrotoxic Drugs | e.g., NSAIDs, Aminoglycosides | |
| Procedure | Contrast Volume | High (e.g., >4 mL/kg or >100-125 mL) |
| Contrast Type | HOCM > LOCM > IOCM (risk ↓) | |
| Route | Intra-arterial > IV | |
| Repeat Exposure | <72 hrs between studies |
Prevention Strategies - Shield Up!
- Hydration:
- Isotonic saline (0.9% NaCl): 1-1.5 mL/kg/h (3-12h pre, 6-24h post).
- Oral hydration if IV unfeasible. 📌 Mnemonic: "Hydrate right, CIN takes flight!"
- Contrast Media:
- Use Low-Osmolar (LOCM) or Iso-Osmolar (IOCM).
- Minimize volume.
- Medications:
- N-acetylcysteine (NAC): 600-1200 mg PO BID x2d (pre/day of); benefit debated.
- Hold nephrotoxins (e.g., NSAIDs) 24-48h prior.
⭐ Hold metformin 48h post-contrast if eGFR < 30 mL/min/1.73m² or AKI; restart after stable renal function.
Clinical Features & Management - Rescue & Recovery
- Clinical: Usually non-oliguric AKI.
- Serum creatinine (SCr) begins to rise 24-48 hours post-contrast.
- SCr peaks at 3-5 days.
- SCr typically normalizes within 7-10 days.
- Urine output is often maintained.
- Management (Rescue & Recovery):
- Supportive care is the mainstay.
- Maintain euvolemia; monitor fluid balance carefully.
- Track SCr, BUN, and electrolytes.
- Avoid additional nephrotoxic agents (e.g., NSAIDs).
- Renal Replacement Therapy (RRT) is rarely required, reserved for severe AKI.
⭐ In CIN, serum creatinine characteristically peaks 3-5 days after contrast administration and usually returns to baseline within 7-10 days if no other renal insult occurs.
High‑Yield Points - ⚡ Biggest Takeaways
- CIN is AKI occurring 48-72 hours post-contrast, defined by ↑ serum creatinine (≥0.5 mg/dL or ≥25% from baseline).
- Major risk factors: Pre-existing CKD (eGFR <60 mL/min/1.73m²), diabetes mellitus, dehydration, and large contrast volume.
- Pathogenesis involves direct tubular toxicity and renal vasoconstriction, leading to medullary hypoxia.
- Prevention is paramount: IV hydration (isotonic saline), use low-osmolar or iso-osmolar contrast media, and minimize contrast dose.
- Most cases are transient, non-oliguric, and resolve with supportive care; dialysis is rarely needed.
- Serum creatinine typically peaks at 3-5 days and returns to baseline within 1-3 weeks in most patients.
- Avoid NSAIDs and other nephrotoxic agents around the time of contrast administration in high-risk patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

