Radiographic Signs in Chest Imaging - Border Patrol Signs
- Silhouette Sign:
- Principle: Border loss between same-density structures.
- Localizes: Pathology to lobe/segment by obscuring heart, aorta, diaphragm.
⭐ The Silhouette sign, based on the loss of normal radiographic interface, is invaluable for localizing pathology adjacent to structures like the heart or diaphragm.
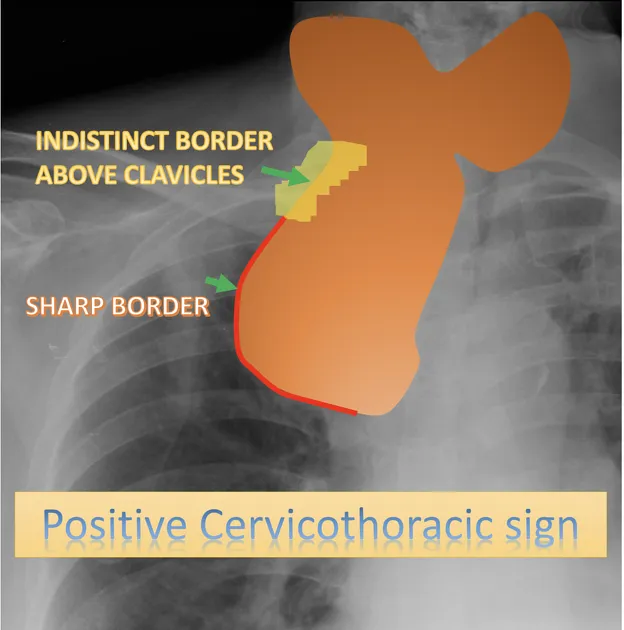
- Cervicothoracic Sign:
- Principle: Lesions above clavicles: sharp border = posterior; indistinct = anterior.
- Differentiates: Anterior vs. posterior mediastinal/neck masses.
- Thoracoabdominal Sign:
- Principle: Mass sharp through diaphragm = thoracic; obscured = abdominal.
- Differentiates: Intrathoracic vs. abdominal masses near diaphragm.
- Hilum Overlay Sign:
- Principle: Hilar vessels seen through mass = mass not hilar (anterior/posterior).
- Differentiates: Hilar vs. non-hilar masses.
Radiographic Signs in Chest Imaging - Lung Lucency Lore
- Air Bronchogram Sign
- Appearance: Branching air-filled bronchi against opaque, consolidated lung.
- Pathology: Alveolar opacification (pneumonia, edema) with patent airways.
- Location: Any affected lobe.
- Golden S Sign (of Felson)
- Appearance: Reverse 'S' on CXR; convex minor fissure, concave central mass.
- Pathology: RUL collapse due to a central obstructing mass.
- Location: RUL.
⭐ The Golden S sign, a reverse S-shape on frontal chest X-ray, strongly suggests a right upper lobe collapse due to a central mass.
- Luftsichel Sign
- Appearance: Crescent lucency (hyperinflated superior LLL segment) around aortic arch.
- Pathology: LUL collapse, often due to central mass.
- Location: LUL.
Radiographic Signs in Chest Imaging - Lining & Air Leaks
-
Deep Sulcus Sign
- Appearance: Deep, lucent costophrenic angle on supine CXR, extending inferiorly.
- Significance: Indicates pneumothorax in a supine patient.
-
Continuous Diaphragm Sign
- Appearance: Diaphragm visible continuously from one side to other beneath heart.
- Significance: Pneumomediastinum (air in mediastinum).
⭐ The Continuous Diaphragm sign, where air outlines the entire undersurface of the diaphragm, is a key indicator of pneumomediastinum.
-
Fallen Lung Sign
- Appearance: Lung falls away from hilum, often towards diaphragm/posteriorly.
- Significance: Suggests bronchial fracture or transection.
-
Split Pleura Sign
- Appearance: Thickened visceral and parietal pleura clearly separated by pleural fluid.
- Significance: Highly suggestive of empyema (exudative effusion).
Radiographic Signs in Chest Imaging - Clot & Infarct Clues
-
Hampton Hump:
- Appearance: Peripheral wedge-shaped opacity, pleural-based, apex towards hilum.
- Pathophysiology: Pulmonary infarction due to Pulmonary Embolism (PE).
-
Westermark Sign:
- Appearance: Regional oligemia (↓ vascular markings) distal to embolus.
- Pathophysiology: Pulmonary Embolism (PE) causing ↓ blood flow.
⭐ Westermark sign, representing regional oligemia distal to a pulmonary embolus, is a specific but insensitive sign of PE.
-
Fleischner Sign (Knuckle Sign):
- Appearance: Prominent/distended central pulmonary artery, proximal to embolus.
- Pathophysiology: Large PE; pulmonary hypertension.
-
Palla's Sign:
- Appearance: Enlarged ("sausage-shaped") right descending pulmonary artery.
- Pathophysiology: Large embolus in right descending pulmonary artery (PE).
Radiographic Signs in Chest Imaging - Cavity Chronicles
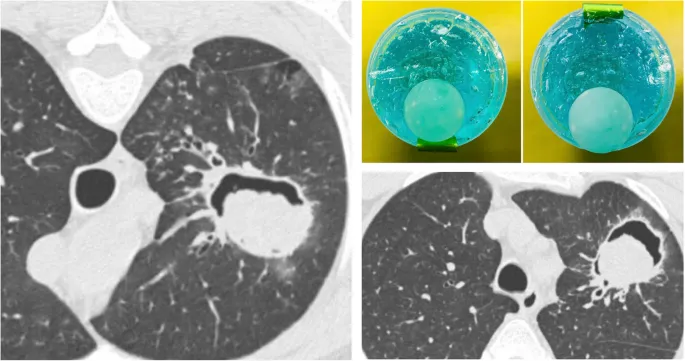
- Water Lily Sign (Sign of the Camalote):
- Appearance: Detached endocyst membranes floating within a hydatid cyst.
- Cause: Ruptured pulmonary hydatid cyst (Echinococcus granulosus).
⭐ The Water Lily sign, representing detached endocyst membranes floating in a hydatid cyst, is pathognomonic for a ruptured pulmonary hydatid cyst.
- Monod Sign:
- Appearance: Air surrounding a mobile fungal ball (mycetoma) within a pre-existing cavity.
- Cause: Aspergilloma (Aspergillus).
- Air Crescent Sign:
- Appearance: Crescent of air in nodule periphery, separating wall from necrotic core.
- Cause: Invasive aspergillosis (angioinvasion), TB.
- Comet Tail Sign (Rounded Atelectasis):
- Appearance: Curved vessels & bronchi converging towards a peripheral rounded opacity.
- Cause: Asbestos-related pleural disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Silhouette sign: Loss of border indicates lesion is contiguous with the structure.
- Air bronchograms: Visible bronchi within consolidation, confirms intrapulmonary location.
- Golden S sign: S-shape on frontal CXR suggests RUL collapse with a central mass.
- Hampton"s hump: Pleural-based wedge opacity, points to pulmonary infarction in PE.
- Deep sulcus sign: Increased lucency of costophrenic angle in supine pneumothorax.
- Continuous diaphragm sign: Air outlining diaphragm, indicates pneumomediastinum or pneumopericardium.
- Bat wing/Butterfly pattern: Bilateral perihilar opacities, classic for pulmonary edema.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

