Bacterial Pneumonias - Bugs & Blobs
- Lobar Pneumonia:
- Organism: Streptococcus pneumoniae (most common)
- Pattern: Homogeneous consolidation (lobe/segment)
- X-ray/CT: Dense opacity, air bronchograms.

- Bronchopneumonia (Patchy):
- Organisms: Staphylococcus aureus, Haemophilus influenzae, Pseudomonas aeruginosa, Klebsiella pneumoniae
- Pattern: Patchy, segmental, or lobular consolidation
- X-ray/CT: Multiple foci of opacity, often bilateral, peribronchial thickening.
- Atypical Pneumonia (Interstitial):
- Organisms: Mycoplasma pneumoniae, Legionella pneumophila, Chlamydia pneumoniae
- 📌 Mnemonic: "My Lungs Cough" (Mycoplasma, Legionella, Chlamydia)
- Pattern: Interstitial infiltrates (reticular, reticulonodular)
- X-ray/CT: Ground-glass opacities, fine reticular markings.
- Organisms: Mycoplasma pneumoniae, Legionella pneumophila, Chlamydia pneumoniae
⭐ Streptococcus pneumoniae is the most common cause of community-acquired lobar pneumonia, classically presenting with consolidation in a single lobe and air bronchograms.
Viral & Fungal Pneumonias - Hazy Invaders
- Viral Pneumonias:
- Influenza: Non-specific bilateral infiltrates.
- COVID-19: Peripheral, bilateral Ground-Glass Opacities (GGOs); "crazy-paving" pattern.
- Fungal Pneumonias:
- Pneumocystis jirovecii Pneumonia (PJP):
- Bilateral, perihilar GGOs ("batwing" appearance).

⭐ In immunocompromised patients, especially with HIV and CD4 count < 200 cells/µL, PJP classically presents with bilateral, diffuse, symmetrical perihilar GGOs.
- Bilateral, perihilar GGOs ("batwing" appearance).
- Aspergilloma:
- Fungus ball within a pre-existing lung cavity.
- Invasive Aspergillosis (immunocompromised):
- "Halo sign" (early).
- "Air crescent sign" (later, with neutrophil recovery).
- Pneumocystis jirovecii Pneumonia (PJP):
Pulmonary Tuberculosis - The Great Mimicker
- Primary TB: Often asymptomatic; immune response contains infection.
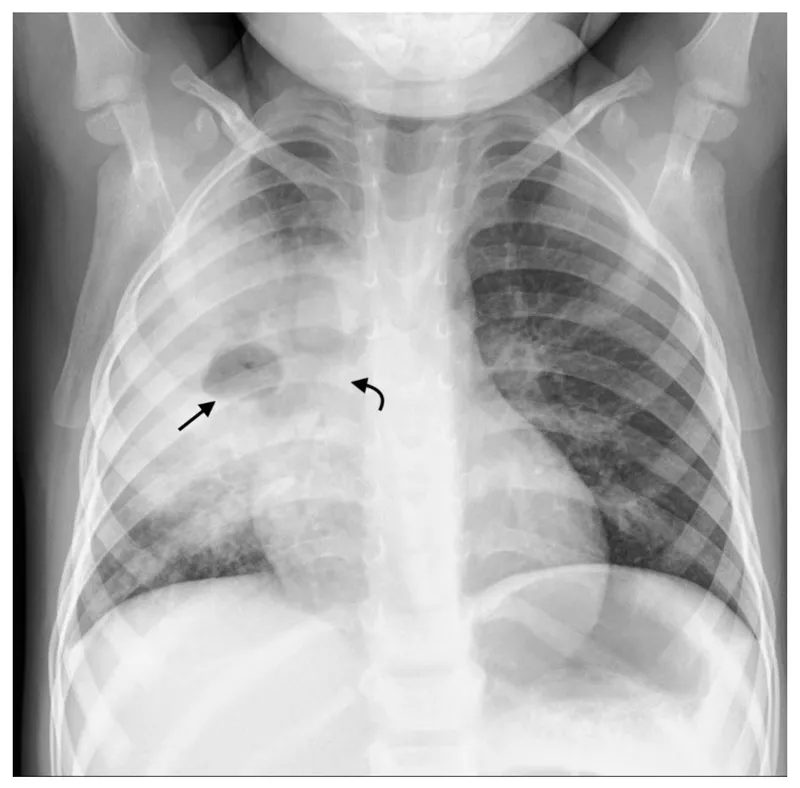
- Ghon focus: Initial lung lesion (calcified peripheral nodule).
- Ranke complex: Ghon focus + ipsilateral hilar/paratracheal lymphadenopathy (often calcified).
- Lymphadenopathy: Hilar/paratracheal, can cause airway compression in children.
- Post-primary (Reactivation) TB: Symptomatic; reactivation of latent infection.
- Predilection: Apical/posterior segments of upper lobes, superior segments of lower lobes.
- Key findings: Cavitation, fibrocalcific changes (scarring), Rasmussen aneurysm (rare, pulmonary artery pseudoaneurysm within cavity).
- Miliary TB: Hematogenous dissemination.
- Key findings: Diffuse, bilateral millet-seed (1-2 mm) opacities on CXR.

- Key findings: Diffuse, bilateral millet-seed (1-2 mm) opacities on CXR.
⭐ Post-primary (reactivation) tuberculosis most commonly affects the apical and posterior segments of the upper lobes or the superior segments of the lower lobes, often leading to cavitation.
Infection Patterns & Complications - Reading Between Lines
Key radiological signs:
- Silhouette Sign: Lost lung-soft tissue interface. Seen in: Consolidation.
- Air Bronchogram: Patent bronchi in opaque lung. Seen in: Pneumonia.
- Tree-in-bud Sign: Centrilobular nodules, branching lines. Seen in: Endobronchial spread (TB, MAC).
⭐ The tree-in-bud sign on CT, representing centrilobular bronchiolar dilatation and impaction, is highly suggestive of endobronchial spread of infection, commonly seen in tuberculosis or atypical mycobacterial infections.
- Halo Sign: GGO around nodule/mass. Seen in: Invasive Aspergillosis.
- Air Crescent Sign: Air in cavity, around sequestrum. Seen in: Invasive Aspergillosis (recovery).
- Reversed Halo (Atoll) Sign: Central GGO, peripheral consolidation ring. Seen in: COP, fungal, TB.
Major Complications:
- Lung Abscess: Thick-walled (>2mm) cavity, air-fluid level.
- Empyema: Pleural pus; split pleura sign.
- ARDS: Bilateral diffuse opacities (white-out); normal heart size.
Approach to Patterns:
High‑Yield Points - ⚡ Biggest Takeaways
- Lobar pneumonia: Typically S. pneumoniae; presents as lobar consolidation with air bronchograms.
- Post-primary TB: Favors apical/posterior segments of upper lobes; shows cavitation and fibrosis.
- PJP: In immunocompromised patients; bilateral, diffuse perihilar ground-glass opacities.
- Aspergilloma: A fungus ball (mycetoma) developing in a pre-existing lung cavity.
- Atypical pneumonia (Mycoplasma): Characterized by diffuse reticulonodular or interstitial patterns.
- Viral pneumonia: Often presents with bilateral, diffuse ground-glass opacities or interstitial infiltrates.
- Bronchopneumonia: Manifests as patchy, segmental consolidations, often multilobar.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

