Normal Post-Op Appearance - Surgical Skyline Shifts
- Pneumonectomy:
- Immediate: Hemithorax air-filled; mediastinum midline.
- Days-Weeks: Progressive fluid accumulation (air-fluid level). Mediastinum shifts slightly towards operated side as fluid replaces air.
⭐ Post-pneumonectomy space fluid: ~1-2 rib spaces/day or 50-250 mL/day initially. Full opacification by 3-6 months.
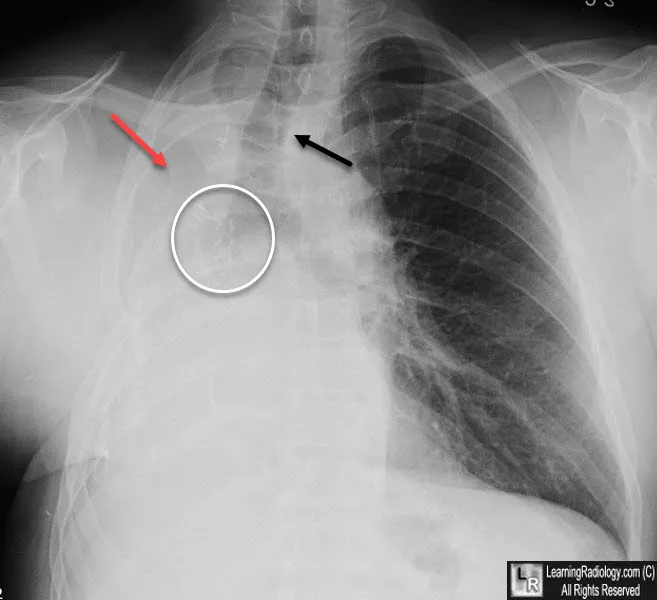
- Late (Months): Complete opacification. Marked mediastinal shift towards surgical side. Ipsilateral hemidiaphragm ↑. Contralateral lung hyperinflation. Ribs approximated.
- Lobectomy:
- Remaining lobe(s) hyperinflate, partially filling void.
- Mediastinal structures (trachea, heart) shift moderately towards surgical side.
- Ipsilateral hemidiaphragm ↑. Transient pleural effusion; staple lines.
- Segmentectomy/Wedge Resection:
- Minimal architectural distortion: Local scarring, staple lines.
- Typically no significant mediastinal or diaphragmatic position changes.
Early Complications - Immediate Post-Op Pitfalls
- Pneumothorax:
- Common; tension (mediastinal shift) is ⚠️ emergency!
- Intervention if symptomatic or >2-3 cm.
- Hemothorax/Hemorrhage:
- ↑Drain output, ↓BP, ↑HR.
- Opacification on CXR; CT defines extent.
- Atelectasis:
- Most frequent; lobar/segmental collapse.
- Due to pain, mucus plugs.
- Surgical Emphysema:
- Subcutaneous air; usually benign.
- Extensive may compromise airway.
- Chylothorax:
- Milky pleural fluid (thoracic duct injury).
- Bronchopleural Fistula (BPF):
- Persistent air leak; new/worsening pneumothorax.
- Acute Lung Injury/ARDS:
- Diffuse bilateral opacities, severe hypoxemia.
⭐ Atelectasis is the most common early post-thoracotomy complication.
Late/Specific Complications - Long-Term Lurkers
-
Bronchopleural Fistula (BPF)
- Abnormal airway-pleural connection; often late post-pneumonectomy.
- CXR: New/↑ pneumothorax, new/↑ air-fluid level in pleural space, "falling lung sign".
- CT: Definitive. Shows fistulous tract, air bubbles in pleural fluid.
⭐ Key CT sign: Direct visualization of a fistulous tract from the airway to the pleural space, or persistent air bubbles within a pleural fluid collection (especially after chest tube removal).
- 📌 BPF Signs Mnemonic: AFLAT - Air leak (persistent), Fluid (new/↑ air-fluid level), Lung collapse (falling), Air bubbles (CT), Tract (CT).
-
Empyema
- Pus in pleural space; presents as loculated effusion.
- CT: "Split pleura sign" (thickened, enhancing visceral & parietal pleura separated by fluid); differentiates from sterile effusion. Gas bubbles may be present.
-
Post-Pneumonectomy Syndrome (PPS)
- Late complication (months-years) due to extreme mediastinal shift/rotation causing airway (trachea/main bronchus) compression. More common post-right pneumonectomy.
- Symptoms: Dyspnea, stridor.
- CT: Confirms airway compression between sternum/great vessels and vertebral column.
-
Chronic Post-Thoracotomy Pain Syndrome (CPTPS)
- Persistent pain >2-3 months post-surgery, typically neuropathic (intercostal nerve).
- Imaging: Usually normal; used to exclude other causes (e.g., infection, tumor recurrence).
-
Esophagopleural Fistula (EPF)
- Connection between esophagus and pleural space.
- CXR: Hydropneumothorax, pleural effusion (often left-sided).
- Contrast swallow (Gastrografin first) / CT with oral contrast: Demonstrates leak into pleural space.
Imaging Modalities & Signs - Detective's Diagnostic Devices
- CXR (Chest X-ray):
- Initial check: lines, tubes, pneumothorax, effusion, atelectasis.
- Portable for immediate post-op monitoring.
- CT Scan:
- Definitive for complications: abscess (rim-enhancing), hematoma, empyema.
- CTA for PE, vascular injury.
⭐ CT is the modality of choice for suspected mediastinal fluid collection post-CABG.
- USG (Ultrasound):
- Guides drainage (pleural/pericardial effusion).
- Assesses diaphragmatic movement. Portable, radiation-free.
Key Post-Op Signs:
- Pneumothorax: Visceral pleural line, absent lung markings.
- Effusion: Meniscus sign, blunted costophrenic angle.
- Atelectasis: Opacification, volume loss (e.g., fissure displacement). oka
High‑Yield Points - ⚡ Biggest Takeaways
- Pneumothorax is common; tension pneumothorax is an emergency.
- Pleural effusions are expected; monitor for rapid increase, hemothorax, or empyema.
- Surgical emphysema is usually benign; extensive forms need evaluation.
- Mediastinal widening on CXR prompts CT for hematoma or mediastinitis.
- Atelectasis is frequent: linear opacities, volume loss.
- Post-op pneumonia: new consolidations; differentiate from atelectasis.
- Check sternal wires and hardware for malposition or fracture.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

