Pleural Effusions - Water Woes
- Types & Causes:
- Transudate: ↑ hydrostatic or ↓ oncotic pressure (CHF, cirrhosis, nephrotic).
- Exudate: ↑ pleural permeability (pneumonia, malignancy, TB, PE).
- Light's Criteria (Exudate if ≥1): (📌 5-6-2/3)
- Pleural Fluid Protein/Serum Protein > 0.5
- Pleural Fluid LDH/Serum LDH > 0.6
- Pleural Fluid LDH > 2/3 Upper Limit of Normal Serum LDH.
- Imaging:
- CXR: Costophrenic angle (CPA) blunting (>200ml), meniscus sign, subpulmonic effusion, vanishing tumor (fissural). Lateral decubitus: confirms free fluid.
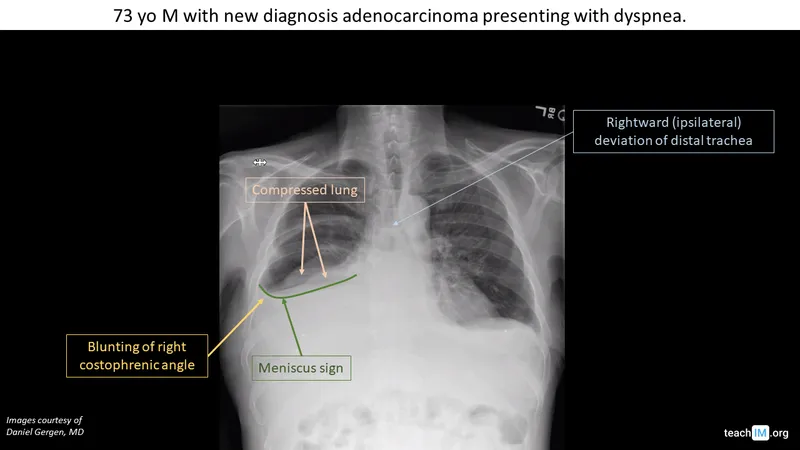
- USG: Anechoic (transudate) vs. complex/septated (exudate); ideal for thoracentesis guidance.
- CT: Loculations, pleural enhancement, underlying lung pathology.
- CXR: Costophrenic angle (CPA) blunting (>200ml), meniscus sign, subpulmonic effusion, vanishing tumor (fissural). Lateral decubitus: confirms free fluid.
⭐ A subpulmonic effusion can mimic an elevated hemidiaphragm; a lateral decubitus X-ray showing layering of fluid is key for confirmation.
Pneumothorax - Air Scare
- Types:
- Spontaneous:
- Primary: No underlying lung disease (e.g., ruptured apical blebs in tall, thin males)
- Secondary: With underlying lung disease (e.g., COPD, TB, cystic fibrosis)
- Traumatic: Due to penetrating or blunt chest trauma
- Iatrogenic: Resulting from medical procedures (e.g., central line insertion, lung biopsy)
- Spontaneous:
- CXR Signs:
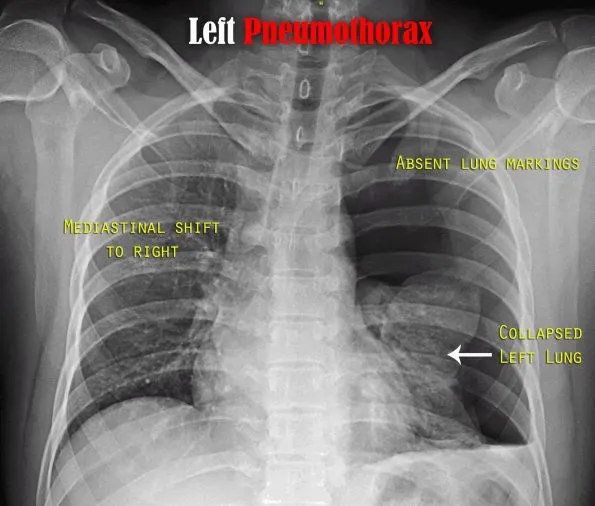
- Visible visceral pleural line (sharp white line of the collapsed lung edge)
- Absent peripheral lung markings beyond the pleural line
- Expiratory films: May enhance visibility of small pneumothoraces
- Deep sulcus sign: On supine CXR, indicates air collection anteroinferiorly, deepening the costophrenic angle
⭐ The 'deep sulcus sign' on a supine chest X-ray is a critical indicator of pneumothorax, especially in trauma or ICU patients.
- Tension Pneumothorax (EMERGENCY!):
- Mediastinal shift (contralateral, away from PTX)
- Diaphragmatic depression (ipsilateral)
- ↑ Hyperlucent hemithorax, widened intercostal spaces
- CT Chest:
- Gold standard for detecting small or loculated pneumothoraces
- Identifies underlying cause (e.g., bullae, blebs, cysts)
Pleural Infections & Thickening - Gunk & Grime
- Parapneumonic Effusion (PPE): Exudate with pneumonia.
- Uncomplicated: Free-flowing; antibiotics.
- Complicated: Loculated; needs drainage.
- Empyema: Pus in pleural space. Criteria:
- pH < 7.20
- Glucose < 60 mg/dL
- LDH > 1000 IU/L
- Positive Gram stain/culture.
- Imaging (Empyema):
- CXR: Lenticular opacity.
- CECT: Split pleura sign, thickened/enhancing pleura, gas.
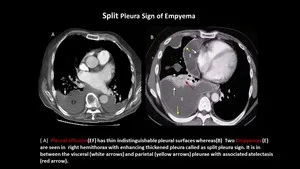
- USG: Loculations, septations; guides drainage.
⭐ 'Split pleura sign' (CECT): thickened, enhancing visceral & parietal pleura separated by complex fluid; highly suggestive of empyema.
- Pleural Thickening Causes: Post-infection (TB), asbestos, post-hemothorax, malignancy.
- Pleural Calcification:
- Asbestos: Parietal/diaphragmatic plaques; spares costophrenic angles/apices.
- TB: Extensive, visceral; 'empyema necessitans' (pus tracks through chest wall).
Pleural Masses - Lumps & Bumps
| Feature | Malignant Mesothelioma | Metastases |
|---|---|---|
| Etiology | Strong asbestos link (long latency) | Most common; Primaries: Lung, breast, lymphoma, ovary |
| Imaging | Nodular/lobulated circumferential thickening, lung encasement, ipsilateral volume ↓, fissure involvement, large effusion | Multiple nodules/plaques, effusion, often bilateral |
| Laterality | Usually unilateral | Often bilateral |
⭐ Malignant mesothelioma typically causes circumferential, nodular pleural thickening that encases the lung, often associated with a history of asbestos exposure and may lead to ipsilateral lung volume loss.
- Solitary Fibrous Tumor of Pleura (SFTP)
- Mostly benign; can be large, pedunculated/sessile.
- Associations:
- Hypoglycemia (Doege-Potter syndrome).
- Hypertrophic osteoarthropathy (Pierre Marie-Bamberger syndrome).
- Lipoma
- Fat density on CT.
High‑Yield Points - ⚡ Biggest Takeaways
- Pleural effusion: Meniscus sign on CXR; Light's criteria for exudate vs. transudate.
- Pneumothorax: Visceral pleural line visible; tension type is an emergency with mediastinal shift.
- Empyema: Loculated pus in pleural space, requires prompt drainage.
- Hemothorax: Blood in pleural cavity, often post-traumatic; CT density >50 HU.
- Mesothelioma: Aggressive tumor linked to asbestos; causes large unilateral effusion, nodular pleural thickening.
- Chylothorax: Milky pleural fluid due to lymph; high triglyceride levels (>110 mg/dL).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

